Summary
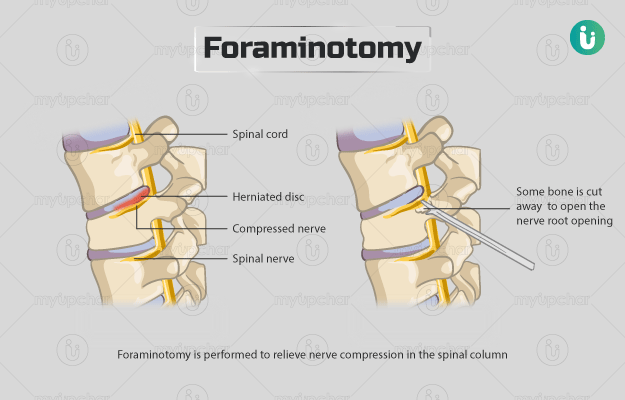
Foraminotomy is performed to relieve nerve compression in the spinal column. The spinal column is made up of a series of vertebral bones stacked one over each other vertically. Within the spinal column, a tunnel is formed that houses and protects the spinal cord. Spinal cord is a bunch of nerve fibres that receives and sends signals between the brain and other parts of the body. Nerves fibres exit the spinal column through openings called neural foramen in the vertebrae. Certain conditions such as foraminal stenosis narrow the neural foramen leading to compression of nerve fibres and symptoms that can affect the person's day-to-day activities.
Foraminotomy involves creating an incision in the skin over the affected part of the spine to access the compressed nerve. The surgeon then cuts and removes the blockage to relieve the symptoms of nerve compression. You will be discharged in one to three days following the surgery. Physical therapy will help regain your motion, and speed the recovery process.
- What is foraminotomy?
- Why is foraminotomy recommended?
- Who can and cannot get foraminotomy?
- What preparations are needed before foraminotomy?
- How is foraminotomy done?
- How to care for yourself after foraminotomy?
- What are the possible complications/risks of foraminotomy?
- When to follow up with your doctor after a foraminotomy?
What is foraminotomy?
Foraminotomy is a surgery that helps to relieve pressure on a spinal nerve.
The spinal column extends from the skull to the pelvis (located between the abdomen and thighs). It is a strong flexible structure made of 24 separate bones stacked vertically one above the other, with two additional bones fused at the end of the column. The column houses and protects the spinal cord inside a tunnel created in the vertebral bones and also supports body weight.
The spinal cord consists of several nerve fibres that send and receive messages from the brain. These nerves exit the spinal column through openings between the vertebral bones called neural foramen.
If you have a condition called foraminal stenosis, the foramen can become narrow and compress the spinal nerves. The compressed nerves can result in various symptoms such as pain, weakness, and a tingling sensation. The definite symptoms may depend on the position of the affected nerve. Surgeons recommend foraminotomy to widen the spinal foramen and remove any blockages, if present.
Why is foraminotomy recommended?
This surgery is indicated if you have foraminal stenosis - a condition caused by old age or conditions such as a slipped disc or cysts or tumours. The condition may result in some of the following symptoms that may affect your day-to-day activities:
- Muscle weakness
- Numbness or tingling sensation
- Difficulty holding things and walking
- Pain in the hands, shoulders, lower back, thigh, and calf
Other conditions that can be treated with this surgery include degenerative disc disease, herniated disc, and spondylosis.
Who can and cannot get foraminotomy?
The surgeon may not perform this surgery if you have any of the following conditions:
- Segmental instability (more than normal movements in one or more levels of the vertebrae)
- Segmental kyphosis (kyphosis at one or more spinal level)
- Cervical myelopathy (degenerative condition caused by compression of the spinal cord)
- Myelomalacia (softening of the spinal cord)
- Conditions of the vertebral body
- The surgery may also not be performed if you have recurrent disc and bilateral pathology
What preparations are needed before foraminotomy?
Prior to the surgery, your surgeon will ask you to undergo imaging tests like a magnetic resonance imaging (MRI) scan so that he/she can confirm your diagnosis. In addition, the surgeon will give you specific instructions to prepare for the surgery, such as:
- Share your medical history with your healthcare team, such as whether you have heart diseases, diabetes, or other medical problems
- Stop smoking as smoking prolongs the recovery period after the surgery
- Not to drink alcohol in excess
- Stop taking blood-thinning medicines one week before the surgery, e.g., warfarin, aspirin, naproxen, clopidogrel, and ibuprofen.
- Visit a physical therapist who will teach you a few exercises and instruct you on using crutches (to be used after the surgery).
- Not drink or eat anything six to 12 hours before the surgery. This is because anaesthesia administration is associated with a risk of vomiting.
- Inform the doctor if you get a flu, cold, fever, or other illnesses on the days leading to the surgery
- Arrange for a walker, cane, or wheelchair to use for a while after the operation
- Take a shower and remove body piercings, nail polish, and make-up before arriving at the hospital on the day of the surgery.
