Summary
Biliary endoscopic sphincterotomy is an endoscopic procedure wherein an incision is made in the papilla of Vater and biliary sphincter for treating conditions such as bile duct stones, cholangitis, bile sludge and leakage, narrowing of the bile duct, and sphincter of Oddi dysfunction.
To prepare for the procedure, you should not eat or drink for at least six hours. Blood tests will be required, and the doctor will ask for your complete medical history. The procedure will be done under local anaesthesia and sedatives. You will be discharged in about three hours after the procedure, or you may need to spend the night in the hospital. Do not operate any machinery, or drive until the effect of the sedatives wears off. Some risks of the procedure include bleeding, perforation of surrounding tissue, and pancreatitis.
- What is biliary endoscopic sphincterotomy?
- Why is biliary endoscopic sphincterotomy recommended?
- Who can and cannot get biliary endoscopic sphincterotomy?
- What preparations are needed before biliary endoscopic sphincterotomy?
- How is biliary endoscopic sphincterotomy done?
- How to care for yourself after biliary endoscopic sphincterotomy?
- What are the possible complications/risks of biliary endoscopic sphincterotomy?
- When to follow up with your doctor after a biliary endoscopic sphincterotomy?
What is biliary endoscopic sphincterotomy?
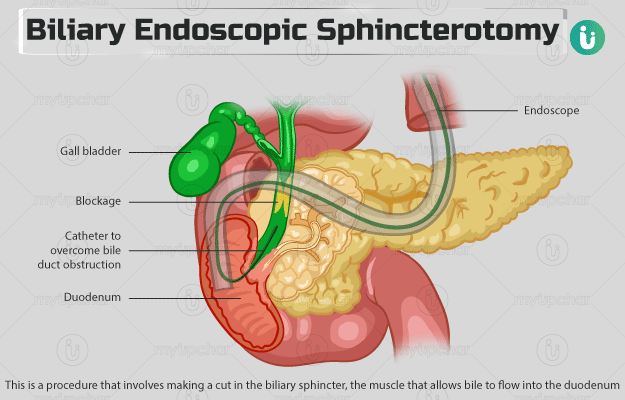
Biliary endoscopic sphincterotomy is a procedure that involves making a cut in the biliary sphincter, the muscle that allows bile to flow into the duodenum (the first part of the small intestine) along with a part of the bile duct (papilla of Vater).
Bile is a digestive secretion produced by the liver. It is stored in the gall bladder (a small pouch) and is released when you eat, particularly to digest food. Bile flows through the bile duct that opens into the duodenum through the papilla of Vater. The pancreas is another organ that produces digestive secretions and hormones, and it is attached to the bile duct with the help of the pancreatic duct.
The opening of the bile and pancreatic duct is guarded by the sphincter of Oddi, a muscular valve that allows the digestive juices to flow into the duodenum when there is food.
Biliary endoscopic sphincterotomy is done to remove stones or any other blockages obstructing the bile duct. In the procedure, an endoscope is passed into the digestive system to enter the papilla of Vater, and enlarge the opening by making a cut in it. The enlarged opening thus allows the flow of bile and removal of stones.
Why is biliary endoscopic sphincterotomy recommended?
The procedure can be recommended in the following conditions:
- Bile duct stones
- Bile sludge
- Cholangitis (inflammation of bile duct)
- Bile leakage
- Narrowing of the bile duct which may or may not be cancerous
- Sphincter of Oddi dysfunction (spasm of the sphincter, causing the digestive juices to backflow and lead to abdominal pain)
Symptoms of cholangitis include:
- Jaundice (yellowing of the eyes and skin)
- Upper right-side abdominal pain
- Pale-coloured stools
- Fever
- Chills
- Dark urine
- Nausea and vomiting
Symptoms of bile stones include:
- Fever
- Nausea
- Jaundice
- Vomiting
- Severe pain in the belly
Some of the symptoms of sphincter of Oddi dysfunction include jaundice and abdominal pain.
Who can and cannot get biliary endoscopic sphincterotomy?
The contraindications for the procedure include:
- Uncooperative/unstable person
- Bleeding disorders that cannot be corrected
- The wire of the sphincterotome (an instrument used during the procedure) cannot be placed correctly
What preparations are needed before biliary endoscopic sphincterotomy?
The following preparations are needed for a biliary endoscopic sphincterotomy:
- Your doctor will conduct a physical examination and order the following tests to make sure you are medically fit for the surgery:
- An electrocardiogram (ECG)
- Blood test
- You will need to share the following information with your doctor before the procedure:
- Your medical history
- Pregnancy status
- Any allergies
- A list of medicines that you take such as over-the-counter, homoeopathic, or herbal medications
- You will be asked to stop taking any blood thinners like clopidogrel, warfarin, or aspirin before the procedure.
- If you have diabetes, the dose of your diabetes medicines will need to be altered as you cannot drink or eat for some hours prior to the procedure.
- Fasting is recommended for at least six hours before the procedure to give the doctor a clear view of your digestive system.
- You will have to sign an approval form if you agree to the procedure.
- Arrange for a friend, family member, or responsible adult to take you home after the surgery.
How is biliary endoscopic sphincterotomy done?
Once you arrive at the hospital, the hospital staff will ask you to undress and wear a hospital gown and disposable underwear. They will start an intravenous line in your arm to provide you with essential fluids and medicines during the procedure. Different devices will be attached to you to monitor your oxygen level, pulse, heart rhythm, and blood pressure. Your throat will then be numbed with the help of a local anaesthetic throat spray. A sedative (medicine that makes you drowsy but keeps you awake) and painkiller will be administered to you intravenously.
A mouth guard will be put in so that an endoscope (duodenoscope, a specialised endoscope for this procedure) can be passed via your mouth. In the examination room, the following steps are performed for the procedure:
- You will lie on your left-hand side, and an endoscopist (an individual trained in using the endoscope) will put the endoscope in your mouth once you are drowsy. He/she will pass the endoscope from your mouth to your stomach and then to your duodenum.
- Some air will be blown into the stomach so the surgeon can better view inside your body. The internal image, as seen by the endoscope, will be shown on a screen inside the room.
- The doctor will insert a very narrow tube in the endoscope through which he/she will inject a special dye and take X-ray images of your bile and pancreatic duct.
- Using the image, the doctor will make a cut at the papilla of Vater in your body and extend it towards your biliary sphincter with the help of a sphincterotome (a tube with a cutting wire at its end). This will enlarge the opening of the bile duct.
- If gall stones are present, the doctor will either remove them with the endoscope or crush and push them in your small intestine, through which, they are easily eliminated via stools.
- Finally, the doctor will remove the endoscope.
The procedure normally lasts for about an hour. After the procedure, the medical staff will shift you to the recovery room. After an hour of rest in the recovery area, you will be asked to sit on a chair and will be provided with a liquid to drink.
You will be allowed to go home in about three hours after the procedure, or you may need to stay overnight.
How to care for yourself after biliary endoscopic sphincterotomy?
Once you reach home, you will need to take the following care:
- You may feel bloated and experience soreness at the back of your throat for a day after the procedure. However, they will subside on their own and you won't need any medicines.
- You should eat light meals for a day.
- Avoid driving, resuming work, or operating machinery for about 24 hours until the effect of the sedative lasts.
- Take rest after your discharge for the remaining part of the day.
- Do not drink alcohol until you are under the effect of the sedative.
When to see the doctor?
Meet the doctor immediately if you see the following symptoms:
- Blood in vomit
- Fever
- Severe abdominal pain
- Shortness of breath
- Black stools
What are the possible complications/risks of biliary endoscopic sphincterotomy?
Some of the possible complications include:
- Bleeding
- Inflammation of the pancreas
- Infection
- Perforation (a hole formed in any of the regions through which an endoscope was passed)
- Cholangitis
- Recurring bile duct stones
- Biliary stricture
- Cholecystitis
When to follow up with your doctor after a biliary endoscopic sphincterotomy?
Follow up appointments will be needed after the surgery to monitor your progress. You will be informed about the follow-up schedule at the time of your discharge.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Find Gastroenterologist in cities
- Gastroenterologist in Gurgaon
- Gastroenterologist in Bangalore
- Gastroenterologist in Chennai
- Gastroenterologist in Jaipur
- Gastroenterologist in Ahmedabad
- Gastroenterologist in Noida
- Gastroenterologist in Mysore
- Gastroenterologist in Visakhapatnam
- Gastroenterologist in Hyderabad
- Gastroenterologist in Pune
Surgery Cost In Your City
Doctors for Biliary Endoscopic Sphincterotomy

