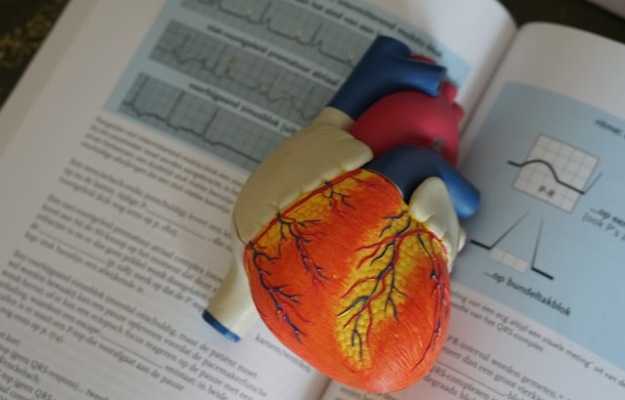
The heart is a muscular organ that pumps blood to all parts of the body. Our blood transports oxygen, nutrients, immune cells, and a number of hormones, enzymes and other proteins throughout the body. But what happens when the heart is unable to pump well?
We are all aware of heart diseases like heart failure—which happens when the muscles of the heart are unable to pump blood properly, usually because they have become weak.
Please check this page for complete treatment of coronary heart disease.
Hypertrophic cardiomyopathy is another condition in which the heart may not be able to pump blood properly—this happens when the wall (septum) that separates the lower right and left chambers (ventricles) of the heart becomes too thick (hypertrophied) or stiff.
People with this condition may also have an abnormal arrangement of heart muscle cells, which is called myofiber disarray. This abnormal arrangement is responsible for triggering arrhythmias (irregular heartbeat) in some people.
Hypertrophic cardiomyopathy is “the most frequent cause of death in young people (including trained athletes)”, according to a 2013 seminar lecture published in The Lancet. The seminar also pointed out that some 1,400 mutations have been observed in 11 genes in many people with this condition.
In addition to managing symptoms like chest pain and shortness of breath, treatment may involve medicines (pharmacological intervention), electrical interventions like placing an implantable cardioverter-defibrillator (ICD) or surgical intervention like septal myectomy in which a portion of the thickened wall is removed in open-heart surgery.
In people who experience syncope (fainting without an obvious reason), irregular heartbeat (arrhythmias) especially during exercise, it is recommended that they see a doctor who can diagnose or rule out hypertrophic cardiomyopathy.
(Read More - Heart Bypass Surgery)

 Doctors for Hypertrophic cardiomyopathy
Doctors for Hypertrophic cardiomyopathy  OTC Medicines for Hypertrophic cardiomyopathy
OTC Medicines for Hypertrophic cardiomyopathy