Summary
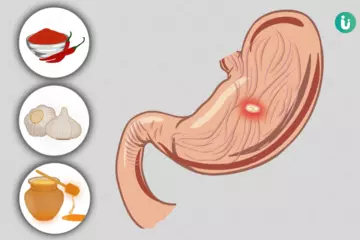
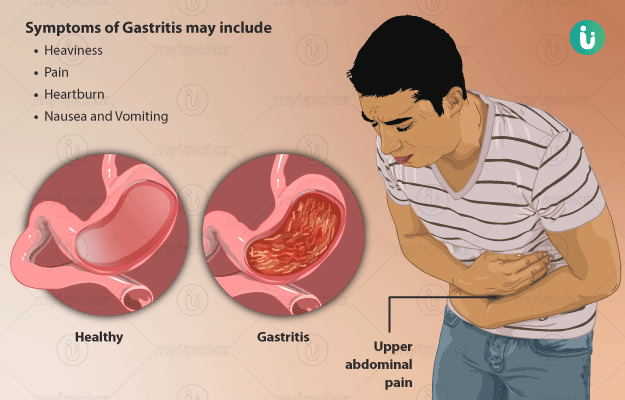
Gastritis is one of the most common digestive tract disorders. It occurs due to the inflammation and irritation of the inner lining of the stomach. This stomach inflammation can cause pain, burning sensation in the upper abdomen, heartburn, burping, regurgitation of food, nausea, and occasional vomiting. Gastritis could be a result of prolonged use of painkillers (NSAIDs), bacterial infection, smoking, alcohol, and some autoimmune conditions. It may sometimes linger for several years. Diagnosis is established by endoscopy. Treatment options include the use of antacids, antibacterial therapy, and dietary alterations.

 Doctors for Gastritis
Doctors for Gastritis  OTC Medicines for Gastritis
OTC Medicines for Gastritis
 Gastritis articles
Gastritis articles
 Ayurvedic Treatment of Gastritis
Ayurvedic Treatment of Gastritis
 First Aid for Gastritis
First Aid for Gastritis
 Homeopathic Treatment of Gastritis
Homeopathic Treatment of Gastritis




































 Editorial Team
Editorial Team

 Dr. Rachita Narsaria
Dr. Rachita Narsaria

 Dr. Laxmidutta Shukla
Dr. Laxmidutta Shukla