Dr. Rishabh Gupta
Gastroenterology
6 Years of Experience

Dr. Paramjeet Singh.
Gastroenterology
10 Years of Experience

Dr. Nikhil Bhangale
Gastroenterology
10 Years of Experience

Dr Jagdish Singh
Gastroenterology
12 Years of Experience
References
- Koksal AS, Eminler AT, Parlak E. Biliary endoscopic sphincterotomy: techniques and complications. World J Clin Cases. 2018 Dec 26;6(16):1073–1086. PMID: 30613665.
- MUSC Health [Internet]. Medical University of South Carolina. US; What is ERCP?
- The Royal Bournemouth and Christchurch Hospitals [Internet]. NHS Foundation Trust. National Health Service. UK; Endoscopic retrograde cholangiopancreatography (ERCP)
- Gabbrielli A, Pezzilli R, Uomo G, Zerbi A, Frulloni L, Rai PD, et al. ERCP in acute pancreatitis: what takes place in routine clinical practice? World J Gastrointest Endosc. 2010 Sep 16;2(9):308–313. PMID: 21160762
- Johns Hopkins Medicine [Internet]. The Johns Hopkins University, The Johns Hopkins Hospital, and Johns Hopkins Health System; Cholangitis
- Michigan Medicine [internet]. University of Michigan. US; Bile Duct Stones
- Guy's and St. Thomas' Hospital: NHS Foundation Trust [Internet]. National Health Service. UK; Having an ERCP
- Hull University Teaching Hospitals [Internet]. NHS Foundation Trust. National Health Service. UK; ERCP (Endoscopic Retrograde Cholangiopancreatography)
- Oxford University Hospitals [internet]: NHS Foundation Trust. National Health Service. U.K.; Endoscopic retrograde cholangiopancreatography (ERCP)
- York Teaching Hospital [Internet]. NHS Foundation Trust. National Health Service. UK; Having an ERCP
- Royal Berkshire Hospital [Internet]. NHS Foundation Trust. National Health Service. UK; Endoscopic retrograde cholangiopancreatography (ERCP)
- Northern Devon Healthcare [Internet]. NHS Foundation Trust. National Health Service. UK; Advice Following your Endoscopic retrograde cholangiopancreatography (ERCP)