Summary
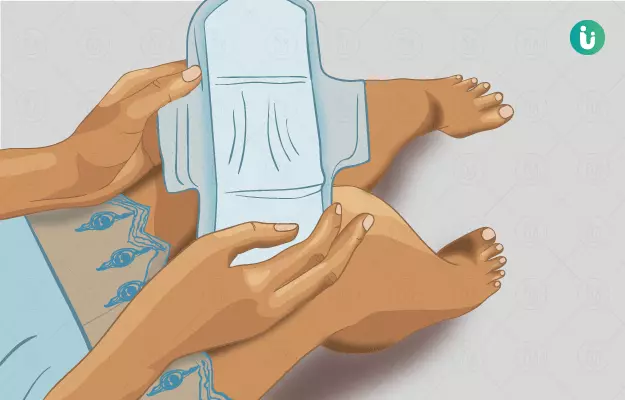
Following the onset of puberty, every woman expects to have her period once a month. While it may take a while for the menstrual cycle to regularise, over time, the period starts to appear in a regular pattern. A typical menstrual cycle lasts for around 28 days. It is common for the cycle to be slightly longer or shorter, and most women start to understand how their period cycle works. It is, however, not uncommon for them to have irregular periods.
Irregular periods are experienced when the duration or gap between two periods is not consistent. Some women have an extremely irregular cycle and do not know when the next period will arrive. Another common experience involves either very heavy or scanty bleeding.
Often, we tend to view period-related problems in a very generalised manner and believe that they can be treated using one universal method. However, various complications could cause irregular periods, and knowing the underlying problem can help address it optimally.
(Read more: How to induce periods)
- What are Irregular periods
- Causes and risk factors of Irregular menstruation
- Symptoms of Irregular menstrual bleeding
- Prevention of Irregular periods
- Diagnosis of Irregular menses
- Treatment of Irregular periods
What are Irregular periods
Menstrual cycles not only vary among women but may also vary with every month to pass. Some women may experience them infrequently while others may have them more often. Hence, periods can be irregular in the following ways:
- Menorrhagia
A common occurrence among women is a heavy period. A heavy menstrual flow can occur for several reasons, but when it becomes so severe that it hampers normal functioning, or continues for longer than usual, it is termed as menorrhagia. - Hypomenorrhoea
In some cases, women may have alarmingly short or scanty periods. Such a condition is commonly referred to as hypomenorrhoea. While hypomenorrhea occurs most widely either during menopause or at the onset of puberty, it can also sometimes occur in the regular course of the period. - Oligomenorrhoea
A woman’s period doesn’t always stick to the 28-day cycle. The normal range of a menstrual cycle can vary between 21 to 35 days. When a period is delayed further and does not occur beyond 35 days of the previous cycle, the woman is said to have a condition called oligomenorrhoea. - Amenorrhoea
Amenorrhoea is a condition when the period is missed altogether. Various reasons can lead to the condition, and treatments are suggested depending on its cause and nature.
Causes and risk factors of Irregular menstruation
Different types of irregularities in periods have different reasons. Let us have a look at them:
Causes of heavy periods (menorrhagia)
Several factors can contribute to menorrhagia. The common ones include:
- Hormonal imbalances, which may exist independently, or be caused by conditions like thyroid disorders, diabetes, obesity and polycystic ovary syndrome (PCOS).
- Ovarian dysfunction leading to an inadequate release of progesterone.
- Non-cancerous growths, such as fibroids or polyps in the uterus.
- Using an intrauterine device (IUD) in the womb for birth control.
- Complications in previous pregnancies (which may include placenta previa or a low-lying placenta), or miscarriage.
- Cancer of the uterus or cervix cancer.
- Bleeding disorders, which may increase the amount of bleeding e.g., haemophilia.
- Medications including those used in hormonal therapy, anticoagulants (clot-busting or clot-preventing) or anti-inflammatory medicines.
- Problems in the liver or kidneys.
Causes of light periods (hypmenorrhoea)
Several factors contribute to the condition. These are:
- Heredity plays a role since women can inherit this from their mothers.
- Women with low levels of body fat may experience hypomenorrhea. Women with anaemia and anorexia and those who diet and exercise heavily may also have hypomenorrhoea.
