Summary
The uterus (womb) is one of the parts of the female reproductive system that undergoes frequent or cyclic changes. It is lined by cells that undergo periodic multiplication in order to support a viable physical environment to grow a baby within. Sometimes, these cellular multiplications may get affected and cause abnormalities or unwanted growth inside the womb. This may affect the ability to conceive. Dilation and curettage is a conventional treatment that has been carried out since ages to manage unwanted pregnancy or abnormal growths within the womb. However, its diagnostic role is questionable as there are newer technologies available to examine the uterus, for example, ultrasound, CT scans, MRI, and so on. Although it is still used as a standard procedure in gynaecological practice, there are various risks and complications associated with it that require careful management of the internal environment of the womb to avoid any damage to the surrounding structures.
- What are dilation and curettage
- Why are dilation and curettage done
- Preparations before the procedure
- How are dilation and curettage done
- Risks and complications of dilation and curettage
- Post-surgical care
- Precautions after dilation and curettage
- Prognosis of dilation and curettage
- Follow up after surgery
- Seeking support
What are dilation and curettage
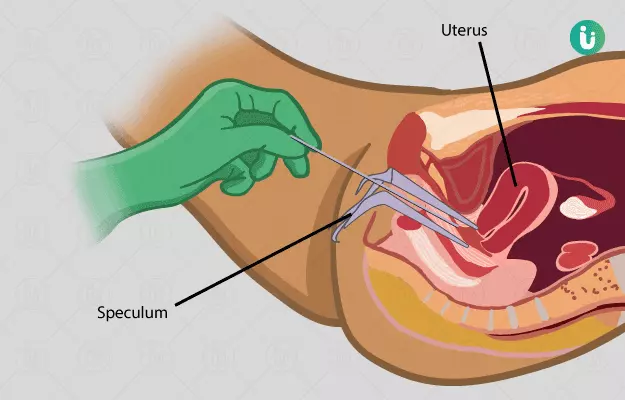
Dilation and curettage (D&C) is a procedure done to remove the tissue from the inner lining of your womb. During this procedure, the cervix or the entrance to the womb is dilated/ widened and a spoon-shaped instrument is inserted to slowly scoop out the infected tissue or remains of the developing or unborn foetus from the womb. As this instrument is inserted through the vagina, no cuts or openings are made surgically and no stitches are placed.
Curettage is one of the oldest gynaecological operations. This procedure has been replaced by a new method called ‘Hysteroscopy’ and the development of newer medications and other methods have made this procedure less popular among gynaecologists based on its risks. according to the World Health Organisation, it should only be done when manual vacuum aspiration (removal of tissue/foetus through suction) is unavailable during abortion procedures. It is the method of choice for abortion if you are in the first trimester of pregnancy.
Why are dilation and curettage done
The reason why your doctor will advise you this operation broadly falls under two major groups:
- Diagnostic (to check for the disease)
This procedure is performed to get a sample of the innermost lining of your womb (endometrium) that is tested for abnormalities under a microscope. - Therapeutic (to treat an illness)
This technique is used in order to get rid of the abnormal tissue in the womb.
They may overlap sometimes, for example, the diagnostic procedure may sometimes become therapeutic. The most common and more specific conditions of the womb in which your doctor will advise you for a D&C are:
- To remove/clear a tissue remaining in your womb after a miscarriage or abortion to avoid infection and heavy bleeding.
- Molar pregnancy removal, in which there is a tumour formation in your womb which mimics pregnancy and D&C is used to remove it.
- To treat excessive bleeding by clearing out any leftover placenta (a cord that gives nourishment to the baby from the mother during pregnancy) in the womb after birth.
- To remove cervical and uterine polyps (non-cancerous finger-like tissue growths).
Preparations before the procedure
- Speaking to your Gynaecologist
After the diagnosis, you will visit your gynaecologist and other specialists to check your fitness for the procedure. You will be informed about the possible outcomes, risks, tests, costs and essential precautions. - Medical Examination and Investigations:
You will undergo some tests, such as blood test, urine test and pregnancy test approximately one week before the procedure. If the procedure is advised to remove a fibroid (non-cancerous growths that develop around the uterus), you will be given medicine to shrink these beforehand in order to reduce bleeding. - Getting a date fixed for the procedure:
Your doctor will set you an appointment for the procedure as it is usually carried out in daycare surgery.