- Arrange for a family member, friend, or responsible adult to take you to the hospital and bring you back home after the surgery.
- Sign a consent form to grant your approval for the procedure.
How is foraminotomy done?
For the surgery, you will be asked to lie on your stomach. The surgery is usually performed with the assistance of X-ray imaging and microscope. The minimally invasive procedure for the surgery usually involves the following:
- You will be given general anaesthesia. It will make you fall asleep so that you do not experience any pain during the operation.
- The medical team will continuously monitor your vital signs (blood pressure and heart rate) during the surgery.
- The surgeon will make a small cut close to the affected portion of your spinal column.
- He/she will move aside the skin, muscles, and other adjacent tissues in the area to expose the affected foraminal opening.
- Then, the surgeon will remove (cut) any blockages that narrow the opening.
- Once the blockage is removed, the surgeon will put back the muscles and tissues in their place and stitch up the incision on your skin.
In a traditional procedure, the surgeon usually makes a large incision. This procedure may be performed with other surgeries, such as a laminectomy, to relieve nerve compression. You will be discharged to home in one to three days. During your hospital stay:
- You will be able to sit up and get out of bed in about two hours following the surgery.
- You may feel some pain after the surgery, for which a nurse will provide you with some medicines.
- Your surgeon will advise you to stop performing certain activities (e.g., bending your neck if foraminotomy was performed in the neck region) that can affect the operated area. If you have had surgery on the neck, you would be asked to wear a soft neck collar to prevent bending your neck.
- You will be allowed to continue your regular diet.
How to care for yourself after foraminotomy?
The surgeon will give you the following warnings and instructions for taking care of yourself at home after the surgery:
- You may experience numbness, pain, or weakness for a while after the surgery. This is completely normal and will resolve on its own.
- Your bones may require three to four months to heal. However, the time required for complete healing can extend up to a year.
- Make sure to keep your incisions clean and dry for at least five to seven days following the surgery. Ask your surgeon if you want to take a shower. If you do, the surgeon may tell you to cover the operated area with plastic film.
- Avoid sitting in the same position continuously for more than 20 to 30 minutes.
- The surgeon may ask you to wear a back brace.
- While picking up things, avoid bending from your waist; instead, bend from the knees and crouch down.
- Avoid strenuous activities and heavier work for a few months.
- Avoid driving during the initial two weeks after the surgery or until your surgeon allows you to.
- Your surgeon may recommend physiotherapy to help you recover quickly, regain your body’s ability to move comfortably, and maintain a good back posture.
When to see the doctor?
Inform the surgeon immediately if you experience any of the following:
- Fever with a temperature of ≥101°F (38.3°C)
- Chills
- Swelling
- Problem in controlling bowel movements and urinating
- Breathing difficulty
- Chest pain
- Yellow or green discharge from the operated site
- Loss of sensation in your arms (in case of neck surgery) or feet and legs (in case of lower back surgery)
- No improvement in back pain or increased pain that is not relieved with medicines
What are the possible complications/risks of foraminotomy?
The operation is successful in 80% to 90% of individuals; however, there is a small risk that the surgery may not provide relief from your symptoms. In addition, foraminotomy is also associated with a few complications, such as:
When to follow up with your doctor after a foraminotomy?
Your surgeon will provide you with a schedule for future follow-up visits. During the follow-up, the surgeon will conduct x-ray test to check the condition of your spine.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Surgery Cost In Your City
References
- Johns Hopkins Medicine [Internet]. The Johns Hopkins University, The Johns Hopkins Hospital, and Johns Hopkins Health System; Foraminotomy
- Cleveland Clinic [Internet]. Ohio. US; Spine Structure and Function
- Mount Sinai [Internet]. Icahn School of Medicine. New York. US; Foraminotomy
- Mount Sinai [Internet]. Icahn School of Medicine. New York. US; Foraminotomy
- UT Health Neurosciences [Internet]. The University of Texas Health Science Center at Houston. Texas. US; Foraminectomy
- McAnany SJ, Qureshi SA. Minimally invasive cervical foraminotomy. JBJS Essent Surg Tech. 2016 Jun 22;6(2):e23. PMID: 30237932.
- Papavero L, Kothe R. Minimally invasive posterior cervical foraminotomy for treatment of radiculopathy : An effective, time-tested, and cost-efficient motion-preservation technique. Oper Orthop Traumatol. 2018 Feb;30(1):36-45. PMID: 28929274.
- National Health Service [Internet]. UK; Before surgery
- University of Rochester Medical Center [Internet]. University of Rochester. New York. US; Spine surgery patient guide
- Singrakhia MD, Malewar NR, Deshmukh S, Deshmukh S. Clinical and Radiological Outcomes of Day-care Posterior Foraminotomy and Decompression of the Cervical Spine. Asian J Neurosurg. 2018 Oct-Dec;13(4):1118-1122. PMID: 30459879.