Summary
Osteochondral grafting is the surgical treatment of articular cartilage damage that may be caused by trauma or wear and tear. The articular cartilage is a tissue present at the end of bones in some joints. It lowers the friction between the bones when the joints move, however, it has a poor ability to heal. If an articular cartilage gets injured, you may start to feel pain while moving the affected joint. To check for the damage to the cartilage, your doctor will perform different tests before the surgery, including an MRI and X-ray.
During the surgery, the surgeon will remove the damaged cartilage and replace it with cartilage from a non-weight bearing area of the bone (autograft) or another tissue donor (allograft). The surgery is generally conducted under general or spinal anaesthesia and takes about an hour or two. You will need physical therapy after the surgery to promote healing and fast recovery.
- What is osteochondral grafting?
- Why is osteochondral grafting recommended?
- Who can and cannot get osteochondral grafting?
- What preparations are needed before osteochondral grafting?
- How is osteochondral grafting done?
- How to care for yourself after osteochondral grafting?
- What are the possible complications/risks of osteochondral grafting?
- When to follow up with your doctor after osteochondral grafting?
What is osteochondral grafting?
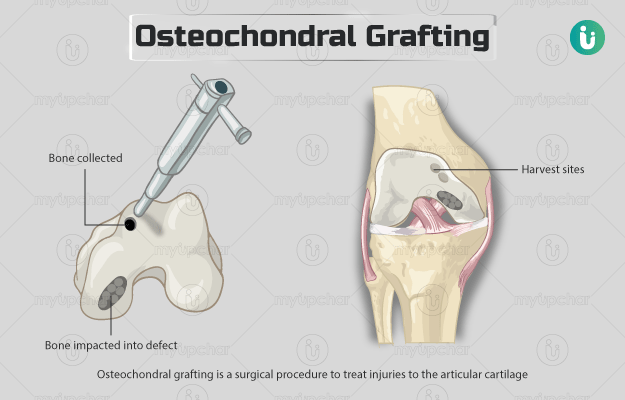
Osteochondral grafting is a surgical procedure to treat injuries to the articular cartilage. It is commonly performed on the knee but can be done in other joints as well.
Articular cartilage is 2-4 mm thick and present in synovial joints as a covering for the bone end. It does not contain lymph vessels, blood vessels, and nerves, and healing of the articular cartilage can occur only to a limited extent. A healthy cartilage lowers the friction in the joint and helps in the movement of the joint due to its smooth surface. An injury to the cartilage may make the surface rough and cause the bone to lose its protective cartilage cover.
A traumatic injury caused by direct impact or progressive degeneration (wear and tear) that causes loss in the function and structure of the cartilage are two types of damages to the cartilage. Loss of the articular cartilage gradually leads to wear and tear of the underlying bone and may cause arthritis.
Osteochondral grafting is recommended for treating injuries in the cartilage that expose the underlying bone. Due to poor healing of cartilage, the damaged cartilage may need to be replaced with a donor graft. The donor graft may be taken from another region of your body (autograft) or some tissue donor (allograft). Autografts are used for smaller defects, while an allograft may be used if the autograft is too small to treat the defect.
Why is osteochondral grafting recommended?
Osteochondral grafting may be required for the treatment of traumatic injuries of the articular cartilage and its progressive degeneration.
Osteochondral autografting is indicated in young and active people who have articular damage less than 4 cm2. It can be performed for articular damage in the knee, ankle, shoulder, hip, and elbow.
Osteochondral allograft does not have any size restrictions. It can be used in the following conditions:
- Osteoarthritis caused by injury to the joint with substantial damage to the cartilage
- Osteochondritis dissecans (death of a part of the bone just below the cartilage due to lack of blood supply)
- Death of bone tissue because of poor blood flow
The symptoms of articular cartilage damage include:
- Pain in joints
- Swelling
- Impaired joint activity
- Occurrence of joint “lock” or “catch”
- Joint stiffness
Who can and cannot get osteochondral grafting?
Contraindications for osteochondral allografts include:
- Altered bone metabolism in cases such as alcohol abuse, smoking, and chronic steroid usage
- Inflammatory joint disorders
- Early osteoarthritis in more than one joint
Relative contraindications (surgery can be performed but with caution) to osteochondral autograft include:
- Inflammatory disorder of the joints
- Lesions are equivalent to or larger than 8 cm2
- Severe osteoarthritis
- Absence of an appropriate donor site
What preparations are needed before osteochondral grafting?
You will need the following preparations before the surgery:
- Your doctor will check your joint for any pain, injury to the different tissues in the joint, decreased joint movement, fluid collection at the joint, and appropriate joint alignment.
- He/she will take your medical history and order the following tests:
- Magnetic resonance imaging (MRI)
- Arthroscopy (a technique used to see inside the joint)
- X-ray
- Electrocardiogram (ECG)
- Your doctor will ask you to share a list of all the medicines that you take, including any supplements and herbs.
- He/she may suggest you to discontinue medicines like aspirin, ibuprofen, warfarin, and other blood thinners before the surgery.
- Quit smoking before the procedure. This will reduce your chances of complications associated with osteochondral grafting.
- You may have to fast from midnight before the surgery.
- Arrange for a friend, family member, or responsible adult to drive you home following the procedure.
- The medical staff will ask you to sign an approval form if you agree to the procedure.
How is osteochondral grafting done?
