Summary
Anterior cruciate ligament (ACL) injury is a very commonly occurring sports injury and it affects the function of the knee. In case you get this injury then optimal treatment is very necessary because it can affect your joint function, sports activity, work, and other daily activities. The most common treatment employed for ACL injury is a reconstruction surgery, which is performed by putting small incisions around your knee. The torn ligament is replaced by a tendon from another portion of your knee or from a donor. The procedure is performed by a specialist surgeon after taking necessary pre-surgical steps, such as assessing the status of your health, blood tests, X-rays, anaesthesia (a procedure to numb the surgical area) and so on. After the surgery, a few days of hospitalisation is needed followed by home care which includes exercises, dressing, eating healthy and preventing strain on the operated knee. Read on to know more about the procedure.
- What is an ACL reconstruction surgery
- When is an ACL reconstruction surgery done
- What preparations are done before the ACL reconstruction surgery
- How is an anterior cruciate ligament (ACL) reconstruction surgery done
- Self-care after ACL reconstruction surgery
- What are the risks and complications of an ACL reconstruction surgery
- How does one recover from the ACL reconstruction surgery
- Follow-up after the anterior cruciate ligament (ACL) reconstruction surgery
What is an ACL reconstruction surgery
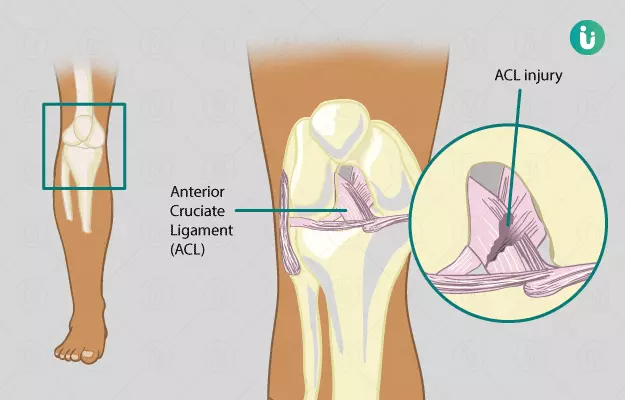
The anterior cruciate ligament (ACL) is located in your knee and it joins the shin bone (tibia) to the thigh bone (femur). Any tear of this ligament can cause your knee to give way during physical activity. ACL reconstruction surgery is done to restore the ligament in the centre. ACL surgery may be required in any age groups that may include but are not limited to young people, active athletes and the elderly population. It is more common in females as compared to males. There might be an audible pop, severe pain and immediate swelling if you get an ACL injury.
When is an ACL reconstruction surgery done
A torn ACL is reconstructed by attaching (grafting) new tissue to it. An ACL reconstruction is done in case you have any of these knee problems:
- A knee that gives way or you feel unstable during daily activities.
- Knee pain.
- If you are unable to continue playing sports or carrying out other activities.
- When other ligaments are also injured.
- When your meniscus is torn. A meniscus is a C-shaped disc of soft tissue made of fibre and cartilage that is interposed between the rounded ends (condyles) of femur and tibia.
- The decision to have the surgery depends upon the extent of damage to the ligament and how much it is affecting your quality of life.
- And very importantly, delaying the surgery will cause further damage to your knee.
What preparations are done before the ACL reconstruction surgery
Before you undergo surgery, the surgeons would want to ensure that you are in good condition to be operated. For this, a few things need to be examined and kept in mind, such as:
- If you have a swelling in your knee then you should wait for the swelling to subside and a full range of movement to return before getting the knee surgery done. Recovery will be more difficult in case you don't have the full range of movement in your knee.
- To help you prepare for the surgery, you might need to go to your Physiotherapist. Your physiotherapist will help you to regain movement in your knee by showing you some low-stress impact exercises like swimming or cycling.
- In case you have an underlying medical condition, such as diabetes or hypertension (high blood pressure) then consult your doctor before the procedure as it is necessary that any such condition is kept under control.
- Tell your doctor about the medicines you are taking. Medicines like aspirin and ibuprofen can make your blood thin which would take it longer to clot after the surgery.
- Ask your doctor about the medicines you can safely take on the day of your surgery.
- If you smoke or drink alcohol frequently then tell your doctor about it and quit it a few days before the surgery. This is very crucial because these products slow down the healing process after the surgery.
