Summary
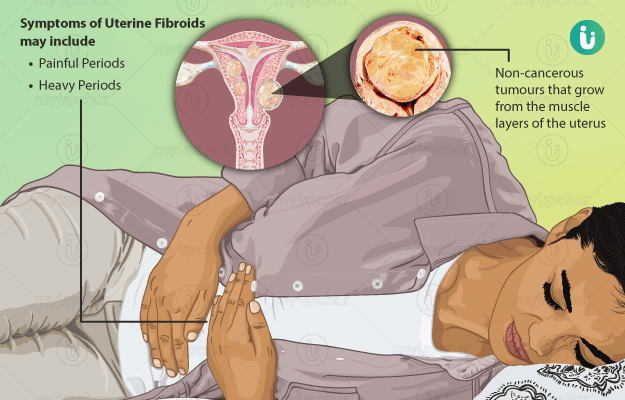
Uterine fibroids (also known as leiomyomas, uterine myomas, myomas, or fibromas) are non-cancerous (benign) growths that develop from the muscular tissue of the uterus (womb). A fibroid may be present anywhere in the uterus, such as in the, on the outer surface of the uterus, within the wall of the uterus, or attached to the uterine wall by a supporting structure resembling a stem (pedunculated fibroid). There may be a single fibroid or multiple fibroids of varying sizes. A fibroid may gradually grow over a number of years or may remain small for a long time and then suddenly grow rapidly. While the reason why fibroids develop is unknown, factors like heredity and hormones are thought to play a role in stimulating the development of fibroids. In some cases, fibroids may cause no symptoms at all, while in others, women may experience heavy periods and severe abdominal pain. There are certain medications that can relieve the symptoms of fibroids. However, these medicines may not prevent the fibroids from increasing in size. Usually, fibroids that are without any symptoms do not require any treatment. In symptomatic women, if the medications do not work as expected, surgery is the choice of treatment. The possible complications of fibroids mainly include severe pain, heavy bleeding, or twisting of the fibroid itself. Other complications that can occur include anaemia, urinary tract infections or in rare cases, infertility.

 OTC Medicines for Uterine Fibroids
OTC Medicines for Uterine Fibroids
 Uterine Fibroids articles
Uterine Fibroids articles
 Ayurvedic Treatment of Uterine Fibroids
Ayurvedic Treatment of Uterine Fibroids
 Diet for Uterine Fibroids
Diet for Uterine Fibroids
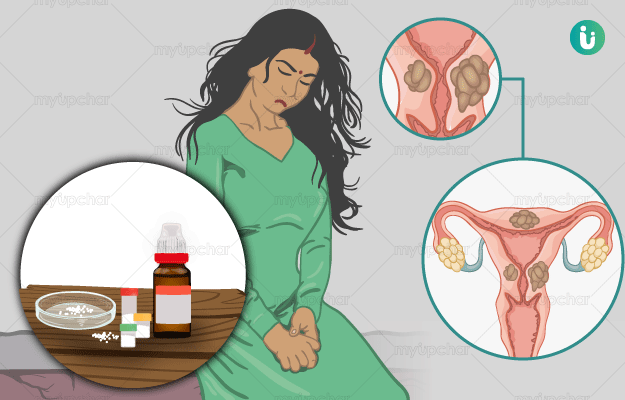
 Homeopathic Treatment of Uterine Fibroids
Homeopathic Treatment of Uterine Fibroids
































 Editorial Team
Editorial Team

 Dt. Akanksha Mishra
Dt. Akanksha Mishra
 Dr. Rachita Narsaria
Dr. Rachita Narsaria