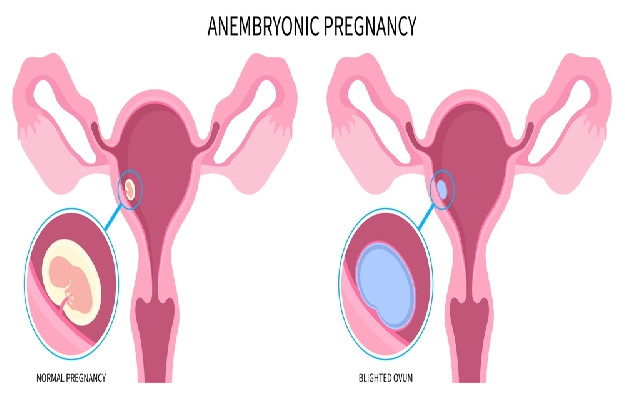
Molar pregnancy or hydatidiform mole is a condition in which a part or whole of the placenta starts to grow unusually. It is a type of gestational trophoblastic disease.
Trophoblasts are the cells that the placenta is made of. Gestational, as you know, is anything pregnancy-related. Trophoblastic disease refers to a group of conditions wherein tumours develop in the womb from the placenta.
Molar pregnancy is an uncommon condition—it affects about 1 in every 800-1,000 pregnancies—and it usually occurs due to a genetic error in the fertilization process. In some cases, there is no development of foetal tissue. In others, miscarriage occurs early in the pregnancy. (Read more: Chemical pregnancy symptoms, causes, treatment)
A woman with a molar pregnancy usually has all the signs of pregnancy. That is why a lot of women do not get to know about them until after a miscarriage. Most women with a molar pregnancy miscarry by the end of the first trimester. However, for some, the mole may also show up on an ultrasound.
Hydatidiform moles are generally not harmful but if left untreated, the affected tissue can spread to other parts of the body (through the blood) including the lungs, brain and liver. In rare cases, it can turn cancerous.
The condition is usually treated through medications and surgery.