Summary
Vertebrectomy involves the removal of some elements of the spine along with the vertebral bodies. This surgery is performed when individuals complain of neurologic deficits, pain, and reduced coordinated movements. These symptoms can be caused by spinal compression leading to nerve pinching, tumours that press against the spinal canal, or any other mechanical trauma. You will need to fast from midnight, the night before the surgery. The procedure will be done under general anaesthesia. You will have to visit the doctor four to six weeks after the procedure for a follow-up visit.
- What is vertebrectomy?
- Why is vertebrectomy recommended?
- Who can and cannot get vertebrectomy?
- What preparations are needed before vertebrectomy?
- How is vertebrectomy done?
- How to care for yourself after vertebrectomy?
- What are the possible complications/risks of vertebrectomy?
- When to follow up with your doctor after a vertebrectomy?
What is vertebrectomy?
The human spine (or vertebral column) is a structural and central support system of the body that keeps the body erect and upright. It is divided into four regions – neck region (cervical spine), upper and mid-back region (thoracic spine), lower back region (lumbar spine), and base of the spine (sacral spine) - and has 26 vertebrae (sequentially arranged small bones) that extend from the base of the skull to the base of the spine called the coccyx. The vertebrae are separated by intervertebral discs.
Each vertebra has a vertebral body on the anterior side and the vertebral arch on the posterior side. The spinal cord passes through a hollow centre between the vertebral arch and body. Now, the vertebral arch is made of various parts including a pair of transverse processes on either side and a single spinous process, which is a projection on the posterior end of the vertebral arch. The transverse process is connected to the vertebral body through two pedicles and to the spinous process through two laminae. Right between the lamina and the pedicles on each side of the vertebral arch are articular processes. There are about four articular processes in each vertebra. It helps connect two vertebrae togather.
some posterior projections and a body that has a hollow centre for the spinal cord to pass through it.
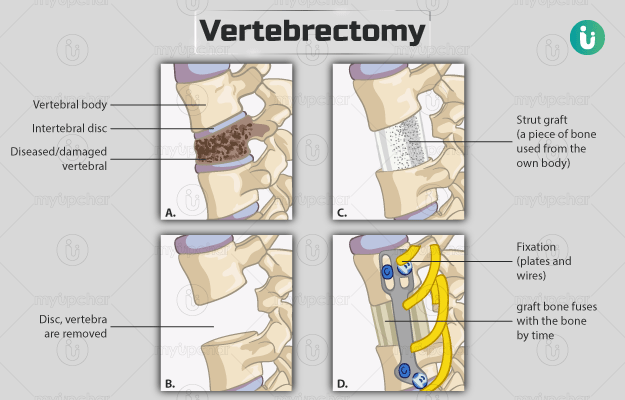
A vertebrectomy refers to the removal of all the posterior (backside) spinal components (the spinous process, lamina, and pedicles) and the vertebral body.
This procedure may be performed in the cervical, thoracic, or lumbar regions of the spine. The space that is created after this surgery is filled with an implant (synthetic cage or bone graft), and the spinal column is reconstructed. Additionally, spine-stabilising materials are inserted above and below the vertebra for stability and support.
Why is vertebrectomy recommended?
The doctor may recommend this surgery under the following conditions:
- Fractured vertebral body causing the bony fragments to displace into the spinal canal and compress the spinal cord
- A tumour of the vertebral body spreading to the spinal canal.
- A cervical vertebrectomy is indicated for ossification of the posterior longitudinal ligament (a condition where a flexible structure called posterior longitudinal ligament, located posterior to the vertebral bodies, reduces in flexibility and becomes bone-like) in people with kyphosis (an abnormally curved spine)
- Nerve root or spinal cord compression
- Pseudoarthrosis
- Degenerated or herniated disc
- Chronic instability of the vertebrae
- Spinal deformity due to scoliosis (sideways curvature of the spine)
- Vertebral osteomyelitis (a bone infection) that causes the vertebral body to collapse.
