Summary
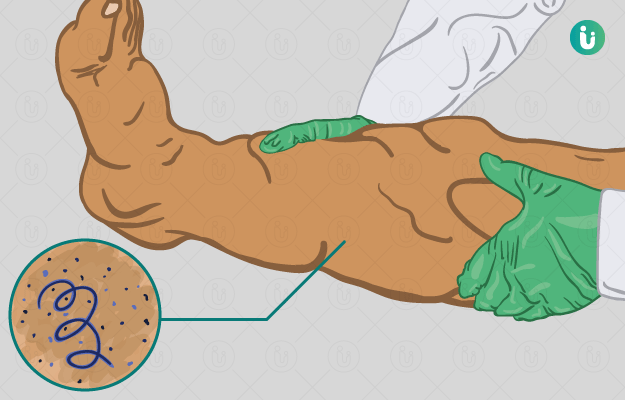
Filariasis is a parasitic infection transmitted by mosquitoes that affect the lymphatic system and the tissues under the skin. It is caused by a parasite, namely Wuchereria bancrofti, Borgia malayi and Borgia timori. The diseases caused by the first two parasites is a major health issue in India. The disease can affect both the genders and individuals of any age group. The infection is transmitted through mosquitoes.
Filariasis is very common in tropical countries, especially Africa, South Asia, India, South America and China. More than two-thirds of the cases are reported in Asia. Even though the number of cases has drastically reduced due to effective mass drug administration, infection rates are still high in some areas. Many people may be asymptomatic throughout life, whereas others may experience fever, body aches with painful swelling in the lymph nodes and genitalia, in the acute phase. People with chronic symptoms show massive swelling due to oedema in the lower limbs known as elephantiasis, a condition caused due to the obstruction of the lymphatic channels. Anti-parasitic treatment is prescribed after diagnosis is confirmed on a blood smear.

 Doctors for Filariasis
Doctors for Filariasis  OTC Medicines for Filariasis
OTC Medicines for Filariasis
 Lab tests for Filariasis
Lab tests for Filariasis Filariasis articles
Filariasis articles
 Ayurvedic Treatment of Filariasis
Ayurvedic Treatment of Filariasis
 Homeopathic Treatment of Filariasis
Homeopathic Treatment of Filariasis


































 Dr. Rachita Narsaria
Dr. Rachita Narsaria

 Dr. Laxmidutta Shukla
Dr. Laxmidutta Shukla