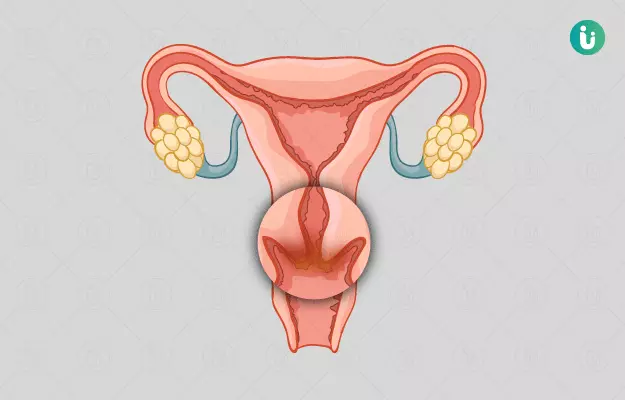
Cervicectomy is the surgical removal of the cervix - the lower-most part of the uterus that extends to the vagina. In addition to the cervix, surgeons may also remove nearby tissue, lymph nodes, and the upper part of the vagina during the procedure.
Also known as a radical trachelectomy, cervicectomy is done in younger women with early-stage cervical cancer, provided the tumour is no larger than two to three centimetres.
Women can opt to have children after a cervicectomy, though vaginal birth is not possible afterwards.
- What is a radical trachelectomy or cervicectomy?
- When is a radical trachelectomy or cervicectomy recommended?
- Preparations before a radical trachelectomy or cervicectomy
- How is a radical trachelectomy or cervicectomy done?
- Post-surgical care after a radical trachelectomy or cervicectomy
- Risk and complications of a radical trachelectomy or cervicectomy
- Follow-up visits to the doctor after a radical trachelectomy or cervicectomy
- Is there an alternative to radical trachelectomy/cervicectomy?
- Causes, symptoms and early detection of cervical cancer
What is a radical trachelectomy or cervicectomy?
Women with early-stage cervical cancer - where the tumour is no bigger than two centimetres and has not spread to the lymph nodes can opt for a radical trachelectomy.
Also known as cervicectomy, it is a surgical procedure in which the surgeon removes the cervix (also known as the neck of the womb because it connects the uterus to the vagina), the upper third of the vagina, and parametrial tissue (the tissue surrounding the lower end of the uterus).
During the surgery, the surgeon first removes some of the lymph nodes in the pelvis to check if cancer has spread beyond the cervix, this is known as pelvic lymph node dissection.
The womb or uterus is not removed completely, so the patient can still get pregnant.
When is a radical trachelectomy or cervicectomy recommended?
Radical trachelectomy is a surgical procedure usually done on younger women who have early-stage cervical cancer that is small (two centimetres or less in size) and who wish to become pregnant in the future.
Scientists in the US have introduced a potential new indication for radical trachelectomy. According to them, radical trachelectomy in pregnant women with cervical cancer may be a reasonable option in an attempt to save both the mother and fetus. However, the best management course for first stage cervical cancer in early pregnancy is still uncertain.
Preparations before a radical trachelectomy or cervicectomy
- Stop smoking at least 24 hours before the operation to reduce the risk of chest problems and to help the body cope with the general anaesthesia.
- Stop taking oral contraceptive pills six weeks before the operation.
- Stop taking any antiplatelet medicines such as aspirin or clopidogrel or any anticoagulant medicines such as warfarin or rivaroxaban before the surgery, as they may hamper the clotting of blood.
- Stop taking vitamin E 10 days before the surgery, as it may promote bleeding.
- Do not eat anything after midnight the night before the surgery. This includes hard candy and gum.
- Between midnight and up until 2 hours before the scheduled time of surgery, you may drink a total of 12 ounces or about 350 millilitres of water.
How is a radical trachelectomy or cervicectomy done?
There are different methods for doing a radical trachelectomy or cervicectomy:
- Vaginal radical trachelectomy (VRT) involves removal of the cervix and the nearby supporting tissue through the vagina.
- Abdominal radical trachelectomy involves removing the cervix and nearby supporting tissue through a large incision (surgical cut) in the abdomen.
- Laparoscopic radical trachelectomy uses a thin, tube-like instrument with a light and lens (called a laparoscope). Surgery is carried out through three to five small key-hole incisions. When the surgery is done laparoscopically, the cervix and the parametrial tissue (the supporting tissue around the cervix) are removed through the vagina.
At the end of the surgery, the surgeon partially closes the opening of the uterus with a special stitch that is like a “purse-string”. This stitch is strong enough to hold a pregnancy. Only a narrow opening is left to allow menstrual flow during monthly periods. A temporary urinary catheter (a hollow, flexible tube that collects urine from the bladder and drains it to a drainage bag) may be placed in the artificial opening to help keep it from closing.
Post-surgical care after a radical trachelectomy or cervicectomy
- The recovery period after a cervicectomy is at least five to six weeks.
- Avoid strenuous tasks and lifting, including lifting children or heavy household items, during this time.
- Do not engage in sexual intercourse for at least six weeks.
- Do not insert anything in the vagina for at least till six weeks. This includes tampons, and vaginal douching, etc.
- Patients are provided with anti-embolic stockings and made to walk around as soon as possible as it helps in maintaining good blood circulation thus preventing the formation of blood clots. Make sure you use them as directed by your surgeon.
- Drink an adequate amount of water, to avoid constipation.
