Summary
A haemorrhoidectomy is a surgery to remove severe haemorrhoids (piles) that are associated with uncomfortable symptoms like pain, itching, and lumps around the anus. A haemorrhoidectomy can be performed with closed, open, stapled or rubber band ligation techniques. The surgery requires the administration of a sedative (medicine that induces sleep) and takes not more than 45 minutes to complete.
This surgery is mainly done to provide relief from symptoms of inflamed haemorrhoids. However, the surgery is associated with a high rate of complications such as pain and bleeding from the anus, which may persist for a few weeks. The average recovery time after the surgery is 2 to 3 weeks.
- What is haemorrhoidectomy surgery?
- Why is haemorrhoidectomy surgery recommended?
- Who can and cannot get a haemorrhoidectomy?
- What preparations are needed before a haemorrhoidectomy surgery?
- How is a haemorrhoidectomy surgery done?
- How to care for yourself after the haemorrhoidectomy surgery?
- What are the possible complications/risks of haemorrhoidectomy surgery?
- When to follow up with your doctor?
What is haemorrhoidectomy surgery?
Haemorrhoidectomy is an effective surgery to remove extensive or severe haemorrhoids.
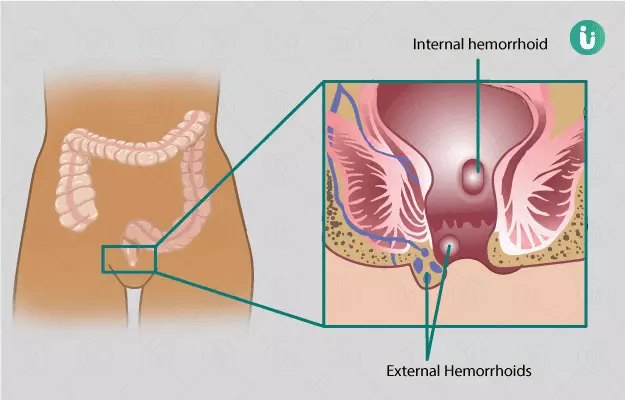
Haemorrhoids are tissues that are naturally present in the inside or outside of your anus (the back passage of the body). These tissues play an important role in faecal continence - the ability of your bowel to prevent leakage of faeces. However, when the pressure in haemorrhoidal veins increases, they enlarge, stick out, and bleed - the condition is called piles or simply haemorrhoids.
The most common cause of piles is constipation. Other causes include pregnancy, childbirth, obesity, and straining (during vomiting and weight lifting). Haemorrhoids are associated with the following symptoms:
- Pain around the anus
- Slimy discharge
- Red-coloured stool
- An itchy anus
- Lumps around the anus
Haemorrhoids or piles are of three types: internal, prolapsed, and external. Internal haemorrhoids are present inside the anus, prolapsed haemorrhoids bulge out of the anus, and external haemorrhoids are present outside the anus. Most haemorrhoids can be treated with non-surgical approaches such as medicines, diet, or exercise. Doctors may recommend haemorrhoidectomy when the haemorrhoids do not respond to non-surgical treatment or are too large, to provide relief from the uncomfortable symptoms. However, haemorrhoid surgery is associated with a high rate of complications and the condition can recur even after surgery.
Why is haemorrhoidectomy surgery recommended?
Doctors recommend this surgery to:
- Provide relief from persistent discomfort and pain of piles
- Stop bleeding from the anus
Who can and cannot get a haemorrhoidectomy?
Individuals with the following conditions can get this surgery:
- Large size internal haemorrhoids
- Internal haemorrhoids that do not respond to non-surgical treatments
- Large external haemorrhoids
- Both external and internal haemorrhoids
- Strangulated haemorrhoid, a condition where the anal sphincter, the muscle that guards the anal opening, interrupts the blood flow to the haemorrhoid (prolapsed) and compresses it
Haemorrhoidectomy is not recommended in people with the following conditions:
- Ineligibility for general anaesthesia due to medical conditions such as allergies, are allergic to certain medicines or have diseases of the heart, kidneys, or lungs
- Rectocele, a condition that causes the tissue that separates the vagina and the rectum (last part of your large intestine) to bulge
- Uncontrolled bleeding disorders (conditions such as haemophilia A, haemophilia B, and von Willebrand disease that impair the ability of blood to clot)
- Inflammatory bowel diseases (diseases that cause inflammation of the digestive tract) such as ulcerative colitis or Crohn’s disease
- Rectal varices (a condition wherein some veins in the rectum become enlarged) present with portal hypertension (increased pressure in the blood vessels (portal vein) that carry blood from the digestive organs to the liver)
- Baseline faecal incontinence (inability to control bowel movements)
What preparations are needed before a haemorrhoidectomy surgery?
