Tympanoplasty is a surgical procedure that is done to repair a perforated eardrum using a piece of tissue. The surgery is employed in large perforations which cannot heal by themselves.
Investigations prior to tympanoplasty include blood tests, radiological tests and special hearing tests. The surgery is done under general anaesthesia and requires a few days of hospital stay.
Aftercare post-surgery is important to ensure proper healing and thereby restore the function of the ear.
- What is Tympanoplasty
- Indications for Tympanoplasty
- Contraindications for Tympanoplasty
- Preparations before Tympanoplasty
- What happens during Tympanoplasty
- Risks and complications of Tympanoplasty
- Aftercare, discharge and follow up
- Takeaway
What is Tympanoplasty
The ear consists of three parts - the outer, middle and inner ear.
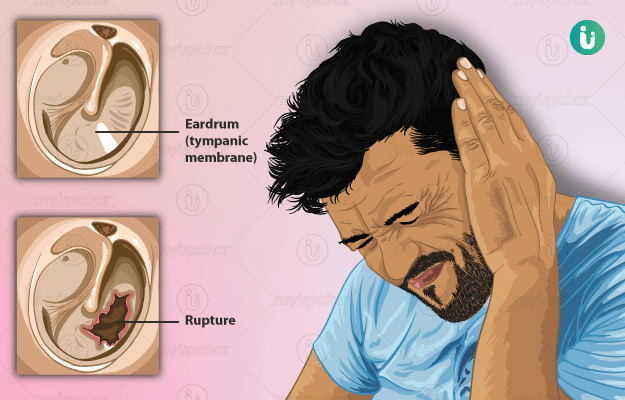
The middle ear mainly contains the eardrum (also called as tympanic membrane) and the ear ossicles which are three small bones that help conduct sound (bone conduction of sound).
The tympanic membrane is shaped like a flattened cone with a tip pointed inwards. It is well supplied with blood vessels and sensory nerves which makes it extremely sensitive to pain. This membrane receives sound vibration from the outer environment and transfers it to the ear ossicles.
(Read more: Ear pain)
When the tympanic membrane ruptures due to diseases of the middle ear or from certain offending agents (increased pressure, outside infection, etc.) the transmission of sound from the middle ear to the inner ear is affected leading to a certain degree of deafness.
Usually, if the perforation is small and uncomplicated, the eardrum can heal itself. However, if the perforation is large and is associated with a focus of disease or infection, then healing does not occur leading to a lasting defect that could further result in permanent hearing impairment.
The repair of the eardrum using a graft of tissue to fill up the perforation is known as tympanoplasty. Tympanoplasty additionally also involves treating the ear ossicles, if diseased, to maximally repair the hearing loss.
Indications for Tympanoplasty
Typically, small perforations can heal on their own. However, tympanoplasty is advised in patients under the following circumstances:
- The perforation is large
- No active ear infection is present or the ear is “dry” for more than 3-4 months which is incurable by just antibiotics
- Malfunctioning ear ossicles
Contraindications for Tympanoplasty
Tympanoplasty has increased risks in the following circumstances:
- Active ear infection: the infection is continuously discharging pus and debris from the middle ear
- Caution is to be taken if it is the only hearing ear that is to be operated
- Since the procedure is done under general anaesthesia, certain pre-existing conditions such as diabetes, heart conditions, etc. which may increase the risk of anaesthetic-related complications may also result in a longer recovery period. Hence, these conditions are to be kept under control before proceeding with the surgery.
Preparations before Tympanoplasty
The procedure is usually done by an ENT surgeon. A detailed history of the patient is taken which includes the symptoms of the patient, history of any other illnesses (comorbidities) and medication history.
A physical local examination of the ear is done using an instrument called an otoscope. The otoscope helps visualise the inner anatomy of the ear. Through the otoscopic examination, the surgeon makes note of the following points:
- Size of the perforation
- Location of the perforation
- Any debris or discharge (pus or blood) is present
- Whether any active signs of infection are present
- Examine the other ear for comparison
Medications for any pre-existing conditions may be altered or stopped as per the surgeon's orders before the surgery.
Investigations before the surgery include:
- Complete blood count (CBC): to check the haemoglobin status and severity of infection
- A swab will be taken from the ear and will be sent for microbiological assessment
- Liver function test and kidney function test
- Coagulation profile
- Chest X-ray
- ECG
- X-ray, CT scan or MRI of the head with a focus on the ear may be taken to find out the extent of disease and involvement of the ear ossicles
- Audiometric tests: these are special investigations that are done to assess the hearing status of the patient. The diseased ear is tested and compared with the normal ear. In case both the ears are diseased the results are compared to the baseline results in a normal ear.
The patient may require a couple of days of hospital stay.
Prior to the day of the surgery, the patient is told to fast overnight. On the day of the surgery, the patient arrives at the hospital with all the relevant investigations and documents and gets admitted. The patient changes into the hospital attire and a final review of the patient is done by the surgeon and nurses before clearing for surgery. Written consent is taken from the patient after the surgeon has explained the technique of the surgery and the associated risks and complications. Any facial hair and hair around the ear, if present, is shaved off to ensure a clean operation field.
See Similar Category Medicines Here
What happens during Tympanoplasty
