Coronary angiography is a minimally-invasive, special-imaging procedure that helps visualise and assess the heart and its blood vessels. It is an important procedure and is commonly advised in heart conditions such as heart attack, abnormal chest pain, and structural abnormalities of the heart, to name a few.
Click on the link to know in detail about heart disease treatment.
The procedure is a small one and the patient is usually admitted in the morning and discharged by the evening. After discharge, the patient is advised to not drive while going home from the hospital.
Before the procedure, investigations such as blood tests, chest x-ray, and ECG are carried out.
Post-procedure care and recovery are usually simple and uncomplicated, e.g. the patient is instructed to avoid lifting heavy weights or do strenuous exercise. Follow up with the doctor is usually within 1 week.
(Read More - Ventricular Tachycardia treatment)
- What is Coronary Angiography?
- Indications for Coronary Angiography
- Contraindications for Coronary Angiography
- What preparations are done before Coronary Angiography
- What happens during Coronary Angiography
- Care after Coronary Angiography
- Discharge advice and follow up
- Takeaway
What is Coronary Angiography?
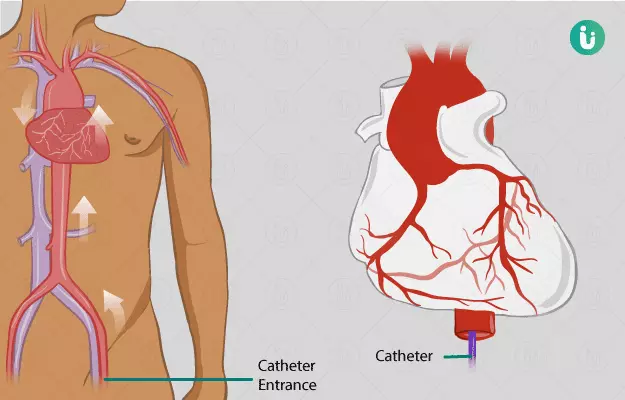
Angiography is a minimally-invasive medical-imaging procedure used to visualise and assess blood vessels using a special dye (radiopaque contrast agent, a substance that is visible on x-ray) that is typically injected using a catheter (very small, hollow flexible tube). Coronary angiography, by extension, is a procedure used to visualise and assess the heart and its blood supply and hence can identify any structural or functional abnormalities of the heart and its vessels.
The heart is the main organ that transports blood throughout the body. It is made of four chambers. The heart itself gets blood supply from two vessels called coronary arteries (left and right). They are named so because they form a crown (corona) around the heart.
Coronary angiography can identify occlusions/blockages, narrowing or abnormal dilation of the coronary vessels along with heart chamber size and the heart’s pumping performance and is hence a diagnostic procedure. It can also be combined with interventional procedures most commonly being coronary angioplasty.
(Read More - Bradycardia treatment)
Indications for Coronary Angiography
The following are some of the reasons for doing coronary angiography:
- Heart attack: symptoms may include chest pain (not relieved by medications), sweating, abnormal pain in the jaw, pain in the left arm, or pain in the back, shortness of breath, blackout (syncope).
- Diseases of the heart present from birth, such as structural abnormalities in the walls of the heart or its valves.
- Abnormal results of non-invasive investigations such as ECG, 2D echo of heart, CT of heart, cardiac stress exercise tests.
- To monitor the acceptability/rejection status in heart transplant patients.
- To assist interventional procedures such as angioplasty (placement of a stent in the vessels), a biopsy of a part of the heart, bypass procedures of the heart.
(Read More - CT Coronary Angiography)
Contraindications for Coronary Angiography
The procedure is relatively contraindicated (i.e. the procedure is riskier) in patients with:
- Uncontrolled blood pressure
- Coagulopathy (excessive bleeding or clotting)
- Pregnancy
- Kidney dysfunction
- Severe anaemia (low haemoglobin (Hb))
- Pre-existing heart conditions such as irregular heartbeat, weak heart
- Active systemic infection
- History of allergies to food or allergy to medicines (which may cause a severe allergic reaction with dye)
(Read More - Tachycardia treatment)
What preparations are done before Coronary Angiography
The procedure can be done in an elective (planned) or emergency scenario depending on the severity of the indication. The procedure along with the risks are explained to the patient.
A detailed medical history of the patient is taken which includes the patient's symptoms, any other diseases the patient might have (comorbidities), medication history, menstrual history, history of allergy to any medications/food, and family history.
Investigations primarily include
- Blood tests which include
- Complete blood count: to check haemoglobin levels and infection
- Coagulation profile
- Kidney function test
- X-ray of the chest (after ruling out pregnancy)
- ECG (electrocardiography)
- Other tests may include CT of the heart and cardiac stress tests.
Before the procedure, medications such as anticoagulants and cardiac medications may be altered/stopped as per the doctor’s assessment.
(Read More - Aortic Stenosis treatment)
What happens during Coronary Angiography
The procedure is usually a short one and people are admitted in the morning and can be discharged by the evening. The patient is asked to fast overnight before the day of the procedure.
On the day of the procedure, the patient arrives with all the relevant reports of the investigations and changes into hospital clothes. Some investigations may be repeated as advised by the doctor after admission.
Pre-procedure instructions
Pre-procedure instructions involve:
- Continuing the medications as prescribed by the doctor if any pre-existing illness is present.