You need to take into consideration the following things before a haemorrhoidectomy surgery:
- Inform your doctor:
Your doctor may ask you to temporarily stop taking medicines such as ibuprofen, aspirin, naproxen, warfarin, clopidogrel. Discuss with your doctor which medicines you can take till the time of surgery
Your doctor may give you instructions on when to stop eating and drinking before the surgery. Moreover, if asked to take any medicine just before your surgery, you should consume it with a minimum quantity of water as water is restricted. If you smoke, try to quit. Smoking can slow down wound healing.
How is a haemorrhoidectomy surgery done?
This surgery may be conducted in the surgeon’s consulting room or in the hospital operating theatre. Before starting the procedure, you may be given general anaesthesia to help you sleep during the procedure.
Haemorrhoidectomy surgery can be performed by any of the following methods: closed, open, stapled, or rubber band ligation haemorrhoidectomy.
- Closed haemorrhoidectomy: It is the most commonly used procedure to treat people with internal haemorrhoids. The haemorrhoids are removed with a sharp instrument, such as scissors, scalpels or even laser. The wound is stitched closed; the stitches typically disappear in 7-10 days. This procedure has a success rate of 95%.
- Open haemorrhoidectomy: The procedure for removal of haemorrhoid is the same as in closed haemorrhoidectomy; however, after haemorrhoid removal, the wound is kept open. This procedure is performed in cases where the position or number of haemorrhoids can cause difficulties in closing the wound or in cases where the chances of infection after the surgery are high.
- Stapled haemorrhoidectomy: The procedure involves the use of a circular stapling device that removes only the enlarged portion of the haemorrhoids. This procedure is performed in people with prolapsed haemorrhoids.
- Rubber band ligation: A rubber band ligation is mostly done for internal haemorrhoids. In this type of surgery, the doctor inserts an anoscope into your anus to view the haemorrhoid and with the help of a special instrument, will tie the base of the haemorrhoid with a rubber band, which cuts off circulation to the tissue. Due to this, in a few days, the hemorrhoid dries up.
The time taken for the procedure varies depending on the number and location of the haemorrhoids. The average time required to complete the procedure varies from 15 to 45 minutes.
After the surgery, you will be shifted to another room to allow you to recover from drowsiness caused due to general anaesthesia. The medical staff will insert a small gauze pad (thin cloth) into your anal opening. Unless you receive special instructions from the surgeon, do not remove the gauze pad until you have a bowel movement wherein it may come out on its own.
In addition, when you are still drowsy, you may be injected with local anaesthesia to relieve you from pain for 6 to 12 hours. After your surgery, if you are not staying overnight in the hospital, you will be discharged once the drowsiness from general anaesthesia wears off and you have urinated (to make sure you do not have the complication of being unable to urinate after anaesthesia and surgery).
You will need to make an arrangement for someone to take or drive you home.
How to care for yourself after the haemorrhoidectomy surgery?
In general, it may take 2 to 3 weeks to recover after surgery.
You can expect the following things on returning home after the surgery:
- Pain in the surgical site. Take the medicines for pain as prescribed by your doctor.
- Bleeding after the first bowel movement. This occurs commonly after surgery. In case of rubber band ligation, bleeding may occur for up to a week or more after the surgery when the haemorrhoids fall off. However, it stops by itself.
If you have undergone the stapled haemorrhoidectomy surgery, you may experience less pain after surgery and have a shorter recovery period compared to the other surgical methods. However, the stapled haemorrhoidectomy is associated with a higher risk of haemorrhoid reappearances.
The doctor will give you the following dietary advice that needs to be followed at home after the surgery:
- Drink a lot of fluids, such as juice, broth (soup, liquid in which vegetables and meat have been cooked), and water
- Eat soft foods for the first few days after surgery
- Take stool softeners to have easy bowel movements
You can take care of the wound by doing the following:
- Use a gauze pad or sanitary pad to absorb bleeding or drainage from the wound. Make sure to change it frequently.
- Talk to your doctor on when you can take a bath. Typically, you are allowed to shower on the same day of surgery.
In addition to the medicines prescribed by your doctor for pain relief, you can consider doing the following activities:
- Apply an ice pack, covered by a towel, on the wound to reduce swelling and pain for a maximum of 15 minutes. Covering the ice pack with a towel is essential to prevent cold injury to the skin.
- Take a sitz bath multiple times in a day. Sitz bath is a type of warm water bath wherein only your hip and buttocks are immersed in water.
