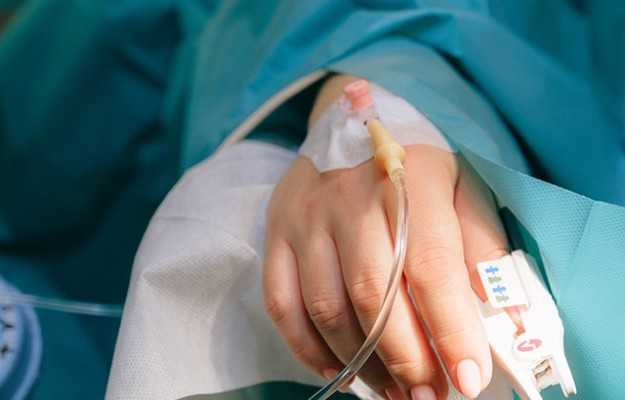
A cannula is a tube that is inserted into the body to perform the function of delivering or removing any bodily fluid or taking samples. A cannula surrounds the inner or outer area of a needle (trocar) and increases the effective length of the needle by half the length of the original needle. It is commonly called an intravenous cannula (IV cannula). Peripheral venous cannulation (cannula inserted directly into the peripheral veins of the body) is the most common method to deliver intravenous therapy. The ultimate goal of intravenous management is to deliver treatment safely and effectively without any major discomfort or damage to tissues and without compromising venous access. This is especially important when long-term treatment is advocated. There are various indications and contraindications for peripheral cannulation; however, research suggests that intravenous cannulas are often inserted in patients when it can easily be avoided. In a recent study conducted in a sample of 1,000 patients admitted in general medicine wards, intravenous cannulas were absolutely idle in around 33% of the patients. An idle cannula is a cannula that is not used for 48 hours or more or without any prophylactic indication (when a cannula is inserted in anticipation of any requirement).
99% Savings - Buy Just @1 Rs
X

- हिं - हिंदी
- En - English
- Treatment
-
- Skin Issues
- Acne
- Fungal Infection
-
- Hair Problems
- Hair Growth
- Hair Dandruff
- Self-Analysis
-
- Chronic Diseases
- Diabetes
- Heart Care
- Weight Loss
- Sleep Support
- Liver Care
- Stress & Anxiety
- Our Brands
- Doctor Consultation
- Medicine A-Z
-
Health A-Z
-
- Treatments
- Home Remedies
- Herbs
- Surgery
- Lab Test
- Therapy
- First Aid
- Ayurveda
- Homeopathy
-
- Yoga And Fitness
- Fitness
- Yoga
- Weight Loss
- Weight Gain
-
- Other Topics
- Baby Names
- Beauty
- Healthy Foods
- Tips
- Health News
- Pet Health
- Men Health
- Medical Cannabis
- Login / Sign Up