Summary
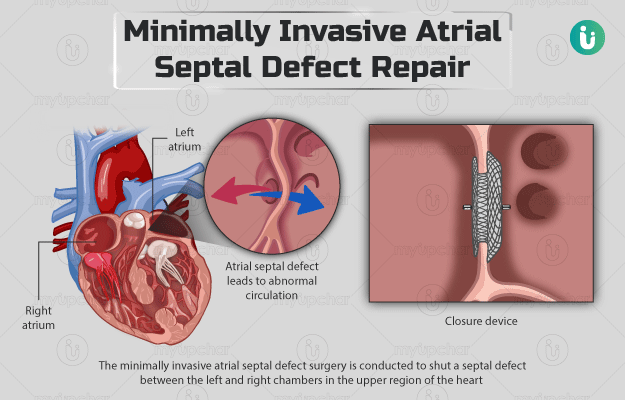
The minimally invasive atrial septal defect surgery is conducted to shut a septal defect between the left and right chambers in the upper region of the heart - atrial septal defect. This prevents the mixing of deoxygenated and oxygenated blood in the heart. If this condition persists, it can cause cyanosis (bluish colour of the skin due to inadequacy of oxygen-rich blood in the body). Before the surgery, your doctor will perform a few diagnostic tests to examine the septal defect properly. The surgery will be performed under general anaesthesia.
After the surgery, you will require special care for your wound. A follow-up is required after three months of surgery wherein the doctor will assess your healing.
- What is minimally invasive atrial septal defect (ASD) repair?
- Why is minimally invasive atrial septal defect repair recommended?
- Who can and cannot get minimally invasive atrial septal defect repair?
- What preparations are needed before minimally invasive atrial septal defect repair?
- How is minimally invasive atrial septal defect repair done?
- How to care for yourself after minimally invasive atrial septal defect repair?
- What are the possible complications/risks of minimally invasive atrial septal defect repair?
- When to follow up with your doctor after a minimally invasive atrial septal defect repair?
What is minimally invasive atrial septal defect (ASD) repair?
Minimally invasive atrial septal defect repair involves the shutting of an atrial septal defect (ASD) through keyhole incisions. The atrial septum is a valve situated between the upper chambers of the heart, i.e., the right and left atria, in a baby till birth. At birth, a baby has a small opening in the atrial septum that eventually seals. However, if the opening persists, deoxygenated blood (that flows from the body to the right atrium) mix with oxygenated blood (that flows from the lungs to the left atrium), increasing the amount of blood flowing towards the lungs. This damages the blood vessels of the lungs and leads to a reduction in blood oxygen levels, ultimately causing cyanosis. The latter manifests as early fatigue and congestive heart failure.
This surgery helps prevent cyanosis.
Why is minimally invasive atrial septal defect repair recommended?
Your surgeon will recommend this procedure if you have an ASD in your heart. A child with ASD may not show any symptoms and look healthy during his/her childhood. However, the following symptoms may appear during middle age or in childhood if the ASD is too large:
- Tiredness
- Cyanosis
- Slow growth
- Difficulty in breathing
- Shortness of breath during activities
- Breathing at a faster rate
- Abnormal heart rate
- Palpitations (feeling of the heartbeats) in adults
- Recurrent respiratory infections in children
Who can and cannot get minimally invasive atrial septal defect repair?
A surgeon cannot perform this surgery under the following conditions:
- Low body weight
- More than one defect in the heart
- Poor formation of heart structure
- High pulmonary vascular resistance (Resistance to the blood flow through arteries that carry blood from the lungs to the heart)
What preparations are needed before minimally invasive atrial septal defect repair?
You will need the following preparations before the surgery:
- Your healthcare provider will check for the severity of your ASD by a physical examination, tests, and reviewing your symptoms. Abnormalities may be detected in the blood flow of the heart when checking with a stethoscope. A murmuring sound indicates smooth functioning of the heart, whereas any abnormal sound or no murmur suggests a problem in the heart. You will be asked to undergo the following tests:
- Blood tests
- Urine tests
- Chest X-ray: The radiation waves used in this test can detect the structures inside the chest
- Echocardiogram
- Electrocardiogram (EKG)
- Tell your doctor about all the medicines that you take, including prescribed and non-prescribed medications, herbs, minerals, vitamins, and supplements. Your doctor may ask you to stop taking blood-thinning medicines before the surgery. These include aspirin, ibuprofen, warfarin, or clopidogrel.
