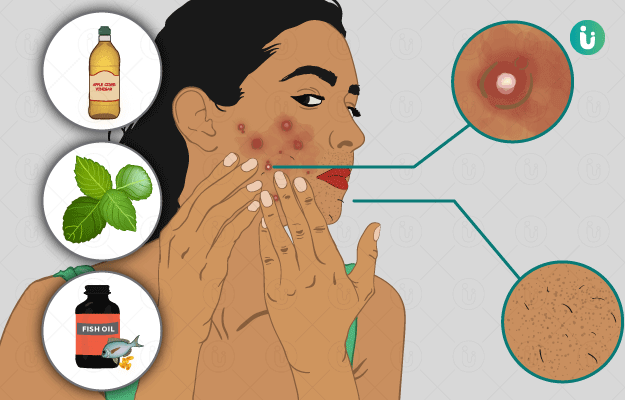
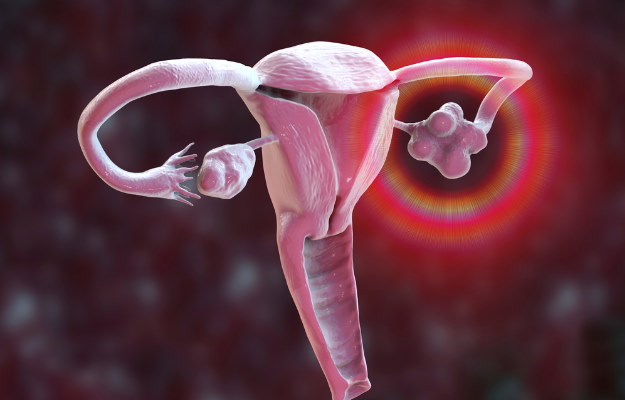
Polycystic ovarian syndrome (PCOS) is one of the most common hormonal disorders in women worldwide, affecting up to 13% of women of reproductive age. Caused by an excess of androgen hormones, PCOS usually presents with symptoms like irregular periods, painful periods, PCOS related excessive hair growth on the face and body, acne and weight gain. It is strongly associated with several metabolic disorders like insulin resistance, type 2 diabetes, hypertension, dyslipidemia and obesity as well as mood disorders and an impeded quality of life.
Research published in the European Journal of Endocrinology also suggests that women who have PCOS are more likely to suffer from sleep apnea than women who don't have this condition. This may be due to the fact that it is harder for women with PCOS to lose weight, and obesity and sleep apnea have a close connection.
Sleep apnea is a breathing disorder in which the patient's breathing stops and starts several times during sleep. This can happen for one of three reasons:
- Our brain sends signals to our breathing muscles to do their job. When these signals are interrupted a few times during the night, this is known as central sleep apnea.
- When the throat muscles relax during sleep and obstruct the upper airways, this is known as obstructive sleep apnea.
- A mix of central and obstructive sleep apnea is known as complex sleep apnea.
People with sleep apnea tend to snore and wake up several times during the night. This loss of sleep, in turn, may lead to further health problems such as unwanted weight gain.
Read more: Can I still get pregnant if I have PCOS?