- Pregnant mothers may experience this in the first few months of pregnancy.
- Those suffering from high levels of stress, anxiety and physical strain may also have hypomenorrhea.
- When ovarian failure occurs before the age of 40, this condition may be one of the symptoms.
- Hormonal imbalances from thyroid disorders, diabetes, and altered androgen (sex hormones) levels may also contribute to the situation.
- Perimenopause or the period leading to menopause usually presents with scanty periods. (Read more: Early menopause)
- Prolonged use of birth control pills and devices, repeated abortions, diseases of the pelvis and anaemia can cause hypomenorrhoea.
- Problems like Sheehan’s syndrome (substantial loss of blood after childbirth that reduces the function of the pituitary gland) and Asherman’s syndrome (adhesions or bands of fibrous tissue inside the uterus) also contribute to hypomenorrhea.
- Hypomenorrhea can also result from PCOS.
Causes of infrequent periods (oligomenorrhoea)
There are a few common causes of oligomenorrhoea. These include:
- Engaging in intense sports and exercise,
- Eating disorders like bulimia and anorexia.
- Hormonal changes in adolescence and perimenopause.
- Hypothyroidism or reduced production of thyroid hormones.
- Diabetes.
- High levels of prolactin in the blood. (Read more: Prolactin test)
- Certain medications like antiepileptics (for treating epilepsy or seizures) and antipsychotics (to treat mental illnesses).
- Taking oral birth control pills. During the first few months of consumption, the period may reduce or stop altogether.
Causes of absent periods (amenorrhoea)
A variety of reasons can lead to amenorrhoea, such as
- Breastfeeding, menopause and pregnancy can cause amenorrhoea.
- Some women who are on oral contraceptive pills may miss their period entirely.
- Medications for cancer, high blood pressure, allergies or depression can also contribute to the condition.
- Excessive exercise, stress or low body weight can cause amenorrhoea.
- Hormonal problems including PCOS, premature menopause, tumours in the pituitary gland, or a thyroid disorder can also contribute to it.
- Genetic abnormalities leading to defects in the uterus or vagina, an underdeveloped reproductive system or scarring of the uterus may also cause amenorrhoea.
- Anatomical defects of the reproductive system.
See Similar Category Medicines Here
Symptoms of Irregular menstrual bleeding
The following are some of the symptoms of the various types of irregular periods:
Symptoms of menorrhagia
Any form of heavy bleeding does not qualify as menorrhagia. There are defined symptoms that typify this condition, including:
- Bleeding that continues for over a week.
- Very heavy flow, which requires changing sanitary napkins or tampons almost once an hour.
- Having to wake up in the middle of the night to change sanitary napkins.
- Passing blood clots larger than a small coin. (Read more: Blood clots during periods)
- Feeling of fatigue, breathlessness, and lack of energy.
- Being unable to perform daily activities due to the intensity of bleeding.
Symptoms of hypomenorrhoea
The primary symptoms of hypomenorrhea include:
- Very short periods (where the flow of blood is less than 80ml).
- A period that lasts two days or less.
- Spotting.
Symptoms of oligomenorrhoea
The most prominent symptoms of oligomenorrhoea include:
- Deviation of the period from its regular cycle and an extension beyond 35 days.
- In some cases when the period is pushed beyond 35 days, the subsequent period may arrive at an earlier date.
- The bleeding during the next period may also be heavy.
Symptoms of amenorrhoea
The most obvious manifestation of the condition is a missed period. Women who have missed three consecutive cycles or girls who have not gotten their period by the age of 15 can be suspected of having amenorrhoea. Other associated symptoms of the condition include:
- Pain in the pelvic region.
- Growth of excessive facial hair or hirsutism.
- Hair loss and acne.
- Headaches.
- Changes in vision.
- Discharge from the nipple.
Prevention of Irregular periods
The following are some ways to prevent irregular periods
Prevention of heavy periods
Menorrhagia caused due to medical complications need medical attention, however, it can be avoided in other cases by simply modifying your lifestyle. Ways to prevent it include:
- Adequate sleep.
- Exercise including walking, running or jogging, swimming or cycling. (Read more: Can I swim during my periods)
- Drinking enough fluids.