- If you smoke, quitting smoking before the surgery can expedite your recovery.
- Inform your doctor if your alcohol consumption is more than one or two drinks a day.
- You will have to sign an approval or consent form to grant your permission for the surgery.
- Make sure to arrange for a friend or family member to drive you home after the procedure.
- You will be asked to maintain a fasting condition for a few hours before the surgery. This is advised to prevent vomiting under the effect of general anaesthesia (a medicine to keep you relax and pain-free during the surgery).
How is minimally invasive atrial septal defect repair done?
Once you reach the hospital, the medical staff will give you a hospital gown to change into, start an intravenous (IV) line in your arm to administer fluids and medicines and move you to the operating room on a stretcher. The surgery will be performed under general anaesthesia and involve the following steps:
- Electrodes for an EKG will be placed on your chest to monitor your heart continuously during the procedure.
- The surgeon will insert a small tube (catheter) into a blood vessel in your arm or groin area and advance it further into the blood vessel until it reaches your heart. He/she will conduct a dye-injected X-ray to visualise your heart.
- The surgeon will check the size of the hole by inserting a tube containing a balloon inside the upper chamber of your heart. He/she will inflate the balloon to measure the size of the hole.
- Thereafter, the surgeon will send in another tube with a device to close the defect in your heart. Some devices open like an umbrella to cover the defect, while some cover the hole on both sides.
- After placing the appropriate device, the surgeon will remove the tube and place a bandage at the insertion site of the catheter.
At some institutions, a mini atrial septal defect repair is done as follows:
- The surgeon will make about a 3-inch incision on the right side of your chest.
- He/she will conduct a heart-lung bypass. In this procedure, the heart is stopped and blood circulation in the body is continued through a heart-lung machine. The latter is connected to small tubes placed in an artery and vein in the right groin.
- Once you are attached to a heart-lung machine, the surgeon will open a space between your ribs using a soft retractor (a surgical tool used to hold back the underlying tissues).
- He/she will attach an ASD closure device to the catheter and insert it in the place at the defect.
- Once the device is fixed and the hole inside your heart is covered, the surgeon will disconnect the heart-lung bypass machine, remove the catheters and cover the site with bandages.
The surgeon may take about one to two hours to complete the procedure. After the surgery, you will be kept in the hospital for two to four days. During the stay, the following care will be taken:
- You will be given painkillers to reduce your post-surgical pain.
- The nurse will ask you to lie still on your back or place a pressure bandage to prevent bleeding from the incision site.
- You will be encouraged to drink ample fluids to flush out the dye from your body.
- Tests like a blood test, EKG, or chest X-ray will be performed to monitor your heart and health.
How to care for yourself after minimally invasive atrial septal defect repair?
Once you are at home after the procedure, you will need to take the following care:
- Wound care:
- Avoid applying cream, soap, or powder on the operated site. It can cause skin irritation.
- Keep the wound area clean by taking a shower or washing the area of operation. Make sure to pat dry the wound properly afterwards.
- Medications:
- You may have to continue taking painkillers for a while after the procedure.
- Your doctor may also suggest medications to prevent constipation that may occur due to pain medicines.
- You may also need medicines like clopidogrel and aspirin to prevent the formation of blood clots on the device after the surgery.
- Activities:
- You may be allowed to resume your daily activities seven days after the surgery. However, in case of a job that requires physical labour, seek advice from the doctor before going back to work.
- Driving is usually permissible within a week after the surgery.
When to see the doctor?
Visit or call your doctor right away if you experience the following symptoms after the surgery:
- Fever
- Rashes
- Chills
- Nausea and vomiting
- Unable to urinate
- Increased sweating
- Loss of appetite
- Redness, swelling, bleeding, or increasing pain at the incision site
- Opening of the wound
- Lack of energy
- Dizziness
What are the possible complications/risks of minimally invasive atrial septal defect repair?
