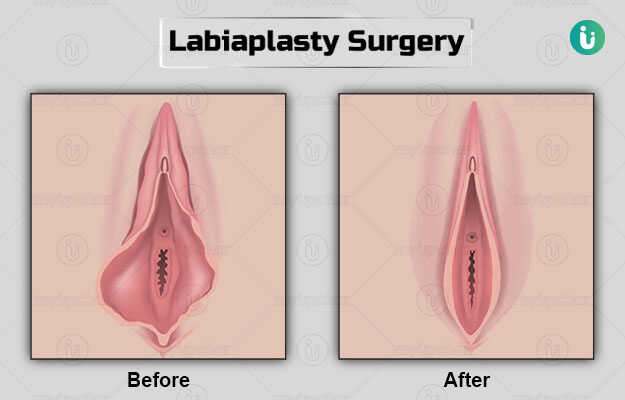
Labiaplasty is a surgical procedure done to alter the size of the labia minora or/and labia majora (the skin folds that surround the urethra and vagina).
The reason for surgery is either cosmetic or medical-related.
Preoperative counselling regarding the reason for surgery is important. Prior to surgery routine blood tests are required.
The procedure is mostly a daycare admission but may require further hospital stay depending on the complexity of the surgery.
Aftercare involves taking care of the wound to prevent further bleeding or injury to the wound. Complete healing takes about 4 to 6 months.
- What is labiaplasty
- Indications for surgery
- Contraindications for surgery
- Preparations before the surgery
- What happens during surgery
- Risks and outcomes of the surgery
- Aftercare, discharge and follow up
- Takeaway
What is labiaplasty
The vaginal and urethral opening is surrounded by folds of skin (shaped liked vertical lips) known as labia. These are two in pair i.e., the outer lips known as the labia majora and the inner lips known as labia minora. The labia majora is covered with hair. The labia minora is smaller and is not covered by hair. The function of the labia is to cover and protect the urethral and vaginal opening.
Labiaplasty is a surgical procedure that is primarily used to alter the size (mainly size reduction) of the labia minora. Sometimes the labia majora may be involved in the surgery.
Indications for surgery
The following are the indications for surgery
- Medical reasons: these include
- In patients where the edges of labia minora are large and hence protrude beyond the boundaries of the labia majora. The excess tissue may get tugged, twisted or pinched causing discomfort during physical activities such as exercise, cycling, intercourse
- The large edges can hinder hygiene and hence can are areas of bacterial growth which can cause infections particularly urinary tract infection
- Cosmetic reasons: these include
- Postmenopause: hormonal changes cause the outer lips to thin thereby causing the inner lips to relatively enlarge
- Childbirth and weight gain are factors to cause the enlargement of the labia minora
- To eliminate the visual lines which are more prominent while wearing tight-fitting lowers
- To improve comfort, self-confidence and by extension sexual well-being during intimacy
- In gender-affirming surgeries: in transgender women to create the external genitalia labiaplasty is one of the procedures performed.
Contraindications for surgery
There are no relative contraindications for the surgery. However, the risk of complications increases in
- Pre-existing conditions such as diabetes, heart disease or hormonal conditions
- Any active infection or malignancy in the area that greatly reduces the success rate of the surgery
Preparations before the surgery
Labiaplasty may be done either by an OBG surgeon or a plastic surgeon. The surgeon discusses in detail the expectations of the patient along with the technique and risks involved in the procedure with the patient.
A complete medical history of the patient is taken involving the symptoms of the patient, the menstrual history, medication history (if any).
Counselling is of importance especially if the surgery is done in patients who seek cosmetic benefit or gender affirmation and will be continued post-surgery as well
Medications, if any, for any pre-existing conditions may be altered/stopped prior to the surgery as per the surgeon’s orders. Investigations include
- Routine blood investigations
- Routine urine tests
- Chest X-ray
The patient will be sore post-surgery and is advised to arrange for a ride back home beforehand. The surgery is usually a daycare admission (admitted in the morning and the patient is discharged by the evening). However, in gender-affirming surgeries, the duration of hospital stay is a few days
The patient is asked to fast overnight before the surgery. On the day of the surgery, the patient arrives at the hospital with all the relevant documents and investigations. She is asked to change into hospital clothes. A final review of the patient by the surgeon and nurse clearing the patient for surgery. The area of surgery is prepared by shaving the hair around the pelvis and legs. The surgeon takes written consent from the patient after explaining the procedure and the risks associated with it. The patient is then shifted into the operation theatre (OT).
What happens during surgery
The patient is made to lie down in the lithotomy position (position where the patient is lying on their back and the legs of the patient are spread wide when giving birth). A monitor is attached to keep track of the vitals (heart rate, blood pressure and oxygen saturation) of the patient. An IV cannula is inserted to administer medications during the surgery (antibiotics/anaesthesia). A urinary catheter is inserted to prevent urine from contaminating the surgical area. The area of surgery is cleaned and the surrounding area is covered with surgical drapes. depending on the complexity and duration of the procedure either general or local anaesthesia can be administered.
