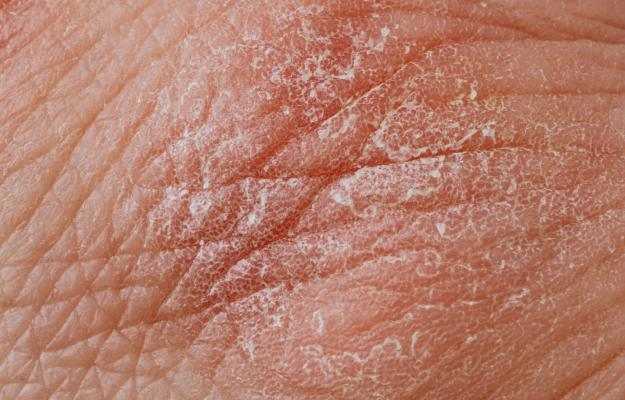
Lichen sclerosus (LS) is a rare skin disorder that causes skin to thin, wrinkle and get patchy, whiten and grow itchy. It affects mostly the genital and anal area. Only in about 15% of cases do lesions develop on the thighs, breasts, shoulders, neck and even inside the mouth.
The disease occurs most commonly in postmenopausal women. The cause is unknown, but hormonal, genetic or underlying diseases are important factors.
LS is not contagious and cannot be transmitted sexually. While there is no cure for it, steroid ointments work well and are able to contain symptoms. There is a chance of the disease recurring, so regular visits to the doctor are recommended to keep it under check.
In men, LS occurs usually on the head of the penis and is more common in uncircumcised men. Circumcision usually takes care of the disease if topical drugs do not.
While LS is not a deadly disease, it does slightly increase the risk of getting squamous cell skin cancer in the genital region.