Getting ready for surgery
- Limitations on food and drinks.
Your doctor will advise you to stop eating and drinking a few hours before the procedure if it is done under general anaesthesia. This is to avoid any nausea after you gain consciousness. - Consent
Medical consent is a universal and the most important part of medical paperwork before any surgery. Here, your doctor will explain to you the risks and benefits of the procedure and any potential complications. You will be asked to verify by signing a declaration stating that you have agreed to the procedure after being fully informed about the surgery. - Arranging a carer
It is important that you clear your schedule before and after surgery for a few days in order to give yourself time to rest and recover. On the day of the procedure, it is advisable to arrange for someone to take you home after the treatment is done and look after you until you recover.
During the surgery
Instruments and medication:
- Medication will be used to dilate (open) the entry to your womb. This is to gain easy access to the womb. The most common medications include ‘Prostaglandins’. These are given either orally or placed directly into the vagina.
- Dilators
- Curettes
- Vacuum extraction device (to clear out the waste with suction)
Operation/procedure room:
D&C can be performed in a hospital, clinic or nursing home. You will be called on the same day when the procedure will be done. You will be given a clean sterilised (germ-free) dress and your vitals will be measured (BP, pulse, body temperature and breathing rate). Depending on your health and choice to remain awake or asleep during the procedure, anaesthesia will be given to you (local, epidural/spinal or general anaesthesia). The area to be operated will be prepared by numbing the region, dilating the birth canal and antiseptic application. You will now be ready to undergo the procedure.
How are dilation and curettage done
The steps of dilation and curettage are discussed below:
- Dilation of the cervix
This procedure is referred to as ‘cervical preparation’. This is done prior to curettage. It is usually done either with medication or with a small, rod-like device placed in the cervix. The medicines work by softening, thinning, and widening the opening of the canal to the womb. Rod-like devices known as dilators are usually placed a few hours before the procedure in order to absorb the moisture from the cervix and swell up, thus causing dilation. - Curettage of the Uterus wall
Recamier in 1843 invented curette (spoon/spoon on a long handle). This instrument is inserted into the womb and in swift scrapping motion, the tissues are evacuated. The cervix is then cleaned with an antiseptic and since no cuts are made, stitches are not placed in most cases.
If at any point you feel discomfort or pain during the procedure you can ask your doctor to stop.
Risks and complications of dilation and curettage
There are certain risks associated with this procedure, such as:
- Haemorrhage
It may occur after D&C. This could be due to accidental perforation of the womb or during the removal of cancerous cells. Symptoms will usually be dizziness, stomach pain and cramping after the procedure. You must visit your doctor immediately if you sense these symptoms or as mentioned earlier if you need to change your pads every 20 minutes. - Perforated uterus
It means that a surgical instrument through the uterine wall. This occurs in less than 1% of the women operated. It is not life-threatening and doesn’t require surgical intervention. You will be observed for several hours after the procedure to assure that there is no excessive bleeding or infection that requires further treatment. Laparoscopy for inspection of the belly through a small incision in the belly wall may be used if you are stable but there is suspected serious damage to the uterus, blood vessels or bowel. In the case of non-stop bleeding, you may need a hysterectomy (removal of the womb). - Infection
Infection is usually rare. - Asherman Syndrome
It is a condition in which aggressive scooping or an abnormal inflammatory reaction to this scraping can cause the formation of scar tissue in the uterus. This may lead to infertility in future and abrupt menopause. However, this is usually rare as nowadays, this procedure is carried out through laparoscopy or hysteroscopy, that make the inside of the womb visible to the doctor on a screen. - Chances of missing out on some disease
While scooping out the tissue in cases of any abnormal growths, some of the infected tissue may not get properly scraped out. Therefore, nowadays, in order to avoid this, doctors use a vacuum suction device that ensures maximum clearing of the womb. - Endometrial thickness
There is contradictory research that the thickness of the innermost lining of the womb is usually reduced in women with a history of D&C. Additionally, with repeated D&C, the lining keeps getting thinner. This may be particularly harmful to women of child-bearing age or perhaps planning to conceive in future.