Common symptoms of spinal problems include:
- Stiffness in the lower back
- Pain for more than 10 days
- Muscle spasm
- Pain radiating from the spine to the chest wall
- Loss of movement
Who can and cannot get vertebrectomy?
Vertebrectomy is contraindicated in people with:
- Trauma to the trachea and oesophagus
- Severe osteoporosis
What preparations are needed before vertebrectomy?
Some of the preparations needed before this surgery include:
- Your doctor will perform a physical examination and order the following tests:
- Complete blood count
- Electrocardiogram
- Chest X-ray
- Stress test (in case of cardiac history)
- Inform your doctor about all your ongoing medications, especially blood thinners (like aspirin), over-the-counter medicines, and supplements. You may be asked to reduce or discontinue the medicines during the surgery temporarily.
- Inform your doctor if you are allergic to any medicines, latex, or food.
- Your doctor should know if you have any medical conditions such as bleeding problems or diabetes.
- You will be asked not to drink or eat anything after midnight, the night before the surgery.
- Avoid smoking a month before the procedure, as nicotine may cause a problem in recovery and bone fusion.
- Tell your doctor if you are or may be pregnant as X-rays taken during the surgery can affect the growing baby. Also, you will be asked to sign a consent form before the procedure.
On the day of the surgery:
- Avoid wearing any makeup, nail paint, contact lenses, dentures, or jewellery.
- Your doctor may advise you to avoid taking any antidiabetic medications, antidiuretics, antihypertensive medications on the morning of your operation.
How is vertebrectomy done?
Once you are in the hospital:
- Your doctor will ask you to wear special socks to improve circulation during and after the surgery.
- The operation will be performed under general anaesthesia (a sleep-inducing medicine).
- A Foley catheter will be placed in your bladder to drain urine.
The surgery may be performed by an anterior or a posterior approach. The posterior access involves the following steps:
- The surgeon will monitor the functioning of your spinal cord using a test called evoked potentials. The test measures the time required by the brain to respond to stimuli. It helps ensure the safety of your spinal cord during the surgery.
- You will be made to lie face-down on the medical table.
- After the anaesthesia takes effect, the surgeon will make an incision on the affected area, and expose the bones in your vertebral column.
- He/she will insert special screws called pedicle screws above and below the vertebra to be operated.
- Thereafter, the surgeon will slowly work on the affected vertebra from back to front.
- He/she will first remove the bony projections or processes from the back of the vertebra. Then gradually remove the laminae and facet joints, which are joints that connect with the backs of other vertebrae.
- The pedicles will be removed next.
- After this, the surgeon will remove a side of the vertebral body (from the affected area) on one side of your spinal cord.
- He/she will temporarily insert rods into the pedicle screws. These rods will stabilise your spine as the surgeon removes the other half of your vertebral body. With this, one vertebra is removed. If other vertebrae are to be removed, it will be done similarly.
- After the procedure, the surgeon will realign your spine, ensuring that your spinal cord is not compressed or stretched. He/she will make sure that your spine is manoeuvred into optimal alignment.
- Once your spine is aligned, the surgeon will fill the vacant spots with implants. These implants can be artificially synthesised using man-made bones, titanium, or ceramic (cage) or a piece of bone used from your own body (a strut graft ).
- The surgeon may place in additional bone grafts to fill the gap at the back of your spine.
- Rods and pedicle screws will help stabilise and keep your spine erect until the implant fuses with the other vertebrae.
- Finally, the surgeon will close the incision with stitches, and bandage the wound.
Once the surgery is complete, you will be moved to the recovery room where you can expect the following:
- You will be given pain medications intravenously.
- Your doctor may place a drain at the surgical site (this is to remove any accumulated fluids after the surgery). It will be removed the next day.
- The catheter will be removed soon after the surgery.
- A physiotherapist will teach you exercises to restore your strength and encourage you to walk after the surgery.
- You will be in the hospital for three to five days.
In case of thoracic surgery, your surgeon may suggest wearing a back brace for comfort.
