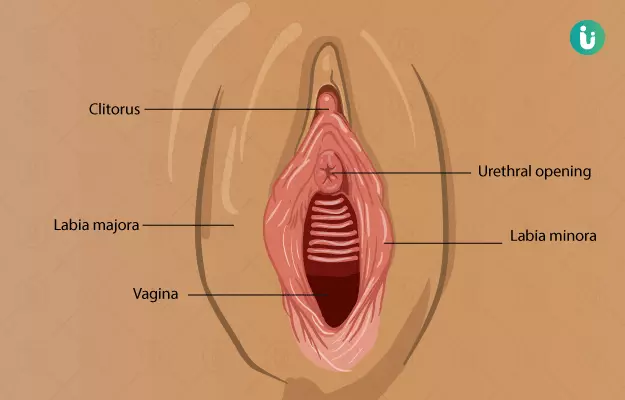
Now you know what is normal when it comes to your vagina and its health. Let’s move on to vaginal diseases and when to contact a doctor.
Vaginitis
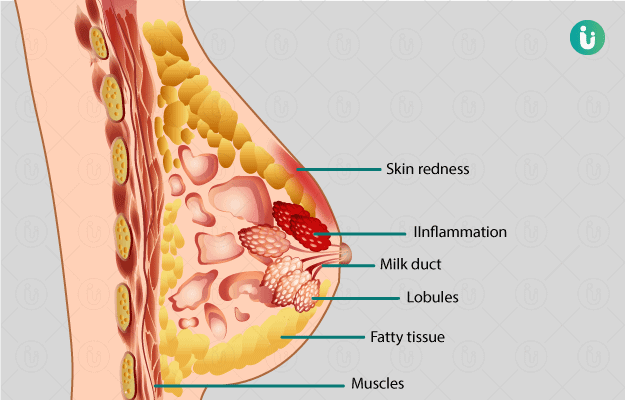
Vaginitis refers to the inflammation of the vagina. It is usually marked by swelling, itching and pain in the vagina and vulva. Though it could be caused by trichomoniasis, a sexually transmitted disease, the most common cause of vaginitis is the disruption of normal microflora.
Vaginitis is a common disease and a lot of women, especially in their reproductive age suffer from this problem.
So what causes this disruption in the normal bacterial population of the vagina?
Unprotected sex for once, may be responsible for this problem likewise having multiple sexual partners is. Some other factors that involved in vaginitis pathogenesis are:
Furthermore, it may be caused by an allergy to a soap or detergent.
In some cases, more than one of these factors is involved in the pathogenesis of vaginitis.
Symptoms:
Vaginitis symptoms may not be as apparent when caused due to a bacterial infection. However, you may notice a fishy smell in the vaginal discharge. A yeast infection may manifest as a thick yellow vaginal discharge that looks like cottage cheese accompanied by redness and itching.
In case of trichomonas-induced vaginitis, you may or may not experience any apparent symptoms, but when it does, it is felt as itching and burning sensation while urinating, sore vagina and an unpleasant smelling greyish green vaginal discharge.
Vaginitis is usually treated by over-the-counter medications which include vaginal pills and creams. However, it is preferable that you refer to a doctor to understand the cause of vaginitis before popping any pill.
Sexually transmitted diseases affecting the vagina
Apart from the already mentioned problems, vagina may also be affected by some sexually transmitted diseases. As the name suggests, they spread from unprotected sex and multiple partners. Here is a list of some of the most common STDs along with their apparent symptoms.
Genital herpes
Genital herpes is mostly caused by the herpes simplex virus, HSV-2, which is also responsible for causing cold sores. Oral herpes is mainly caused by HSV-1, it can spread to the vagina through oral sex. In case of pregnancy, it is important to get them treated as early as possible since they have been known to cause miscarriage and mortality in newborns.
Symptoms:
Genital herpes appears in the form of tiny recurring sores around the genital area which may be associated with pain, though, most people do not notice any symptoms of herpes or they go unnoticed.
It is difficult to completely treat herpes symptoms especially if it’s caused by HSV-2, though, recurrent infections can be managed by medications.
Chlamydia
Chlamydia is yet another STD that is caused by the bacteria Chlamydia trachomatis. Commonly spread by oral, vaginal or anal sex, chlamydia poses a serious threat to the female reproductive system and may increase the chances of ectopic pregnancy and cause difficulty in conceiving. It may also cause infertility and pelvic inflammatory disease when left untreated.
Symptoms:
Chlamydia is completely curable with the right antibiotics, provided that you do not miss your medicine and take care of your vaginal hygiene. Also, it is best that you abstain from sex until your partner has been cleared of chlamydia.
Gonorrhoea
Gonorrhoea is a bacterial infection of vagina and vulva, which is usually symptom-free. It is spread by a vaginal, oral or anal sex. Some of the symptoms of gonorrhoea include vaginal bleeding, painful urination and increased vaginal discharge. Some people may also notice painful bowel movements and sore and itchy anus.
Gonorrhoea infection can be transferred to the foetus, so if you are pregnant, it is highly important to get adequate medical help.
Untreated gonorrhoea infections may lead to permanent damage to the reproductive system in the form of scars in fallopian tubes, infertility and ectopic pregnancies.
Gonorrhoea is usually treated by antibiotics. However, drug-resistant strains of this bacteria are quickly growing If you notice the persistence of symptoms for long, talk to your doctor to get the right treatment as soon as possible.
Genital warts
Genital warts is a common problem that is characterised by the formation of small papular growth around the vaginal wall. However, in some cases, they may be too small to be noticed. Usually caused by human papillomavirus (HPV) it may be associated with itching in the anal area and the genitals. It is spread by coming in contact with infected warts during sex.
Although HPV cannot be completely cured, genital warts are easily removed by surgical treatment which may be done by freezing, electric currents or lasers. It is a completely safe procedure when done by a trained medical practitioner.
Since the virus is still not cleared out of the system recurrences are common.
Vaginismus
Vaginismus refers to the involuntary spasms that happen in vaginal muscles in response to penetration of any kind. This may occur while inserting tampons and during gynaecological examination. Rape, molestation and fear of pregnancy could be the responsible factors. Other factors which cause vaginal spasms are:
- STDs
- Urinary tract infections or UTIs
- Fear of getting hurt
- Childbirth
- Chronic pain syndrome
Vaginismus treatment includes psychotherapy and exercises to make one comfortable with penetration. Pelvic floor exercises and relaxation techniques are also used.
(Read more: Pain during sex)
Vaginal prolapse
Vaginal prolapse refers to a condition where the uterus, intestines and bladders come down through the vagina, sometimes even protruding out.
Common symptoms of vaginal prolapse include:
- Feeling a bulge in the vagina
- Constant pain in the lower back
- Difficulty in passing stools or urine
- Difficulty in intercourse
Vaginal prolapse may be caused due to old age or it may be due to obesity. Long-term constipation, pregnancy and delivery and lifting heavy weights are also some of the causative factors of vaginal prolapse.
It is usually treated by vaginal pessary (a device that fit inside the vagina to support the uterus) and pelvic floor exercises however they are not helpful in the long term and surgery is the best way to get the uterus and bowel back to their position.
Vaginal cancer
Vaginal cancer is marked by an abnormal growth of the vaginal cells. Though vaginal cancer is quite uncommon, age is one of the primary risk factors. It is characterised by vaginal bleeding, lump in the vagina, constipation, pelvic pain and painful urination. However, all of these symptoms may be indicative of other problems as well. It is important that you talk to your doctor before reaching any conclusion.
Vaginal cancer is usually diagnosed by a colonoscopy or a biopsy.