Once you reach the hospital, you will be asked to put on a hospital gown. You may be given medicines or special stockings to wear for prevention of blood clotting. An intravenous line (IV) will be attached to a vein in your wrist or arm to provide fluids and medicines during the surgery.
You will be attached to different devices to check your vital signs. Right before the surgery, someone from the medical staff will administer antibiotics to you through a vein in your arm. This is done to prevent infections. The surgery will be performed under general (sleep-inducing medicine) or spinal anaesthesia (medicine that makes the lower half of the body numb, but keeps you awake).
You will be made to lie on your back on a medical table. An elastic band will be put on your thigh.
In the operating room, the following steps are performed:
- The surgeon will make an incision (cut) on the skin of the affected joint and then make an opening in the joint.
- He/she will take the exact measurement of the damaged cartilage and remove the affected cartilage the way an apple would be cored.
- The surgeon will then prepare the donor cartilage. If it is an autograft, cartilage from a healthy region, which is usually a non-weight bearing area of the bone, will be taken out in a similar manner as the damaged cartilage was removed. If it is an allograft, the cartilage is removed from a tissue donor.
- The allograft is cleaned well to remove any bone debris and tested for any transmission of disease. It will be shaped to a perfect fit to match the area of defect.
- The surgeon will then place the graft into the affected site and press it gently with fingers and a padded device to fit it perfectly.
- If required, the surgeon may use pins or screws to secure the graft.
- Thereafter, the surgeon will move your joint to check if the graft has fit appropriately.
- Finally, he/she will close the cut with staples or stitches. The latter may be absorbable or need to be removed in three to 20 days.
The surgery lasts for one to two hours. After grafting, you will be shifted to a recovery room. A nurse will give you pain medications and will check your vitals and dressing, if placed. You will be given intravenous fluids until you start eating on your own. You will likely be discharged in about three days.
How to care for yourself after osteochondral grafting?
You will need to take care of yourself in the following manner:
- Take the pain medication as required and directed by the doctor.
- You will need physical therapy to help in moving and strengthening the operated joint.
- If surgery is performed on the leg joint, you will be asked to avoid putting your full weight on the operated leg. Your doctor may suggest you to use crutches for a few weeks.
- You will not be able to play sports for a few months. Light sporting activities may be started in about four to six months if the healing progresses well.
- Your surgical bandage may be removed after five days. If you have stitches or staples, make sure to cover them when you have a bath. Avoid soaking the incision in water (e.g., tub baths, swimming pools, etc.) until it is healed.
- You may have swelling in your joints for about three months after the procedure. Keep the operated area raised, and apply ice for about 15 to 20 minutes a few times each day to manage it.
- Avoid lifting any heavy weights until your doctor tells you otherwise.
- Do not drive till your first follow-up.
- You may be able to resume work after the six-week follow-up with the doctor.
When to see the doctor?
Visit or call your doctor if you observe the following symptoms:
- Increased pain
- Swelling
- Fever
- Redness and warmth at the operated site
- Drainage from the surgical area
- The movement in the joint has decreased or remains the same after discharge from the hospital
What are the possible complications/risks of osteochondral grafting?
Some of the possible complications of osteochondral autograft implantation include the following:
- Osteonecrosis or death of the graft tissue
- Post-traumatic arthritis occurring at the donor site
- Overfilling of the donor area
- The graft does not heal well because of the damage at the operated area
- Bleeding
- Stiffness in the operated joint
- Injury to the nerves and blood vessels
- Infection
- Deep vein thrombosis
- Numbness at the surgery site
Osteochondral allografting can cause the following complications:
- Osteonecrosis of the graft
- Poor healing of the graft
- Transmission of disease from the donor graft
- Rejection of graft due to immune response
- Infection
When to follow up with your doctor after osteochondral grafting?
Follow-up visits will be scheduled after four to six weeks, three months, six months, and one year after this surgery. During the visits, your doctor will check the healing of your wound and take x-rays to examine the graft.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Surgery Cost In Your City
References
- Washington University Physicians [Internet]. Washington University in St. Louis. Missouri. US; Osteochondral Autograft & Allograft
- Fox AJS, Bedi A, Rodeo SA. The basic science of articular cartilage: structure, composition, and function. Sports Health. 2009 Nov; 1(6):461–468. PMID: 23015907.
- American Orthopedic Society for Sports Medicine [Internet]. Illinois. US; Articular cartilage injuries
- Orthoinfo [internet]. American Academy of Orthopaedic Surgeons. Rosemont. IL. US; Articular Cartilage Restoration
- Pisanu G, et al. Large osteochondral allografts of the knee: surgical technique and indications. Joints. 2018 Mar 13;6(1):42–53. PMID: 29675506.
- National Health Service [Internet]. UK; Cartilage damage
- The American College of Obstetricians and Gynecologists [Internet]. Washington DC. US; Preparing for Surgery
- Cleveland Clinic [Internet]. Ohio. US; Robotic-Assisted Joint Replacement
- U Health [Internet]. University of Utah. US; Hip cartilage repair and restoration
- American Academy of Family Physicians [Internet]. Kansas. US; Caring for Your Incision After Surgery
- University Hospitals Coventry and Warwickshire [Internet]. NHS Foundation Trust. National Health Service. UK; Knee reconstruction using osteochondral allografts
- UCSF Health [Internet]. University of California San Francisco. California. US; Recovering from Knee Replacement Surgery