Summary
Cataracts occur when certain changes in the constitution of the eye lens cause it to become opaque and now allow light to pass through it. It develops gradually and leads to poor vision and vision loss. The removal of cataract is known as cataract surgery.
The eye lens is made up of an outer capsule, middle cortex and an inner nucleus. Depending on the region affected, cataracts can be of three types – capsular, cortical and nuclear cataracts.
Ageing is the most common reason for the development of cataracts. However, other factors that contribute to the formation of a cataract include UV ray exposure, malnutrition or other nutritional deficiencies, smoking, diabetes, and trauma.
Signs of a cataract include blurring vision, sensitivity to light, especially night glare, and colour fading.
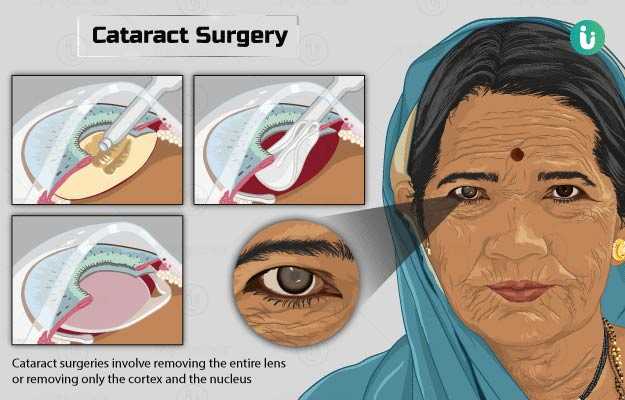
Cataract surgeries involve removing the entire lens with the outer capsule (intracapsular), removing only the cortex and the nucleus (extracapsular), and phacoemulsification (where the contents of the lens are broken down and then drawn out). The procedure may take about 30 minutes to complete, and you will be allowed to go home after the surgery.
- What is cataract surgery?
- Why is cataract surgery recommended?
- Who can and cannot get cataract surgery?
- What preparations are needed before cataract surgery?
- How is cataract surgery done?
- How to care for yourself after cataract surgery?
- What are the possible complications/risks of cataract surgery?
- When to follow up with your doctor after a cataract surgery?
What is cataract surgery?
A cataract surgery is a procedure that is done to treat cataract. Cataract is a condition in which the eye lens gradually becomes opaque, and makes one unable to see clearly. During cataract surgery, the cloudy lens is removed and is replaced with a synthetic lens.
In humans, the eye lens is located behind the coloured portion of the eye (the iris). Through the lens, light is focussed on the retina where the image of the object forms. This image is then sent to the brain via the optic nerve which tells you what you are seeing. The opacification of the eye lens makes it unable to focus light on the retina, which then leads to vision problems.
Cataract occurs due to changes in protein and water content of a lens, which are its key components.
It usually occurs as a normal part of ageing and forms slowly - over the course of several years. With age, the eye lens accumulates a certain brown-yellow pigment. This pigment restricts the passage of light through the eye, making it difficult to see. As cataract progresses, you may start to lose clear perception of colours too. Also, as you age, your eye lens may get thickened and lose its transparency that affects its overall functioning.
The lens is made up of three layers – an outer capsule, followed by a cortex within it, and a small nucleus at the centre. A cataract may form in either of these regions and, therefore, is named after the region. The three types of cataracts are as follows:
- Posterior capsular cataract: An individual with this type of cataract finds it difficult to read and drive in the daytime with discomfort in complete or full lighting (it is easier to see when pupils dilate in moderate-to-less light).
- Cortical cataract: The individual feels comfortable doing daytime activities; has discomfort and glare while driving at night; and has trouble reading.
- Nuclear cataracts: Individuals with nuclear cataracts find it difficult to work after sunset, recognise faces, and read number plates; reading is easier.
Cataract surgeries are of largely two types – intracapsular and extracapsular extraction based on whether the outer capsule of the lens is removed or retained. In intracapsular extraction, the whole lens along with the outer capsule is removed, whereas, in extracapsular extraction, only the lens is removed while the outer capsule is retained. Phacoemulsification is a technique used in most extracapsular extraction procedures; it involves breaking down the nucleus and sucking it out using specialised machines. This surgery has fewer complications, is less invasive and has a shorter recovery period.