- Managing stress through meditation, yoga, and other relaxation techniques.
Prevention of light periods
While it may be difficult to prevent hypomenorrhoea caused due to medical conditions like PCOS, it can be avoided by following some good lifestyle habits. These include:
- Eat a healthy diet.
- Exercise regularly.
- Take an adequate amount of sleep. (Read more: Sleep chart by age and gender)
- Maintain a healthy weight for age and height.
- Manage stress well with yoga, meditation or pursuing hobbies. (Read more: Meditation for stress relief)
Prevention of infrequent periods
Oligomenorrhoea caused due to diseases like diabetes cannot be completely prevented. However, it can be avoided with certain lifestyle changes that directly impact health. Ways to prevent it are:
- Exercising regularly to stay fit and avoiding heavy or strenuous exercises.
- Managing stress with relaxation techniques.
- Having a regular sleep pattern.
- Maintaining a healthy weight. (Read more: What is BMI)
Prevention of absent periods
Amenorrhea may be avoided with certain lifestyle changes that may have a positive effect on reproductive health. These include:
- Keep your health in check and get yourself tested regularly to determine any hormone imbalances and other diseases.
- Indulge in yoga, meditation or pursue hobbies to cope with stress better.
- Get plenty of rest and sleep.
- Maintain a healthy weight for your age and height.
- Exercise regularly.
Diagnosis of Irregular menses
Diagnosis of irregular periods involves the following:
Diagnosis of heavy periods
To confirm a case of menorrhagia, specific diagnostic tests may be conducted:
- Blood test
To check for conditions including thyroid, anaemia, or problems with blood clotting. (Read more: Bleeding/clotting time test) - Pap test
PAP test involves the collection of a tissue sample from the cervix to detect any changes in the structure, which may point to an infection, swelling or cancer. - Biopsy
A biopsy of the uterus, called an endometrial biopsy, is carried out where tissue is sent for an examination to rule out cancer. - Ultrasound
Ultrasonography of the abdomen and pelvis to check for any abnormalities. - Hysteroscopy
In some cases where ultrasound may not prove conclusive, a thin camera attached to a tube (called hysteroscope) is inserted into the uterus to conduct the examination. - Sonohysterography
An injection of fluid into the uterus to examine its lining using an ultrasound.
Diagnosis of light periods
The main methods employed in the determination of hypomenorrhea are:
- Blood tests
These are done to evaluate levels of the luteinizing and follicle stimulating hormones (sex hormones); prolactin; and oestrogen. - Ultrasonography
To assess the thickness of the uterine lining, check for ovulation and the size of the ovaries, growth of follicles and any abnormalities. - MRI Scans
Sometimes MRI scans may also be advised for a better and detailed evaluation.
Diagnosis of infrequent periods
To diagnose oligomenorrhoea, the two most commonly used methods include:
- A review of the woman’s medical history.
- A physical examination along with ultrasounds and blood tests.
Diagnosis of absent periods
The first step towards the determination of amenorrhoea lies in:
- A complete general and pelvic examination to check the reproductive organs for any abnormalities.
- A series of blood tests follow to help rule out problems with the thyroid, ovarian function, prolactin, and androgens (male sex hormones, which are also present in some quantity in women).
- The doctor may prescribe hormonal medication to trigger menstrual bleeding. It helps to test oestrogen levels in the body.
- Scans like an MRI, ultrasound or a CT scan may also be advised to check for abnormalities and to rule out possibilities of a tumour.
Find best medical apps
Treatment of Irregular periods
Irregular periods can be treated in the following ways:
Treatment of heavy periods
The main courses of treatment for menorrhagia include medication and procedures. These are:
- Medication
Different kinds of medicine may be prescribed depending on the nature of symptoms and also severity. - Anti-inflammatory drugs
These are advised since they not only help reduce blood loss but also help in relieving pain from menstrual cramps. - Oral contraceptives
Oral contraceptives are commonly prescribed to help regulate the menstrual cycle, reduce excessive bleeding and also decrease the duration of the period. - Iron supplements
In cases where iron levels are low or the woman is anaemic. - Progesterone
This is the hormone primarily responsible for hormonal imbalance, prescription of oral progesterone helps restore balance and treat menorrhagia. - Tranexamic Acid
This drug helps lower blood loss during the menstrual flow and is usually prescribed to be taken only during the phase where bleeding occurs.
