What is a hip MRI?
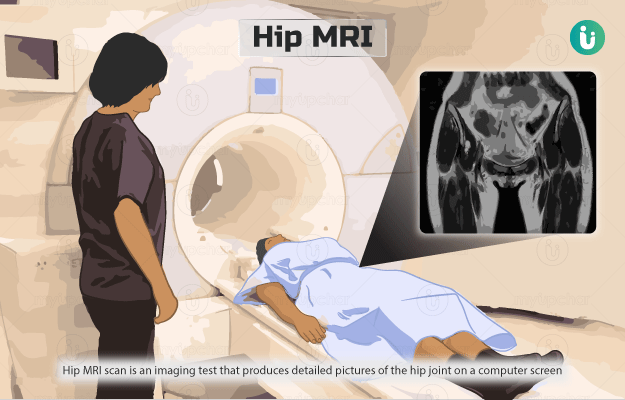
Hip MRI (magnetic resonance imaging) scan is an imaging test that produces detailed pictures of the hip joint on a computer screen using a strong magnetic field and radio waves.
The hip joint, one of the largest weight-bearing joints in our body, consists of the ball or rounded head of the thigh bone (femur) cupped into the socket (acetabulum) of the hip bone. The joint is reinforced by tissues such as:
- Cartilage: The tissue that lines the joint and provides cushioning.
- Ligaments: Tough bands of tissue that anchor the ball to the socket.
- Labrum: A circular band of cartilage that surrounds the socket to provide more stability to the joint.
For an MRI procedure, the person is asked to lie under the strong magnets of the MRI machine. The transmitter of the machine sends short bursts of radio waves, which alter the atoms in the part of the body being scanned. Once the transmitter is shut off, the altered atoms send out radio signals, which are picked up by the receiver of the machine. A computer then uses the data received to create images of the scanned body part.
In some cases, contrast materials are administered to the patient to improve the clarity of pictures. These materials are special dyes that outline the structures within the hip joint and help distinguish normal from abnormal conditions. An MRI of joints with contrast, otherwise called MR arthrography, is the preferred technique for the evaluation of joint conditions and unexplained pain.
There are two types of MR arthrography: direct MR arthrography and indirect MR arthrography. In direct MR arthrography, the doctor injects the contrast material directly into the joint, whereas in the indirect method, the contrast material is administered into the bloodstream and gets absorbed into the joint. Direct MR arthrography is the preferred method because it enlarges the joint, thereby allowing better visualisation of the internal structures.