Some other factors that could trigger cataracts include:
- UV light exposure
- Dehydration-related disorders from a young age.
- Smoking
- Malnutrition or nutritional deficiencies, such as low levels of vitamin C or vitamin E and carotenoids
- Atopic disorders (inherited tendency to develop allergic reactions)
- Diabetes
- Trauma – radiation, electrical or physical force leading to contusion (tear in the blood vessels that leads to blood leaking outside the blood vessel)
Why is cataract surgery recommended?
Your doctor may recommend this surgery if you have the following symptoms of cataract that interfere with your daily tasks:
- Blurred vision
- Reduced night vision
- Sensitivity to light (glare), especially while driving at night
- Difficulty seeing at night
- Fading or ‘yellowing’ of colours
Other special indications for cataract surgery are:
- Anisometropia (causes focus issues in the eye) that affects daily life
- The opacity of the lens inhibits the management of diseases in the posterior segment of the eye
- Conditions caused by the lens such as inflammation (uveitis) and phacomorphic or phacolytic glaucoma (increased pressure inside the eye caused by swelling of the lens or leaking of the protein in the lens through its outer capsule, respectively) or caused by other conditions like diabetic retinopathy (damage to the blood vessels in the retina due to diabetes).
- When the visual function and clarity are not satisfactory even after using spectacles or other aids
Who can and cannot get cataract surgery?
Cataract surgery is not done in people:
- In whom the surgery will likely not improve visual function
- Who do not wish to have surgery or will not consent to it
- If visual aids like spectacles or contact lenses give them a satisfactory visual function
- If their quality of life is not reduced without surgery
- Who are not safe (as per their health condition) to undergo surgery
- Who cannot get proper postoperative care.
- With conditions like rubeosis iridis (unusual blood vessels begin to develop on the iris), buphthalmos (enlarged eyeballs) and microphthalmos (extremely small eyeballs)
What preparations are needed before cataract surgery?
The following preparations are needed before a cataract surgery:
- Your doctor will assess your visual acuity (power of vision) using biometry measurements. This will help him/her to evaluate the power of the lens that needs to be implanted.
- Your eye lens will be assessed under high illumination and magnification to identify the location of cataract and your retina will be evaluated through a dilated pupil.
- Inform your doctor of your medical history and medications that you are currently taking. Your doctor may change some of your medications before the surgery.
- You may be asked to start eye drops prior to the surgery to keep away infections and swelling during and after the procedure.
- Avoid eating any solid food 6 hours prior to your surgery. Avoid wearing any face or eye makeup when you go for surgery.
- You would be asked to sign a consent form to give your approval for the procedure.
- You would be asked to make an arrangement for someone to drive you home after the surgery.
How is cataract surgery done?
Cataract surgery is most often performed in the outpatient department of clinics and hospitals. On your arrival, the doctor will put eye drops in your eyes to dilate your pupils. It will help the doctor visualise the lens and study the cataract. The eye drops will take effect after around half an hour.
Cataract surgery is generally performed under local anaesthesia (only the surgical region is made numb); however, if a patient is not suitably cooperative, general anaesthesia (where the individual is made to fall asleep) is given.
The doctor will give you the local anaesthetic in your eye. He/she may also give you topical antibiotics. Mostly, people are awake during the surgery and may see light and movements, but not what the doctor is doing to the eyes.
Cataract extraction is widely done by extracapsular extraction or phacoemulsification. The intracapsular technique is no longer used as the results are generally poor with higher postoperative complications as compared to the extracapsular technique.
Extracapsular cataract extraction
- The surgeon will make an incision of 10 to 14 mm on your cornea and remove the contents of your eye lens (the cortex and the nucleus) in one piece.
- The lens capsule will be left in place to hold the new intraocular lens.
- Next, the surgeon will insert a strong plastic lens (with a diameter of 6 to 7 mm) into the incision, either in the capsule or on it behind the iris.
Phacoemulsification
Phacoemulsification is considered to have a faster and more stable visual recovery, reduced complications, and is less invasive as compared to other techniques.
- During the procedure, the surgeon will make a small incision of about 2 to 4 mm at the edge of your cornea.
- He/she will introduce a viscoelastic substance in the front chambers of your eye to maintain space and protect your cornea.