Procedures
If medication is suggested but hasn’t shown any marked improvement, the gynaecologist may indicate a medical procedure to help address menorrhagia. It may include any one of the following procedures:
- Hormonal intrauterine devices
These devices, when placed in the uterus slowly release the hormone progestin, which helps thin the uterine lining, thereby reducing blood flow and minimizing cramping. - D&C
D&C or Dilation and curettage is the most frequently suggested procedure. In this procedure, The cervix is dilated, and the endometrial lining of the uterus is then scraped clean to reduce bleeding. While this is extremely effective, it may need to be repeated in case menorrhagia recurs. - Focused Ultrasound Surgery
This is a procedure targeted at shrinking the size of fibroids present in the uterus. Ultrasound surgery is a non-invasive procedure, which uses ultrasound waves to help destroy or reduce the size of fibroids. - Uterine embolization
It targets uterine fibroids to shrink their size. A catheter is passed through the thigh into the arteries to reach the uterus, certain drugs are injected, which cut off the flow of blood to the fibroids thereby shrinking their size. - Myomectomy
The number and size of fibroids may determine whether the surgeon suggests myomectomy, the surgical removal of fibroids. This procedure may be performed through laparoscopy (by making incisions in the abdominal skin) or by passing the hysteroscope in the cervix and vagina. - Endometrial procedures
These can be of 2 kinds – endometrial ablation, which is the destruction of the uterine lining using a laser. Endometrial resection uses a surgical loop to remove the uterine lining. While both methods may prove effective, pregnancy may not be possible following them. - Hysterectomy
Removal of the uterus surgically is perhaps the least opted course to treat menorrhagia and usually suggested only in cases of cancers.
Treatment of light periods
Hypomenorrhea can be harder to cure when it is in pubescents or menopausal women. Understanding the cause is the key to finding the right course of treatment for this condition.
- Medication can be prescribed in cases where the problem stems due to hormonal imbalance, or when the woman suffers from hypothyroidism.
- Procedures, which can help treat scar tissue, fibroids, issues in the reproductive tract or polyps can also be helpful in treating hypomenorrhea.
- Modifications made to the lifestyle are also known to be beneficial. The changes include rest and sleep, exercise and healthier food options like green leafy vegetables, red meats, and dry fruits.
Treatment of infrequent periods
Treating oligomenorrhoea involves:
- Making some lifestyle changes such as better diet, incorporating more rest.
- Cutting on heavy exercise.
- Adjusting the period by progestin or birth control medication.
Treatment of absent periods
Treatment may follow a dual approach and include:
- Medical treatment
Medication may be administered for hormonal imbalances, or to treat problems with other hormone-producing glands such as thyroid, pituitary, ovaries, and more. The doctor may also prescribe oral contraceptive pills to help restore hormonal balance. In cases where there are tumours, surgery may be necessary. - Lifestyle modification
Rest, recreation, regular moderate exercise, and a balanced diet can also help relax the body and bring in regularity in the period.
References
- Center for Disease Control and Prevention [internet], Atlanta (GA): US Department of Health and Human Services; Heavy Menstrual Bleeding
- T. Kröncke and M. David. Magnetic Resonance Guided Focused Ultrasound# for Fibroid Treatment – Results of the Second Radiological Gynecological Expert Meeting. Geburtshilfe Frauenheilkd. 2015 May; 75(5): 436–438. PMID: 26097245
- Eunice Kennedy Shriver National Institute of Child Health and Human; National Health Service [Internet]. UK; What causes menstrual irregularities?
- Eunice Kennedy Shriver National Institute of Child Health and Human; National Health Service [Internet]. UK; What are the common treatments for menstrual irregularities?
- Klein DA, et al. Amenorrhea: An approach to diagnosis and management. American Family Physician. 2013;87:781.
- Rebar R. Evaluation of Amenorrhea, Anovulation, and Abnormal Bleeding. [Updated 2018 Jan 15]. In: Feingold KR, Anawalt B, Boyce A, et al., editors. Endotext [Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000-.