The patient is asked to lie down supine (on their back) on the operating table. The head is turned in such a way so that the ear to be operated on is facing upwards. A monitor is attached to track vitals (heart rate, blood pressure, oxygen saturation). An IV cannula is inserted through which medications for the procedure will be administered. The procedure is done under general anaesthesia.
There are two different approaches to tympanoplasty, depending on which part of the ear is used to gain access to the eardrum:
- Trans-canal approach: in this approach, the entire procedure is carried out through the ear canal. To get the skin for the tympanic membrane grafting, just a small incision is made behind the ear. The advantage of the procedure is that no external incision is required. However, due to limited vision of the eardrum only relatively small perforations can be fixed via this approach.
- Post auricular approach: in this approach, a curved incision is made at the auricle (the crease behind the ear). This approach gives a more complete view of the eardrum and, hence, is a very common approach employed.
Before placing the graft, the surgeon clears the ear of any residue of infection. Additional techniques are employed to repair or reconstruct the damaged ear ossicles. In some cases, a prosthesis may be implanted to serve the function of the ossicles.
The graft that is used to fill the perforation is taken from the patient's own body. The graft is a type of connective tissue most commonly taken from the covering of the temporalis muscle (a muscle present near the side of the head). Other grafts that may be used are cartilage, veins and fat. The graft can either be placed over the perforation (overlay technique) or below the perforation (underlay technique)
Once the graft is placed and secured, the surrounding incisions are sutured (stitched) and the ear canal is packed with medicated gauze. The entire surgery takes two to three hours to complete.
Risks and complications of Tympanoplasty
The risks and complications associated with tympanoplasty are:
- Excessive bleeding
- Incomplete removal of infection
- Perforation of the graft
- Injury to the brain or orbit
- Injury to the hearing nerve
- Injury to the apparatus responsible for balance in an individual
- Ringing sensation in the ear post-surgery
- Permanent and complete hearing loss
- Taste disturbances due to injury to the nerve responsible for taste which passes through the middle ear
- Paralysis of the facial muscles due to injury to the facial nerve (it runs in the middle ear)
- Complications related to anaesthesia
Aftercare, discharge and follow up
After the surgery, the patient is shifted from the OT and kept in an observation room for a few hours. Using a tuning fork the patient's ability to perceive sound is assessed. Post-operative pain is controlled via analgesics. Here, the patient is also checked for postoperative bleeding.
Once the patient is stable, they are shifted into the ward. The dressing of the ear is checked for excessive soakage. Once everything is deemed alright as per the surgeon, a discharge summary is prepared that contains relevant medications and advice on wound care. These typically include:
- Continue medication for pre-existing conditions, if any.
- Antibiotics and analgesics to prevent infection and pain, respectively. Topical preparations such as ear drops are prescribed, which are to be used once the ear pack is removed.
- Keep the ear dry by keeping a dry medicated piece of cotton in the ear
- The patient can take a bath, taking care that no water enters the operated ear
- Some amount of drainage from the operated ear is normal
- Swimming and air travel are not advised till complete healing of the eardrum
- Strenuous exercises and lifting weights are not advised until after two weeks of recovery, since these increase the pressure in the middle ear leading to reperforation
- The patient may feel clicking, popping and pain in the ear associated with a heaviness which will decrease over time as the ear heals.
Notify the doctor immediately if any of the following symptoms arise:
- Excessive bleeding or discharge from the ear
- Excessive pain
- Excessive dizziness and vomiting not controlled by medication
- Fever or pus discharge from the ear
- Sudden complete loss of hearing
The first follow-up usually occurs after a week when the graft uptake is assessed and any signs of infection are looked for. Subsequent visits are scheduled as per the doctor’s orders.
Routine activities may be resumed after two weeks of healing. However, air travel and swimming are to be avoided until complete recovery which may vary from six to twelve weeks. As the recovery progresses the patient's hearing ability improves and may reach near normalcy.
Takeaway
Deafness is an extremely debilitating disability. It is most commonly seen due to ruptured eardrums. Tympanoplasty is a surgical procedure that is used to mend eardrum perforations. The procedure is of short duration with a high success rate and limited complications. Proper post-operative care ensures a faster recovery with limited complications.
Find Otolaryngologist in cities
Surgery Cost In Your City
Doctors for Tympanoplasty

Dr. Varalakshmi Govindappa
ENT
22 Years of Experience

Dr. Anu Goyal
ENT
25 Years of Experience

Dr. Manish Gudeniya
ENT
8 Years of Experience