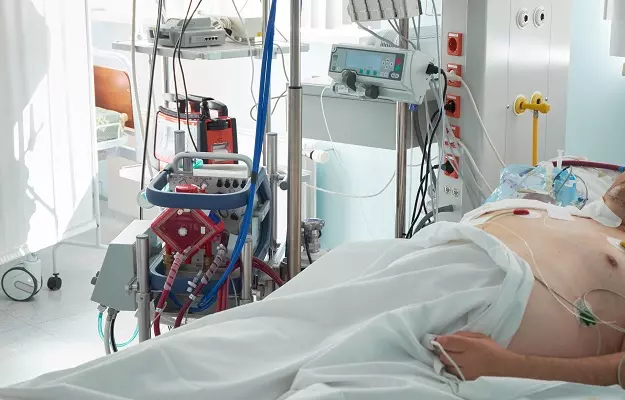
Extracorporeal membrane oxygenation, also known as ECMO, is a life support machine. The word "extracorporeal" means outside the body and "membrane oxygenation" means providing oxygen directly to the blood.
ECMO is required for people suffering from a severe and life-threatening illness which obstructs their heart or lungs from working properly. The ECMO machine pumps the blood and adds oxygen to it outside the patient’s body, thus giving rest to the heart and lungs.
When a person is connected to an ECMO, their blood flows through tubing into a machine, which acts as an artificial lung. This machine adds oxygen to the blood and takes out the carbon dioxide from it. Once the blood is oxygenated, it is warmed up to the body temperature and then pumped back into the patient's body.
Patients with severe COVID-19 have also been shown to benefit from ECMO in some cases. In April 2020, the US Food and Drug Administration approved the use of ECMO for COVID-19 patients. COVID-19, or coronavirus disease 2019, is a respiratory tract infection that started a pandemic in 2019, affecting millions of people across the globe.
In this article, we will talk about the uses, functions and the risks related to an ECMO machine.
- When is ECMO used?
- What are the different types of ECMO?
- How is an ECMO machine connected to a person?
- For how long is an ECMO machine used?
- What to expect when a patient is put on ECMO?
- What are the risks related to ECMO?
When is ECMO used?
Extracorporeal membrane oxygenation or ECMO is used for people who have a critical illness that has hampered the working of their heart and lungs. Some conditions in which ECMO is used are:
- It is used for people suffering from heart failure or lung failure.
- It is used during open-heart surgery.
- It is used during high-risk procedures being performed in the cardiac catheterization lab.
- It is used in patients who are awaiting a lung or a heart transplant, to keep the tissues of their body oxygenated.
- It can be used for a person with pulmonary hypertension and severe pneumonia.
- It is used before the placement of a left ventricular assist device (LVAD) in the heart.
- It can be used for patients of Acute Respiratory Distress Syndrome (ARDS).
What are the different types of ECMO?
There are two types of ECMO: veno-venous ECMO and veno-arterial ECMO. The most common sites for inserting a cannula (thin tube) are:
- The femoral artery or femoral vein in the groin area or the internal jugular vein in the neck, in the case of peripheral ECMO.
- The cannula is inserted into the right atrium and the aorta of the heart In the case of a central ECMO.
All the veins carry oxygen-depleted blood whereas the arteries bring back oxygen-rich blood.
Veno-venous (VV) ECMO
VV ECMO provides support to the lungs. In this type of ECMO, the surgeon inserts cannulas into the large vein either on the side of the neck or in the groin area at the top of the leg. This type of ECMO machine does not support the heart, so it can only be used for people who have a normally functioning heart. VV ECMO machine drains the blood from the vein with the help of the cannula. The machine then adds oxygen to the blood and removes carbon dioxide from the blood. The blood is then warmed according to the body temperature and then returned back to the right side of the heart through the cannula. The patient's heart then pumps the oxygen-rich blood to the rest of the body. This gives the lungs time to rest and recover.
Veno-Arterial (VA) ECMO
VA ECMO supports both the lungs and the heart. In this type of ECMO, two cannulas are inserted in the side of the neck or directly into the chest or into the groin vessels. VA ECMO machine drains the blood from the vein, adds oxygen to it, removes the carbon dioxide and then warms it according to the body temperature. Then the blood is returned to the artery (aorta) and is pumped into the whole body while bypassing the lungs and the heart. This gives time to the heart and the lungs to rest and recover.
How is an ECMO machine connected to a person?
A small surgery is done to access the arteries and veins if peripheral cannulation is done, however, for central cannulation, a sternotomy (cracking open the sternum, which is the middle bone of the rib cage) is done, as the cannula is inserted directly into the aorta and right atrium. To do the surgery, the surgeons sedate the patient and give pain killers and anticoagulants to reduce the clotting of blood.