Post-surgical care
- The procedure is usually carried out in a daycare surgery, which means you can go home after a few hours. However, if it is done under general anaesthesia, you may feel a bit groggy and need assistance to go back home.
- You will be given pain killers by your doctor as a standard procedure after the treatment to ease any discomfort.
- You will be able to continue your work after 1-2 days after D&C.
Precautions after dilation and curettage
There are a few things that should be taken care of after the procedure, such as:
- You will experience light cramps and mild menstrual bleeding after the procedure and may continue for a few days.
- You will be advised to use sanitary pads until the bleeding stops and not to do any strenuous activity shortly after the procedure.
- Your doctor will ask you to refrain from soaking in a bathtub, going in a pool, or have intercourse for a few days.
Prognosis of dilation and curettage
Dilation and curettage are fairly uncommon these days. Hysteroscopy uses a hysteroscope (a wand with a camera at its end) to look into your womb for any abnormalities or to remove or surgically burn any abnormal growth. This is due to the fact that procedures like manual vacuum aspiration (suction) are more beneficial than dilation and curettage in treating early pregnancy failure. Manual vacuum aspiration causes less blood loss, has a short treatment duration, short hospital stay and thus, more cost-effective. Also, no general anaesthesia is required and it has the least complications.
Follow up after surgery
You must visit your doctor every 2 weeks but once you are discharged, your doctor will inform you more about your follow up appointments.
Seek urgent medical advice in the following cases:
- Any heavy bleeding signs (if you have to change your sanitary pad every 20 mins).
- Any pieces of blood clots or leftover pregnancy tissue.
- Signs of fever or chills.
- Severe pain in the belly even after taking medication.
- Smelly discharge from the vagina.
Seeking support
It is essential that you must get complete information and counselling before you consider undergoing this procedure. This should be given voluntarily, confidentially and by a professional. In certain circumstances, it is necessary that you receive contraceptive (birth control) information as pregnancy right after this procedure may harm your health. All this should be facilitated by the nurse in the hospital or daycare centre and your gynaecologist. Family support and more importantly, the support of your partner will be highly beneficial before, during and after the procedure for physical, mental and emotional well-being.
Surgery Cost In Your City
References
- Macfarlane KT. The Indications For Dilatation and Curettage. 1964. Canadian Medical Association journal, 90(5), 364–369. PMID: 14122467
- Moroni R, Vieira C, Ferriani R, Candido-Dos-Reis F, & Brito L. Pharmacological treatment of uterine fibroids. 2014. Annals of medical and health sciences research, 4(Suppl 3), S185–S192. PMID: 25364587
- Newmann SJ, Dalve-Endres A, Diedrich JT, Steinauer JE, Meckstroth K, Drey EA. Cervical preparation for second trimester dilation and evacuation. 2010. Cochrane Database of Systematic Reviews 2010, Issue 8. Art. No.: CD007310.
- Myers-Bradley N. Dilation and Curettage. 2004. In: Encyclopedia of Women’s Health. Springer, Boston, MA.
- Davar R, Dehghani Firouzabadi R, Chaman Ara K. Dilatation and curettage effect on the endometrial thickness. Epub 2013 Apr 5. Iranian Red Crescent Medical Journal. 15(4):350-5. PubMed PMID: 24083012.
- National Health Services. Hysteroscopy: Procedure. NHS-UK. Health A to Z.
- Salam R. Neelofer R. Naserullah P. Comparative Study of Manual Vacuum Aspiration and Dilatation & Evacuation for the Surgical Management of Early Miscarriages: A Randomized Controlled Trial. 2016. Pakistan Journal of Medical and Health Sciences. 10. 183-185.
- Department of Health. Dilatation and Curettage (D&C). Healthy WA.
- World Health Organisation. Safe Abortion: Technical and Policy Guidance for Health Systems. 2012. WHO Guidelines. 2nd Edition.