- Next, the doctor will make a round and continuous opening in the capsule of your eye lens.
- Using ultrasound, the surgeon will fragment the cortex and nucleus of your eye lens and draw it out through the incision made earlier.
- The lens capsule will be left in place like in extracapsular cataract extraction. Once the lens capsule is empty, the doctor will inject more viscoelastic substance into the empty lens space until the new lens can be placed.
- He/she will move a plastic folding or even silicone lens through the small incision and place it in the capsule.
- If a larger lens is to be placed, the doctor may widen the incision.
- The small incision is self-sealing, and no sutures are needed. Once the procedure is done, the doctor will remove the viscoelastic material, check the incision edges to make sure that it is watertight.
- A certain amount of antibiotic solution will be injected into the chamber between the iris and cornea to prevent infections.
There are two main advantages when a small incision is taken.
- Less modification to the shape of the cornea, reducing the eye focus problems. Thus, helping achieve a better-unaided vision.
- Surgery is performed in a controlled and closed environment that leads to smaller changes in intraocular pressure.
Intracapsular cataract extraction
- The doctor will make an incision in your eye and remove your entire lens, including the capsule with the nucleus and cortex.
- This procedure requires a much larger incision and, therefore, the risk of loss of fluids in the eye (vitreous chamber fluids) are much higher risk along with postoperative complications. It is rarely performed.
- In this procedure, the lens may not be replaced with an implant. In such cases, glasses are used as no intraocular lens is inserted.
- This procedure can be performed for cataract removal in cases of trauma.
Cataract surgery will take about 30 minutes, and you can expect the following after surgery:
- The doctor will place a shield or eyeglasses over your eye for protection.
- You will be allowed to rest in the recovery zone for about 30 minutes, after which you will be allowed to go home.
How to care for yourself after cataract surgery?
You may be asked to keep the following things in mind for aftercare at home:
- Wear eyeglasses or protective gear (a shield) to protect the eye.
- Wear the protective covering on your eye even while sleeping.
- Do not press against your eye or rub them.
- Use eye drops as per your doctor’s instructions.
- Avoid doing any housework that requires heavy lifting.
- Avoid wearing eye make up for at least four weeks.
- Do not let soap or shampoo come in contact with your eyes.
- In the postoperative period, corticosteroid eye drops should be used in the eyes as per your doctor’s advice.
You will be advised on when you can resume driving, exercise, and other activities. Generally, patients are allowed to resume work in a week after a cataract surgery unless the work involves strenuous activities.
Overall, after the surgery you will be able to:
- Differentiate colours
- See things in focus
- See in bright light and have less trouble with glare
When to see the doctor?
You should visit a doctor immediately if you have the following symptoms in your eyes:
- Decreased vision
- Increased pain or redness
- Increased stickiness
What are the possible complications/risks of cataract surgery?
The possible complications of cataract surgery include:
- Pain that does not reduce even with medications
- Detachment of the retina (the retina moves up from the back of the eye)
- Retinal swelling
- Bleeding of the eye
- Infection of the eye
- Persistent swelling at the front or inside of the eye
- Reduced vision (endophthalmitis) or vision loss
- The lens implant moves out of position
- Other parts of the eye get damaged
When to follow up with your doctor after a cataract surgery?
The follow-up visit with your doctor will be a day after the surgery, a week, and a month to monitor recovery, healing and complications, if any.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Surgery Cost In Your City
References
- Harvard Health Publishing. Harvard Medical School [internet]: Harvard University; Considering cataract surgery? What you should know
- American Academy of Ophthalmology [internet]. California (U.S.A). Cataract Surgery
- Davis G. The evolution of cataract surgery. Mo Med. 2016 Jan-Feb;113(1):58–62. PMID: 27039493.
- American Optometric Association [Internet]. Missouri. US; Cataract
- Allen D, Vasavada A. Cataract and surgery for cataract. BMJ. 2006 Jul 15;333(7559):128–132. PMID: 16840470.
- Better health channel. Department of Health and Human Services [internet]. State government of Victoria; Cataracts
- Oxford University Hospitals [internet]: NHS Foundation Trust. National Health Service. U.K.; Cataract surgery
- National Health Service [internet]. UK; Cataract surgery