The two main approaches of labiaplasty are:
- Reduction of the labia minora: the surgeon can achieve this by:
- Trim procedure: in this approach, the surgeon removes (trims) the outer edges of the labia minora thereby making it even/smaller than the labia majora
- Wedge resection: in this approach a wedge-shaped piece is resected from the inner aspect of the labia minora and the area is approximated through sutures resulting in reducing the size of the labia majora
- Enlargement of the labia major: This is achieved by injecting the labia majora with fat (harvested from the patient’s thighs), thereby enlarging the labia majora as compared to the labia minora. This is a lesser followed approach.
The incisions made during surgery are closed using absorbable sutures (stitches that dissolve by themselves over a period of time). The entire surgery normally does not exceed more than 2 hours.
In gender-affirming surgeries, the labia are constructed using the penile tissue of the patient. This is one of the steps in the entire gender-affirming surgery. The duration of surgery is also much longer in these patients.
Risks and outcomes of the surgery
Complications associated with the surgery are uncommon. However, they can include
- Excessive bleeding from the site
- Infection at the site
- Excessive pain and swelling at the site
- Scarring of the tissue leading to issues in cosmetic appearance
- Damage to the nearby nerves that could lead to decreased sensation
- Complications due to anaesthesia
Aftercare, discharge and follow up
After the surgery, the patient will be shifted from the OT and is kept in an observation room for a few hours. The pain and swelling are controlled via analgesics. The urinary catheter is removed. Normal passage of urine indicates the wearing off of anaesthesia.
A discharge summary is prepared by the doctor that contains relevant medications and advice on wound care. These typically include
- Continue medication for pre-existing conditions, if any
- Antibiotics and analgesics to prevent pain and infection, respectively. Topical preparations may be prescribed.
- Apply ice packs for 20 minutes once or twice a day on the first day to reduce the swelling and stop bleeding
- Sanitary pads can be used to absorb the bleeding that may occur in the first couple of days but subsides later on
- Sitz bath once or twice a day: a sitz bath is a special bath that involves soaking the perineum (area between the urinary and anus) in warm water for 15-20 minutes. The bath relieves pain and swelling and promotes wound healing.
- Pat dry the area after bathing
- Maintain proper hygiene especially after using the toilet. Wash the area with warm water and pat dry
- Wear loose thin undergarments to prevent irritability and friction around the wound
- Abstain from strenuous physical exercises and sexual activities for 4 to 6 weeks
The sutures dissolve after 4 to 6 weeks after surgery. However, notify the doctor if you experience any of the following:
- Excessive bleeding
- Swelling and pain
- Pus discharge from the wound
- Burning sensation in urine
- Fever
The hospital stay and total recovery time are significantly more prolonged in the case of gender-affirming surgeries.
Serial follow-ups with the surgeon and counsellor are done so that the patient finds it easier to adjust to the results of the surgery. It takes about 4 to 6 months for the wound to heal completely.
Takeaway
Labiaplasty is recommended in women when the enlarged labia minora causes painful and irritable symptoms that interfere with daily activities. Some patients opt for it to enhance its appearance, especially post-childbirth or menopause. It is also one of the surgeries performed in gender-affirming surgery.
Hence, patients undergoing labiaplasty should discuss the expectations and outcome in detail with their surgeon before opting to go through with the procedure. Counselling is an important aspect and is advised pre and postoperatively. Complete recovery takes 4 to 6 months.
Find Obstetrician and Gynaecologist in cities
- Obstetrician and Gynaecologist in Bangalore
- Obstetrician and Gynaecologist in Mumbai
- Obstetrician and Gynaecologist in Ghaziabad
- Obstetrician and Gynaecologist in Chennai
- Obstetrician and Gynaecologist in Pune
- Obstetrician and Gynaecologist in Delhi
- Obstetrician and Gynaecologist in Hyderabad
- Obstetrician and Gynaecologist in New Delhi
- Obstetrician and Gynaecologist in Gwalior
- Obstetrician and Gynaecologist in Gurgaon
Surgery Cost In Your City
Doctors for Labiaplasty

Dr. Shravani A
Obstetrics & Gynaecology
3 Years of Experience

Dr Minoo Singh
Obstetrics & Gynaecology
44 Years of Experience

Dr. Godi Anuradha
Obstetrics & Gynaecology
31 Years of Experience