Avoid any strenuous activities like pulling or lifting things until your wound has completely healed.
Depending on the work you do and the type of surgery that you have undergone, the doctor may advise you to rest for a few days. Most people are advised to rest for 1 to 2 weeks after surgery.
The most important benefit that you may receive after undergoing haemorrhoidectomy procedure is relief from itching, pain, bleeding, and discharge caused by haemorrhoids.
What are the possible complications/risks of haemorrhoidectomy surgery?
Possible risks associated with this surgery are:
- Occasional dizziness or weakness: These symptoms may persist for 7 to 10 days.
- Bleeding at irregular intervals: It may last for up to 4 weeks.
- Pain after surgery: Your doctor will prescribe medications for the same.
- Constipation: You need to take a high fibre diet to avoid it.
- Infection at the site of surgery: This is uncommon after the surgery. Inform your doctor if you experience symptoms like high temperature and redness at the surgery site.
- Excessive bleeding: Consult your doctor if you still experience this after 4 weeks of surgery.
- Loss of bowel control: This risk is very rare, but women with a history of damage to the anal sphincter (the muscle that guards the anal opening) or people with anal surgery are at a higher risk of this complication.
- Reoccurrence of haemorrhoids.
- Inability to pass urine
- Infection in the anal area
Inform your doctor if you have symptoms like:
- Fever above 38.5oC (101.3oF)
- Severe bleeding
- Constipation that persists longer than 3 days even after taking medicines
- Difficulty urinating
- Increased redness and pain
- Excessive swelling or discharge
When to follow up with your doctor?
You may be asked to follow up 2-3 weeks after surgery or as informed by your doctor before your discharge.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Find General surgeon in cities
Surgery Cost In Your City
Doctors for Piles surgery

Dr. P. Priyanka
General Surgery
4 Years of Experience

Dr. Piyush Jain
General Surgery
8 Years of Experience

Dr. Rajive Gupta
General Surgery
28 Years of Experience

Dr. Prity Kumari
General Surgery
References
- UCSF Department of Surgery [internet]. University of California San Francisco. California. U.S.A.; Hemorrhoidectomy
- National Health Service [internet]. UK; Haemorrhoids
- Fontem RF, Eyvazzadeh D. Internal Hemorrhoid. [Updated 2019 Nov 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan.
- The Association of Coloproctology of Great Britain and Ireland [internet]. Royal College of Surgeons of England. London. UK; Haemorrhoids (piles)
- King's College Hospital [internet]: NHS Foundation Trust. National Health Service. U.K.; Haemorrhoidectomy
- Oxford Radcliffe Hospitals [internet]: NHS Foundation Trust. National Health Service. U.K.; Haemorrhoidectomy
- American Academy of Family Physicians [Internet]. Leawood (KS). US; Hemorrhoids
- Health direct [internet]: Department of Health: Australian government; Haemorrhoidectomy
- Michigan Medicine: University of Michigan [internet]. US; Hemorrhoidectomy for Hemorrhoids
- National Cancer Institute [Internet]. Bethesda (MD): U.S. Department of Health and Human Services; NCI Dictionary of Cancer Terms
- Cristea C, Lewis CR. Hemorrhoidectomy. [Updated 2019 Dec 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan
- Hernandez A, Sherwood ER. Anesthesiology principles, pain management, and conscious sedation. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 20th ed. Philadelphia, PA: Elsevier; 2017:chap 14.
- Cohen NH. Perioperative management. In: Miller RD, ed. Miller's Anesthesia. 8th ed. Philadelphia, PA: Elsevier Saunders; 2015:chap 3.
- American Society of Colon and Rectal Surgeons [internet]; Rectocele
- American Society of hematology [internet]; Bleeding Disorders
- NYU Langone Health [Internet]. NYU Langone Medical Center. US; Types of Inflammatory Bowel Disease in Adults
- National Health Service [internet]. UK; Bowel incontinence
- Merchea A, Larson DW. Anus. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice. 20th ed. Philadelphia, PA: Elsevier; 2017:chap 52.
- Cameron JL, Cameron AM, eds. Current Surgical Therapy. 12th ed. Philadelphia, PA: Elsevier; 2017
- Darrah DM, Griebling TL, Silverstein JH. Postoperative urinary retention. Anesthesiol Clin. 2009 Sep;27(3):465-84.
- Huyck A, Broderick K. Hydrotherapy. In: Pizzorno JE, Murray MT, eds. Textbook of Natural Medicine. 4th ed. St Louis, MO: Elsevier Churchill Livingstone; 2013:chap 40.