- Inform your doctor if you get any illness, such as cold, flu, diarrhoea, herpes and others before surgery.
Preoperative Assessment
It is mostly done one or two days before the operation where you visit the hospital for a few important steps, such as:
- Undergoing a few tests, such as blood test, urine test, X-rays, CT or MRI scan among others.
- To find out any underlying medical condition you might be having that needs to be treated before the operation.
- You will be given clear instructions on when to stop eating before the surgery.
- You will also be informed about the medications, if any, that you should stop taking before going to the hospital for the procedure.
- This is the phase where you should clear all your queries and doubts related to the surgery with your doctor.
How is an anterior cruciate ligament (ACL) reconstruction surgery done
Before you go in for the procedure, a few things that are required to be followed are discussed below:
- Do not to drink or eat anything for 6 to 12 hours before the scheduled time of the procedure.
- The prescribed medicines should be taken with a small sip of water.
- You should take a bath before going for the surgery as it helps in keeping you clean and prevent harmful bacteria from entering your body during the procedure.
- Ask a friend or relative to take you to and from the hospital. You may also need to arrange someone to help you out at home for a week or two after the surgery.
How is the surgery done?
The duration of the procedure is about 1-1.5 hours. For this surgery different types of numbing (anaesthetic) methods may be used so that your procedure is painless:
- General anaesthesia where you will fall asleep and won’t feel the pain during the procedure. After a few hours of surgery, the anaesthesia will fade and your sensations will be back to normal.
- Spinal anaesthesia where the medicine will be injected into a particular space in your spine. You will be awake but the area below your waist will remain numb and pain-free during the procedure.
- Your doctor will recommend which type of anaesthetic agent is to be used. After you’ve been anaesthetised, the surgeon will make 2 to 3 small cuts around your knee. A narrow tube with a tiny camera on the end (arthroscope) will be inserted through one of the cuts. The camera is attached to a video monitor that lets the surgeon see the structures inside the knee clearly.
- The surgeon will check for the torn ACL inside your knee. After the torn ACL is confirmed, the graft tissue will be made ready for relocation.
- The graft is taken either from a donor or from your body itself. It is well trimmed and shaped according to the site it is to be placed at. The ends of the replacement ligament are fixed at appropriate sites with special screws.
- During and at the end of your surgery, sterile (germ-free) salt water or saline will be used to wash the surgical area and simultaneously drain it from your knee. The surgeon will close your cuts with sutures (stitches) and cover them with a dressing.
Self-care after ACL reconstruction surgery
Following is a list of things that you may experience after the surgery:
- Since you would be under the effect of anaesthesia, you may feel a little hazy for a couple of hours. It’s also very common to feel sick or to vomit. However, it subsides within a day or two.
- It is also not unusual to experience some pain after the surgery and for that, painkillers and anti-inflammatory (medicines that reduce the swelling) medicines are given. Taking medication before bedtime will help you in falling asleep more easily.
- Some pain killers can cause constipation. Therefore, it is advised that you consume a fibre-rich diet and also drink plenty of water.
- After surgery, you will be advised to take ample amount of bed rest to help the surgical area heal faster. However, lying down can result in the pooling of blood in your legs, which in turn, can cause swelling and increase the risk of developing blood clots. Try to keep a pillow below your legs so that your feet are at the level of your heart.
- Physiotherapy may also be included, which uses exercise and heat treatments rather than medicines or surgery for healing. It can be started about a week after surgery. Your physiotherapist will guide you with a range of exercises that you can do. Exercises like leg lifts, hip abduction, toe curls, heel slides, prong hangs, and others help in regaining joint strength.
- Do some simple leg exercises, such as straight leg raises, flexing your knees or ankles, and rotating your feet for a week, 10 times a day for at least 10 minutes. These exercises should be done for at least seven days after surgery after taking proper instructions from your surgeon or a physiotherapist. Exercise helps in maintaining blood circulation and prevents blood clots from forming in your legs.
- Bruising, redness and swelling at the surgical site and down your shin and ankle may also occur. This happens because of the synovial fluid (fluid in the joints) leaking down your legs. This is normal and gets resolved within a few days after surgery.
- Getting discharged depends upon the status of your health and its improvement while you’re in the hospital. Before getting discharged, you’ll be advised about how to take care of the wound, correct and proper dressing and bandage application, and so on.
