What is Calcium Deficiency?
99% of the calcium in our body is stored as hard tissue in form of teeth and bones. It is a crucial nutrient which is necessary for critical body functions such as transmitting messages through nerves, hormone secretion, contraction and expansion of blood vessels and muscle, most importantly it supports skeletal function.
Calcium deficiency is also known as hypocalcaemia. Untreated chronic hypocalcaemia raises severe concerns for complications like thinning of bones (osteopenia), weak bones in children (rickets) and excessive loss of bone density (osteoporosis). The best part about a calcium deficiency is that it is curable by modifying dietary habits.
What are its signs and symptoms?
It is difficult to identify calcium deficiency at initial stages. However, certain symptoms can be noticed once the condition starts to progress.
Early symptoms include:
- Numbness and tingling in the fingers, feet and legs
- Cramps and spasm in muscles (Read more: Muscle spasm treatment)
- Feeling of lethargy and extreme fatigue
Chronic calcium deficiency can affect several other body parts. Late symptoms include:
- Osteopenia and osteoporosis- proneness to fractures
- Dental problems-dental and enamel hypoplasia, blunted tooth root development, and delay of tooth eruption.
- Weak and brittle nails
- Dry and itchy skin – eczema
- Depression and Confusion
- Poor appetite (Read more: Loss of appetite causes)
- Abnormal heart rhythms (Read more: Arrhythmia prevention)
- Delay in blood clotting
What are its causes?
Minimum requirement of calcium is 700 mg per day for an adult and 1200 mg per day for an elderly.
Populations that are at a high risk for calcium deficiency are
- Women, esp. post-menopausal
- Elderly
- Adolescents
- Persons with lactose intolerance.
Some of the most common causes of calcium deficiency are as follows:
- Poor dietary intake
- Malabsorption due to digestive disorders like celiac disease
- Hypoparathyroidism
- High and low levels of magnesium
- High levels of phosphate
- People on medicines like phenytoin, phenobarbital, rifampin, corticosteroids as well as chemotherapy drugs
- Septic shock (Read more: Sepsis treatment)
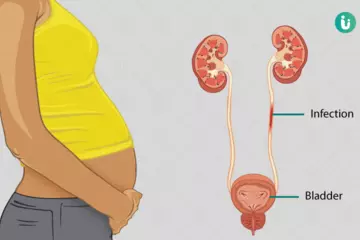
- Kidney failure
- Pancreatitis
- Low levels of vitamin D
How is it diagnosed and treated?
The physician first assesses the patients on the basis of clinical presentation and symptomatology. The next step to confirm clinical symptoms is to go for pathological testing which involves testing the levels of serum calcium, parathyroid hormone, serum phosphate, magnesium, 25-hydroxyvitamin D, and 1,25-dihydroxy vitamin D. The doctor might ask the individual to go for genetic mutation testing of the calcium-sensing receptor, the G protein subunit alpha 11.
Intake of calcium-rich diet not only treats hypocalcaemia but also prevents from having the condition in the first place. Rich sources of calcium are
- Milk and other dairy products- cheese, yoghurt, curd and paneer
- vegetables- spinach, broccoli, legumes- beans and peas
- Fortified cereals, whole grains
- Calcium-rich mineral water
- Seafood, lean meats and eggs
- Nuts, seeds, soya products- tofu
Calcium supplements prescribed by the physician can also help in improving calcium levels.
- Avoid self-treatment
- Avoid taking high doses of calcium – as doses are based on body weight. High doses can cause digoxin toxicity Remember, the calcium deficiency didn’t develop overnight and hence it will take time to recover.
- Calcium supplements may interact with certain medications- blood pressure and cholesterol-lowering medicines, antibiotics- tetracyclines and fluoroquinolones.
Additionally, calcium injections may be required based on individual condition. It may take from one month to six months to completely treat hypocalcaemia depending upon the severity.

 Doctors for Calcium Deficiency
Doctors for Calcium Deficiency  OTC Medicines for Calcium Deficiency
OTC Medicines for Calcium Deficiency
 Calcium Deficiency articles
Calcium Deficiency articles








 Editorial Team
Editorial Team