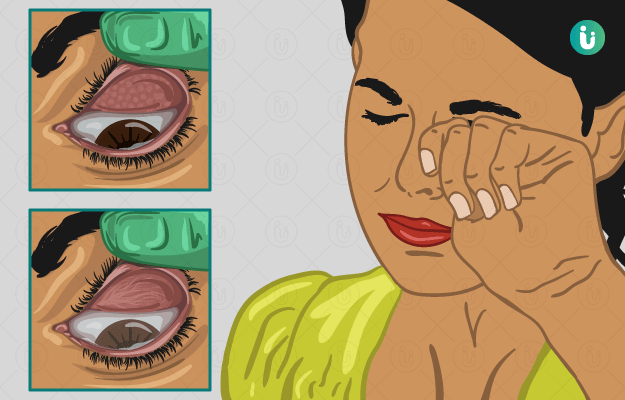
Trachoma is an eye disorder caused by Chlamydia trachomatis infection. It is the most common cause of blindness due to infection in the world.
The infection spreads through contact with the eye discharge, nose discharge or throat discharge of someone with active disease.
The contact can be direct or indirect via fomites (commonly touched surfaces like lift buttons and doorknobs), bedclothes, handkerchiefs and other shared items.
It can also spread via hands, which is why maintaining hand hygiene is crucial to avoid this infection. It is also a good idea to avoid touching your face and eyes, to prevent all kinds of infection.
Flies can also transmit the infection, by transferring eye, nose and throat discharge from infected persons to healthy ones.
In places where there is poor personal hygiene, researchers have also linked the spread of infection among children to dirty faces (because any discharge from the eye stays there for longer).
In places where hygiene is generally poor and the infection is common, infection tends to spread from older family member to younger ones.
Preschool-aged children are the most susceptible to fresh infections.
In places where trachoma is endemic, the chances of repeated infections are very high. While the body is usually equipped to handle one-off infections by Chlamydia trachomatis, repeat infections can scar the inside of the eyelids (trachomatous conjunctival scarring) so they turn inwards. This affects the direction of the eyelashes (trachomatous trichiasis) which, in turn, can scratch and scar the eyeball. People who have had repeated episodes of trachoma infection tend to have increased light sensitivity, eye pain and cornea problems.
Untreated infections can cause blindness, as the scarring of the eye can cause opacities to build up.
In 2017, India declared itself trachoma-free. According to the WHO, though, as of 10 September 2020, only 10 out of 53 countries across Africa, Asia and Central and South America had eliminated trachoma as a public health threat. These countries are Cambodia, China, Islamic Republic of Iran, Lao People’s Democratic Republic, Ghana, Mexico, Morocco, Myanmar, Nepal and Oman. The WHO defines “elimination of trachoma as a public health problem” as meeting the following three criteria:
- Less than 0.2% of the population aged 15 and above has trachomatous trichiasis “unknown to the health system”. That is roughly one case per 1000 total population
- Two years or more in which fewer than 5% of children between one and nine years of age have the first stage of trachoma—trachomatous inflammation-follicular—without resorting to mass treatments with antibiotics. The WHO checks each district where the infection was endemic (present continually at low levels) to validate
- There should be a system in place to identify and manage any cases of trachomatous trichiasis, with properly outlined and funds to prevent the resurgence of infections in the area

 Doctors for Trachoma
Doctors for Trachoma