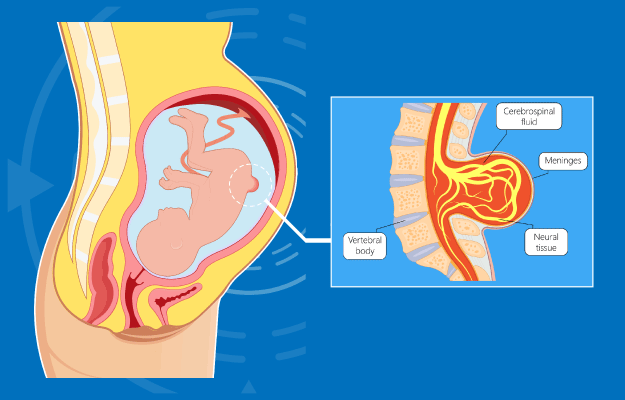
Spina bifida is a type of birth defect or congenital anomaly that occurs when the spine and spinal cord of the foetus do not develop properly. It is a type of neural tube defect (NTD) in which a part of the spine and associated areas form outside the body - this can occur anywhere along the length of the spine. Spina bifida results in damage to the spinal cord and nerves, and it is, therefore, a permanently disabling birth defect.
There are three different types of spina bifida, depending on how the defect takes form: spina bifida occulta, meningocele and myelomeningocele. While the exact cause of spina bifida is not known, doctors have identified a few risk factors that can combine to increase the chances of a baby being born with this congenital defect.
Spina bifida can be diagnosed during prenatal checkups, especially if the mother has a folate deficiency, diabetes, seizure disorders or obesity. An ultrasound during pregnancy, blood test and a test called amniocentesis can usually reveal if your baby is at risk of or has already developed spina bifida.
This birth defect can impair the quality of your child’s life immensely as it is associated with a number of complications like bowel incontinence, urinary incontinence, hydrocephalus (fluid build-up in the brain), mental retardation and paralysis.
Although spina bifida can be treated through surgery, this treatment doesn’t resolve the condition completely. This is the reason why taking preventive measures before and during pregnancy is the best way to reduce the risk of spina bifida.

 OTC Medicines for Spina Bifida
OTC Medicines for Spina Bifida