Then the ECMO catheters are inserted into the required artery and veins. After the catheter is inserted, an X-ray is taken to ensure that the tubes are in the right place.
Since the patient is sedated, a nasogastric tube (NG feeding tube) is inserted from the mouth of the patient which goes till the stomach. This NG tube helps in providing nutrition to the patient. While the patient is on ECMO, they are monitored 24x7 by specially trained nurses and respiratory therapists.
The patient is given certain medications through the intravenous (IV) route while they are connected to the ECMO machine, which includes:
- Heparin is given to prevent the formation of blood clots
- Antibiotics are given to prevent infections
- Sedatives are given to minimize the movement of the patient
- Diuretics are given to increase the production of urine
- Electrolytes are given to maintain the balance of body fluid
Read more: What is fluid therapy?
For how long is an ECMO machine used?
Though it is not a treatment for any disease, an ECMO machine can help to save the life of a person who is in a critical condition - like someone experiencing heart failure or lung failure. An ECMO machine helps in providing support to the person while the doctors take care of the underlying injury or disease or until organs for transplant become available.
Some people may need the ECMO machine for a few hours while other conditions may take longer to get better, so the patient needs to stay connected to the ECMO machine for several days to weeks.
Doctors do multiple tests prior to the discontinuation of ECMO therapy, as they need to confirm that the heart and the lungs are ready to work on their own. Surgery would be required to remove the cannula from the body. Some people need ventilator support even after coming off an ECMO machine.
ECMO can help save many critically ill people who do not respond to usual life support options such as ventilators.
What to expect when a patient is put on ECMO?
A patient connected to an ECMO machine is admitted to the intensive care unit (ICU) until the machine is removed. In the ICU, the patient is monitored 24x7 by a team of nurses and doctors. The patient is connected to various monitors which measure the patient’s heart rate, blood pressure, and oxygen levels.
Doctors frequently test the patient’s blood in order to check the oxygen and carbon dioxide levels, which is also known as the blood gas test.
Patients on ECMO are given anticoagulant medications (blood-thinners) to make sure that the blood does not clot in the ECMO tubings. Doctors also need to keep an eye on the thinning of blood, as excessive thinning can lead to internal bleeding.
The doctors need to monitor the dose and frequency of sedatives, antibiotics, diuretics and painkillers, which are given to the patient throughout the course of treatment.
What are the risks related to ECMO?
The following complications can be seen in a person who is on ECMO:
- Since the patient is given anticoagulants to stop their blood from clotting in the tubing, there are chances of bleeding in such patients. Bleeding can occur inside or outside the body. It can get critical if the bleeding happens near or in the brain.
- There are chances of forming an infection at the sites where the tubes enter the body.
- There could be a formation of blood clots or air bubbles inside the ECMO tubing.
- During the ECMO, one of the two carotid arteries is tied to the ECMO machine, leaving only the other carotid artery which would supply blood to the brain. Since the blood supply is reduced, there are increased chances of stroke.
Doctors for What is ECMO or extracorporeal membrane oxygenation?

Dr. Mothiganesh gnanasekaran
Pulmonology
1 Years of Experience

Dr. Sayli Sawant
Pulmonology
6 Years of Experience

Dr. Devesh Kanoongo
Pulmonology
18 Years of Experience

Dr Viresh Mariholannanavar
Pulmonology
2 Years of Experience
References
- Pavlushkov E, Berman M, Valchanov K. Cannulation techniques for extracorporeal life support. Ann Transl Med. 2017 Feb;5(4):70. doi: 10.21037/atm.2016.11.47.
- University of California San Francisco [Internet]. San Francisco. California. United States; Extracorporeal Membrane Oxygenation (ECMO)
- University of Iowa Hospitals & Clinics [Internet]. Iowa City, United States; A family guide to ECMO
- American Thoracic Society [Internet]. New York, United States; What is ECMO?