Risk and complications of a radical trachelectomy or cervicectomy
Side-effects of the surgery may be seen immediately or a few weeks after the surgery. They may present as pain, blood in the urine or inability to empty the bladder completely. The major risks are rare and may present as:
- Pelvic Inflammatory Disease (PID): After pelvic lymph node dissection - in which the surgeon removes a few lymph nodes prior to surgery to check if the cancer has spread - there is a chance of infections which may lead to pelvic inflammatory disease. PID may present as constant foul-smelling discharge from the vagina, collection of lymph fluid (lymphocele) near the incision, formation of a blood clot in the leg (deep vein thrombosis), build-up of lymph fluid in the soft tissues (lymphoedema) in the lower limbs.
- Lymphoceles: These are swellings filled with fluid that might develop in the abdomen after the surgery. They are often naturally re-absorbed by your body, but if they increase in size, they may have to be drained by the surgeon using local anaesthesia and a needle.
- Problems with the urinary bladder: Some women will have difficulty in emptying their bladder after this surgery and may need to go home with a catheter in their bladder for several weeks.
- Menstrual problems: After the surgery, some women may find that the blood from their menstrual cycle is unable to come out of the uterus as the entrance to the uterus gets smaller. In this case, a minor surgical procedure has to be done to open the entrance to the womb. During this procedure, a Smitt sleeve (small tube) or a coil is inserted into the opening to the womb to keep the entrance open.
- Infertility: In the absence of a cervix, the tissue of the uterus can become narrow at the site of the surgery, which can make it difficult for sperm to pass through and fertilize an egg. If sperm can’t reach an egg, it can cause infertility.
- Miscarriage/pre-term delivery: There is a high risk of miscarriage in the second trimester (also known as late miscarriage) or a preterm delivery after a radical trachelectomy.
- If a woman becomes pregnant after a radical trachelectomy, the baby cannot be delivered vaginally and has to undergo a caesarean section.
- Postoperative infections: Chlamydia infections can lead to Pelvic Inflammatory Disease in the future. Women who have had chlamydia infections more than once are at higher risk of serious reproductive health complications like ectopic pregnancy (attachment of foetus on the outer layer of the uterus) and infertility.
Follow-up visits to the doctor after a radical trachelectomy or cervicectomy
- After the surgery, patients need to go for continuous follow-up appointments to ensure that there is no recurrence of cervical cancer.
- Patients need to come to the surgeon for giving samples of tissues at the site of surgery (similar to a Pap test procedure) and a colposcopy every three to four months for the first two to three years after surgery.
- Patients should get tested for HPV (Human papillomavirus) every five years. HPV vaccination should be administered to ensure there is no recurrence of the disease.
- Patients should contact their doctor immediately if they feel nauseous; notice smelly, itchy, yellow/green discharge from the vagina or from the surgery wound; experience burning pain while urinating or are unable to urinate; or get any lumps or swelling in abdomen.
Is there an alternative to radical trachelectomy/cervicectomy?
Radiotherapy (the use of X-rays to destroy cancer cells) can be given to treat cervical cancer, but it would prevent the affected woman from carrying future pregnancies. Chemotherapy along with radiotherapy can work effectively, but the woman would not be able to have children any more.
Causes, symptoms and early detection of cervical cancer
The female reproductive system comprises internal and external reproductive organs. The internal organs are the vagina, uterus, fallopian tubes, cervix, and ovary. The external structures include the mons pubis, pudendal cleft, labia majora and labia minora, vulva, Bartholin’s gland, and the clitoris.
Cancerous growth in the cervix is known as cervical cancer.
It is mainly seen in sexually active women between the ages of 30-45 years.
Human papillomavirus (HPV) is the cause of cervical cancers in about 99% of the cases. More than 70% of cervical cancer cases can be attributed to two types of HPV: HPV-16 and HPV-18.
Cervical cancer does not present with any symptoms during the early stages. Possible symptoms of more advanced disease may include:
- Abnormal or irregular vaginal bleeding. Abnormal bleeding can be seen as bleeding between regular menstrual periods, after sexual intercourse, after douching, after a pelvic exam or even after menopause.
- Pain during sex.
- Vaginal discharge that may be watery, thick, and possibly have a foul odour.
- Pelvic pain which is unrelated to menstrual cycle.
- Increased and painful urination.
Typically, women do not present with any symptoms in the case of early cervical cancer. Happily, regular screening through Pap smear and HPV tests can help detect precancerous cell changes early and prevent the development of cervical cancer. Other tests for the detection of cervical cancer include:
- Colposcopy is used to find abnormal cells that can become cancerous in the cervix, vagina, or vulva using special endoscopy equipment called a colposcope.
- Pelvic examination (womb, vagina, rectum and bladder) could be done under general anaesthesia for determining any signs of cancer. Blood tests, a CT scan, MRI scan, PET scan and a chest X-ray are used to help identify the amount and severity of cancerous tumours.
Find Obstetrician and Gynaecologist in cities
- Obstetrician and Gynaecologist in Bangalore
- Obstetrician and Gynaecologist in Mumbai
- Obstetrician and Gynaecologist in Ghaziabad
- Obstetrician and Gynaecologist in Chennai
- Obstetrician and Gynaecologist in Pune
- Obstetrician and Gynaecologist in Delhi
- Obstetrician and Gynaecologist in Hyderabad
- Obstetrician and Gynaecologist in New Delhi
- Obstetrician and Gynaecologist in Gwalior
- Obstetrician and Gynaecologist in Gurgaon