How to care for yourself after vertebrectomy?
You may take the following care at home:
- Your doctor will prescribe pain medications. They tend to cause constipation; therefore, consume adequate amount of water, take a fibre-rich diet, and use stool softeners.
- Physiotherapy may be started in a few weeks after the surgery. It will help strengthen your back and improve your range of motion.
- You will be advised to take a soft diet for the first 14 days after surgery. This includes puddings, fruits, cooked vegetables, protein shakes, among others. Tough meats, nuts, and crunchy food items must be avoided.
- It is preferred to take showers, but do not get the wound wet. Use waterproof dressings for this purpose.
- You may be able to resume work eight to 12 weeks after the surgery.
- Walking is the best form of exercise in the first six weeks after the procedure. Start slowly and build up to 30-minutes of walking.
- Remember all postural and positional restrictions explained to you for the first six weeks after surgery. Do not bend or twist. Also, avoid pushing, lifting, or pulling items that weigh more than 5 kilograms. Make sure to keep your spine straight, maintaining the natural curve of the back.
When to see the doctor?
Call a doctor immediately if you experience the following symptoms:
- Sudden numbness or weakness that does not go away
- Sudden loss of control of the bladder and bowels
- A fever of 101.3°F (38.5°C) or more
- Swelling, redness, and oozing of liquid from the surgery site
- Extreme pain that is different from the usual pain
- Headaches that last for a long time even after taking painkillers
What are the possible complications/risks of vertebrectomy?
Complications associated with this surgery include:
- Nerve root injuries
- Pseudoarthrosis
- Wound infections
- Dural tears (a surgical complication wherein a thin covering called dura mater around the spine gets torn)
- Hemopneumothorax (presence of blood and air in the chest cavity)
- Need for revision surgery
When to follow up with your doctor after a vertebrectomy?
A follow-up visit is planned four to six weeks after the surgery. During this visit, X-rays will be taken to assess bone fusion.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Surgery Cost In Your City
Doctors for Vertebrectomy

Dr. Vatsal Khetan
Orthopedics
9 Years of Experience

Dr. Prince Uchadiya
Orthopedics
7 Years of Experience

Dr. Manoj Kumar S
Orthopedics
8 Years of Experience
Dr. Ankur Saurav
Orthopedics
20 Years of Experience
References
- Gupta MC, Devlin VJ, GogiaJS. Procedures for decompression of spinal cord and nerve roots. In: Devlin VJ. Spine Secrets Plus, 2nd ed. Elsevier Mosby; 2012. p. 165
- Waxenbaum JA, Reddy V, Williams C, et al. Anatomy, Back, Lumbar Vertebrae. [Updated 2020 Aug 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan
- The Spine Hospital: The Neurological Institute of New York [Internet]. Department of Neurological Surgery. Columbia University. US; Vertebral Column Resection
- American Association of Neurological Surgeons [Internet]. Illinois. US; Spinal Pain
- Guy's and St. Thomas' Hospital: NHS Foundation Trust [Internet]. National Health Service. UK; Anterior Cervical Surgery
- Johns Hopkins Medicine [Internet]. The Johns Hopkins University, The Johns Hopkins Hospital, and Johns Hopkins Health System; The Road to Recovery After Cervical Spine Surgery
- Brighton and Sussex University Hospitals [Internet]. NHS Foundation Trust. National Health Service. US; Information and Guidance for Patients following Lumbar spinal surgery
- Saifi C, Laratta JL, Petridis P, Shillingford JN, Lehman RA, Lenke LG. Vertebral column resection for rigid spinal deformity. Global Spine J. 2017;7(3):280–290. PMID: 28660112.
- Gokaslan ZL, York JE, Walsh GL, McCutcheon IE, Lang FF, Putnam JB Jr, Wildrick DM, Swisher SG, Abi-Said D, Sawaya R. Transthoracic vertebrectomy for metastatic spinal tumors. J Neurosurg. 1998 Oct;89(4):599-609. PMID: 9761054.