This surgery is known to have the following possible risks:
- Damage to the arteries
- Allergy to anaesthesia
- Arrhythmia (abnormal heart rhythm)
- Infection
- Blood clots
- Bleeding at the catheter insertion point or collection of blood at this location
- Need for pacemaker implantation
- Allergic reaction to X-ray dye
When to follow up with your doctor after a minimally invasive atrial septal defect repair?
You will have a follow-up appointment with your surgeon three months after the surgery. Later on, yearly check-ups will be needed.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Surgery Cost In Your City
Doctors for Minimally invasive atrial septal defect repair

Dr. Manju
Cardiology
10 Years of Experience

Dr. Farhan Shikoh
Cardiology
11 Years of Experience

Dr. Amit Singh
Cardiology
10 Years of Experience

Dr. Shekar M G
Cardiology
18 Years of Experience
References
- UCSF Department of Surgery [Internet]. University of California San Francisco. California. US; Minimally Invasive Atrial Septal Defect (ASD) Closure
- Johns Hopkins Medicine [Internet]. The Johns Hopkins University, The Johns Hopkins Hospital, and Johns Hopkins Health System; Atrial Septal Defect Transcatheter Repair for Children
- Lucile Packard Children's Hospital Stanford [Internet]. Stanford Children's Health. Stanford University. California. US; Atrial Septal Defect (ASD) in Children
- Silvestry FE, Cohen MS, Armsby LB, Burkule NJ, Fleishman CE, Hijazi ZM, Lang RM, Rome JJ, Wang Y; American Society of Echocardiography; Society for Cardiac Angiography and Interventions. Guidelines for the Echocardiographic Assessment of Atrial Septal Defect and Patent Foramen Ovale: From the American Society of Echocardiography and Society for Cardiac Angiography and Interventions. J Am Soc Echocardiogr. 2015 Aug;28(8):910-58. PMID: 26239900
- Liegeois JR, Rigby ML. Atrial septal defect (interatrial communication). In: Gatzoulis MA, Webb GD, Daubeney PEF, eds. Diagnosis and Management of Adult Congenital Heart Disease. 3rd ed. Philadelphia, PA: Elsevier; 2018:chap 29
- Webb GD, Smallhorn JF, Therrien J, Redington AN. Congenital heart disease in the adult and pediatric patient. In: Zipes DP, Libby P, Bonow RO, Mann DL, Tomaselli GF, Braunwald E, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 11th ed. Philadelphia, PA: Elsevier; 2019:chap 75
- Sodhi N, Zajarias A, Balzer DT, Lasala JM. Percutaneous closure of patent foramen ovale and atrial septal defect. In: Topol EJ, Teirstein PS, eds. Textbook of Interventional Cardiology. 8th ed. Philadelphia, PA: Elsevier; 2020:chap 49
- Fraisse A, Latchman M, Sharma S-R, Bayburt S, Amedro P, Di Salvo G, et al. Atrial septal defect closure: indications and contra-indications. J Thorac Dis. 2018 Sep;10(Suppl 24):S2874–S2881. PMID: 30305947.
- Beth Israel Lahey Health: Winchester Hospital [Internet]. Winchester. Maryland. US; Atrial Septal Defect Repair in Children—Transcatheter Procedure
- Smith SF, Duell DJ, Martin BC, Aebersold M, Gonzalez L. Perioperative care. In: Smith SF, Duell DJ, Martin BC, Gonzalez L, Aebersold M, eds. Clinical Nursing Skills: Basic to Advanced Skills. 9th ed. New York, NY: Pearson; 2016:chap 26
- Neumayer L, Ghalyaie N. Principles of preoperative and operative surgery. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice. 20th ed. Philadelphia, PA: Elsevier; 2017:chap 10
- The Royal Marsden [Internet]. NHS Foundation Trust. National Health Service. UK; Consent for surgery
- National Health Service [Internet]. UK; Before surgery
- UT Southwestern Medical Center [Internet]. Texas. US; Atrial Septal Defect Closure
- Guy's and St. Thomas' Hospital: NHS Foundation Trust [Internet]. National Health Service. UK; Going home after your heart surgery