Summary
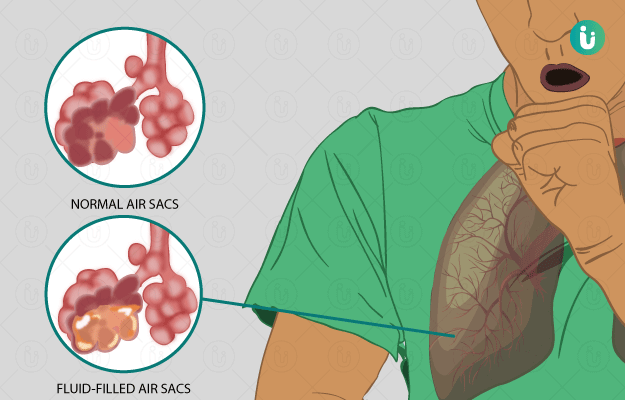
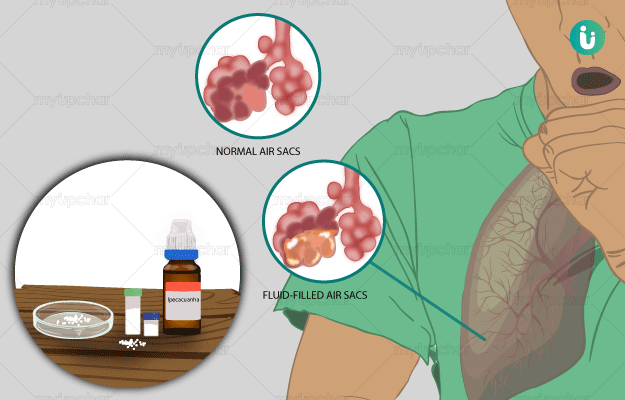
Pneumonia is an infection of the lungs in which there is fluid or pus accumulation in the small air sacs called alveoli of the lungs. It can affect one or both the lungs. Pneumonia is associated with many underlying causes including bacterial, fungal, viral and other less common types of infection. Symptoms include a cough, fever with chills, and difficulty in breathing. These symptoms can be mild, moderate, or severe. The intensity of the infection is determined by many factors such as the microorganism causing the infection, the overall health as well as the age of the affected person. Diagnosis is established based on the medical history of the affected person, laboratory tests and other diagnostic and imaging tests.
Treatment depends on the type of infection that causes pneumonia. If pneumonia occurs due to a viral infection, no specific treatment is employed and the individual’s health usually improves on its own. In the case of bacterial pneumonia, antibiotics are used. While pneumonia is mostly treated at home or out of a doctor’s clinic, a severe infection may require hospitalization. Complications of the disease may include lung abscess (pus formation), respiratory failure, or sepsis (blood infection), which may also lead to multiple organ failure. People who are otherwise healthy usually show a quick recovery if prompt treatment and care is initiated. However, for children under five years of age and adults above the age of 65 years, pneumonia tends to be more serious. People suffering from long-term diseases, especially those of the kidneys, lungs or the heart, and have a weak immune system, pneumonia tends to be severe.

 Doctors for Pneumonia
Doctors for Pneumonia  OTC Medicines for Pneumonia
OTC Medicines for Pneumonia
 Lab tests for Pneumonia
Lab tests for Pneumonia Pneumonia articles
Pneumonia articles News for Pneumonia
News for Pneumonia
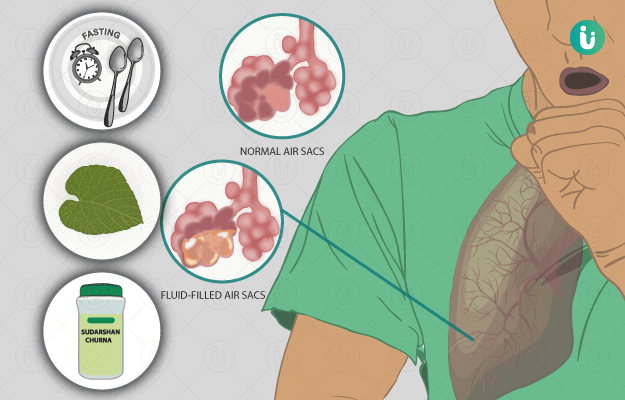
 Ayurvedic Treatment of Pneumonia
Ayurvedic Treatment of Pneumonia
 Homeopathic Treatment of Pneumonia
Homeopathic Treatment of Pneumonia



































 Dr. Ayush Pandey
Dr. Ayush Pandey
 Dr. Rachita Narsaria
Dr. Rachita Narsaria
 Dr. Laxmidutta Shukla
Dr. Laxmidutta Shukla