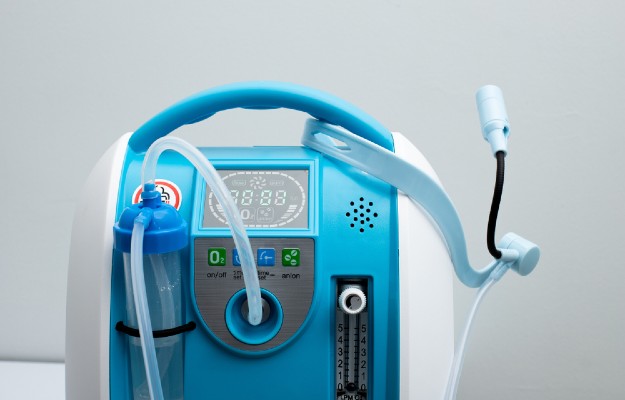
Oxygen therapy refers to a treatment in which a patient is provided supplemental oxygen.
This therapy is given to those who are not able to get enough oxygen on their own. This can happen to those with lung diseases like asthma, chronic obstructive pulmonary disease (COPD) and pneumonia or other health conditions like heart failure and sleep apnea.
Oxygen therapy is also given to COVID-19 patients who experience respiratory distress and hypoxia (lack of oxygen in the body).
This therapy improves the blood oxygen levels of the patient and helps them feel better.
Read on to know more.
Read more: Ventilators for COVID-19 patients to have these special features