Increased mobility could be caused by one or several factors mentioned below:
Bone loss: Loss of supporting bone around a tooth can result in mobility. The amount of mobility in teeth due to bone loss depends on several factors like severity and distribution of bone loss around a tooth structure, shape and size of the root and crown to root length ratio.
For example, a tooth having short and conical root will show mobility earlier than a tooth with long or curved root with the same amount of bone loss.
A tooth undergoing orthodontic treatment should be closely observed for possible apical shortening of the root, which may be the cause of increased mobility because bone loss is a multifactorial outcome and rarely occur as a single finding. Grade of tooth mobility does not necessarily depend on the amount of bone loss.
Trauma from occlusion: It occurs due to injury to the supporting structures as a result of the excessive occlusal load or abnormal occlusal habits like bruxism, clenching or inability of the tooth to withstand normal occlusal force.
Mobility caused by trauma from occlusion initially results in resorption of cortical bone, which leads to loss of collagen fibre support and later manifested in the form of widening of periodontal ligament space as an adaptation of increased occlusal force.
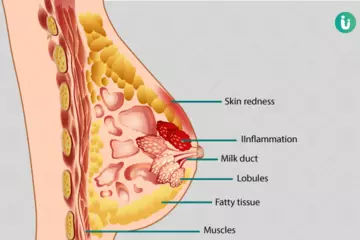
Inflammation: Spread of inflammatory process from the gingiva or periapical area of the tooth to the periodontal ligament leads to changes that may cause mobility. Inflammatory changes extending from an acute periapical abscess can cause mobility of the concerned tooth in absence of periodontal disease. Similarly, chronic gingivitis can also result in periodontal tissue damage and tooth mobility.
Periodontal surgery: The immediate effect of periodontal surgery can be tooth mobility but it is transient in nature and will eventually subside after a short period of time.
Jaw pathology: Jaw diseases affecting the alveolar bone or the roots of the teeth could result in tooth mobility for example osteomyelitis, cysts or tumours of the jaw.
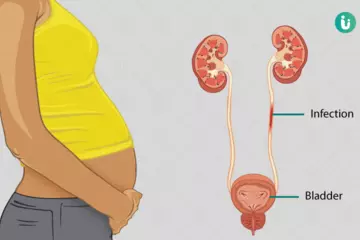
Pregnancy: Tooth mobility may increase during a certain physiological process of the body like pregnancy. Increased mobility could also be seen during menstruation or with the use of hormonal contraceptives pills. The associated factor for this mobility is physio-chemical changes in the body affecting periodontal tissues rather than periodontal disease.

 Doctors for Loose tooth
Doctors for Loose tooth  OTC Medicines for Loose tooth
OTC Medicines for Loose tooth