- Taking consent for the procedure from the patient and the relatives after explaining the risks.
- The site for the catheter insertion (i.e., arm/groin area) is shaved and cleaned.
- The vital signs of the patient (viz. heart rate, blood pressure, and oxygen saturation) are checked to ensure that they are within normal limits.
During the procedure
The patient is then shifted into a procedure room called the Cath Lab. The patient is made to lie flat on their back on an X-ray table. A monitor is attached to observe the vitals continuously. An IV cannula is inserted through which a mild sedative is given. The patient will remain awake throughout the procedure.
Sterile (clean) drapes are placed on either the arm or groin depending on where the incision will be placed and the catheter is then inserted. A local anaesthetic may be given before the incision to minimise the pain.
Once the catheter is placed, it is slowly passed along the lumen of the blood vessel towards the heart. This process is known as threading. The patient does not feel the catheter moving through the blood vessel since it has fewer nerve fibres. The progression of the catheter is monitored through serial dynamic X-rays.
Once the catheter is at the desired position, the dye is then injected. The patient may feel a slight flushing/burning at the time of injection. Serial dynamic X-rays are again taken.
Interventional procedures
Post this, interventional procedures, if required, are performed, followed by additional serial dynamic x-rays. Thereafter, the catheter is slowly pulled out from the incision site completely. A pressure bandage is then applied to the incision area to stop the bleeding.
The entire procedure typically takes about 1 hour but can increase in duration depending on other interventional procedures performed.
Some types of interventions performed are:
- Angioplasty: a procedure in which a stent is placed in clogged up arteries by ballooning them first, to keep them open.
- Atherectomy: a procedure used to improve the blood supply in blocked coronary arteries.
- Ventriculogram: a dye is passed into a ventricle of the heart(one of the heart chambers) to assess its function.
- Valvuloplasty: a procedure used to reopen narrowed valves in the heart
- Heart biopsy: a small portion of heart tissue is removed and sent for pathological studies.
(Read More - Homeopathic treatment for heart attack)
Care after Coronary Angiography
After the procedure is complete, the patient is shifted into the observation room. To prevent bleeding, the patient is made to lie down and instructed not to sit up suddenly, stand or raise their head. The vitals are again monitored since some people can feel dizziness after the procedure. IV fluids may be administered. However, the patient is advised to start oral fluids as soon as they are able to.
Symptoms that need to be notified to the doctor immediately are:
- Extreme pain at the incision site
- Bleeding at the incision site
- Tingling or numbness in the fingers if the procedure is done in the arm
- Chest pain, difficulty in breathing, dizziness, vomiting
Redness (rash) or mild swelling is common at the incision site and subsides over a few days. In case the swelling increases, the doctor should be notified.
The patient is told to drink plenty of fluids to flush out the dye from the body through urine. The patient is typically kept under observation for four to six hours. During this time, the doctor discusses the reports and the outcome of the procedure as well as gives instructions on aftercare.
(Read More - Heart valve replacement)
Discharge advice and follow up
If the procedure is uneventful and without complications, the patient is discharged in the evening. The patient is given a discharge summary with a set of medications and instructions that should be followed. These include:
- Pre-existing medications for comorbid conditions should be continued.
- New medications that the doctor prescribes as per the results of the procedure.
- Analgesics and antibiotics to prevent pain and infection respectively.
- Relatives of the patient are advised to not allow the patient to drive while going home.
- To leave the bandage in place until told to remove it (usually 24-48 hours).
- To avoid strenuous exercises or lift heavy weights for a few days.
- Warning signs such as excessive pain, excessive bleeding, discharge of pus from the incision site, fever are to be looked out for and to be reported to the doctor immediately.
- Healthy diet modifications will be added if needed.
Follow-up depends on the reports of the procedure and as instructed by the doctor, usually from three days to a week later.
(Read More - Mitral valve repair surgery)
Takeaway
In conclusion, coronary angiography is an important, often life-saving procedure with low risks. It is minimally invasive, the duration is shorter as compared to other cardiac procedures, and has hence emerged as a more modern and popular approach to deal with heart conditions.
(Read More - Cardiac Arrest treatment)
Surgery Cost In Your City
Doctors for Coronary Angiography

Dr. Manju
Cardiology
10 Years of Experience

Dr. Farhan Shikoh
Cardiology
11 Years of Experience

Dr. Amit Singh
Cardiology
10 Years of Experience