- It is advised that you take bath only after 4 days of surgery. While bathing, water should not come in contact with the incision. A sponge bath is a good alternative. The wound should always be kept clean and dry. The prescribed ointment should be applied and the dressing should be changed twice a day or as per your doctor’s instructions.
- It's important you don’t put too much stress on the joint. Therefore, avoid placing weights on your leg and doing leg lifts on weight machines for the first few months. Also avoid squatting, twisting, jumping, lifting heavy objects, and other movements that could damage your knee.
What are the risks and complications of an ACL reconstruction surgery
Although each and every precaution is taken to ensure minimum discomfort, in some cases, a few complications that may be seen include:
- Infection
Infection can occur during the initial 5-7 days after surgery. Your doctor will prescribe you antibiotics for controlling the problem. In serious cases, surgery may again be required to resolve the infection. - Clot formation in the legs
This can occur after surgery because of the pooling of blood in the legs. It can be treated with medicines that act as clot busters. - Knee stiffness
This can occur because of limited movement of the knee which can further lead to pain. To prevent this, start doing simple exercises as advised by your physiotherapist. - Failure of surgery
The failure rate of the ACL surgery ranges from 2.9% to 13.7%. This can occur due to some sports accident that can cause the graft to rupture or loosen. During the early period of recovery, excessive loads and increased physical activity can also result in the injury to the graft. Therefore, aggressive rehabilitation during the recovery period should be avoided.
How does one recover from the ACL reconstruction surgery
Every person recovers with a different timeline. It generally takes 10-14 days on an average to recover from the surgery. But in some people who have a job that requires more manual work, the recovery period may extend to 6 weeks. Full recovery after an ACL graft takes about a year.
Here’s what you can do to help it heal faster:
- Eating healthy food during this time is very necessary to meet the nutritional demands of the body. Eat healthy food – get five portions of fresh fruits and vegetables per day. Consume foods like egg, fish, legumes, beans. Try to avoid processed foods.
- Stop smoking as smoking halts the healing process of the wound.
- Practical help from friends and family for daily activities while you recover, such as driving, the weekly shop, or lifting heavier items, and also in keeping your spirits up.
- For resuming sports, you should consult your doctor and start with swimming or activities which do not involve too much twisting, jumping or turning.
- When you are trying to come back to your normal activities, you might not feel very active initially. So take small breaks in between and give yourself some rest. Try a little bit every day and walk by taking small steps. If you feel pain, you have probably just overdone it a little. Be easy on yourself and gradually increase your activities each day.
Follow-up after the anterior cruciate ligament (ACL) reconstruction surgery
After surgery, visit your doctor as per the following schedule:
- Follow up is important firstly, in 2-4 weeks and subsequently, once in 3 months, 6 months, 1 year and 2 years.
- Knee function is evaluated by the doctor and change in physiotherapy exercises may be advised.
- In case you observe that something doesn't feel normal, contact your doctor at the earliest.
Surgery Cost In Your City
References
- Shea, Kevin G, Carey, James L.Management of Anterior Cruciate Ligament Injuries: Evidence-Based Guideline.JAAOS - Journal of the American Academy of Orthopaedic Surgeons: May 2015 - Volume 23 - Issue 5 - p e1–e5
- Benjamin Ma C, Zieve D. ACL Reconstruction. Medline Plus. Medical Encyclopedia. NIH, U.S. National Library of Medicine. 2017 Apr 18
- Arnoczky SP. Structure and Biology of the Knee Meniscus. Biomechanics of Diarthrodial Joints. Chapter 6 - pp 177-190. Springer, New York. 1990
- National health Scheme, The United Kingdom. Knee Ligament Surgery: Overview. NHS-Conditions, 2018 Jun 14
- National Health Scheme, the United Kingdom. Having an operation: Before Surgery. NHS-Conditions. 2018 Feb 7
- Samitier G, Marcano AI, Alentorn-Geli E, Cugat R, Farmer KW, Moser MW. Failure of Anterior Cruciate Ligament Reconstruction. The Archives of Bone and Joint Surgery. 2015 Oct;3(4):220-40. Epub 2015 Oct. PubMed PMID: 26550585
- Royal College of Surgeons. Recover More Quickly. Patient care. Advancing Surgical care.