Summary
Knee replacement surgery can provide relief to people with severe knee pain who do not get relief from any other treatment. Knee replacement may be total or partial depending on the severity of the condition. During the surgery, the affected part will be replaced with a prosthetic (artificial body part). The surgery will require general or spinal anaesthesia.
Before the surgery, some tests and a dental check-up will be required to see if you are fit for the surgery. After the surgery, an exercise and physiotherapy plan will be made, designed to get you back to your routine. A knee replacement surgery helps in alleviating knee pain to a great extent and improves the quality of life; however, in some cases, complications may occur.
- What is knee replacement surgery?
- Why is a knee replacement surgery done?
- Who can and cannot get the knee replacement surgery?
- What preparations are needed before the knee replacement surgery?
- How is the knee replacement surgery done?
- How to care for yourself after the knee replacement surgery?
- What are the possible complications/risks of knee replacement surgery?
- Follow-up with your doctor after knee replacement surgery
What is knee replacement surgery?
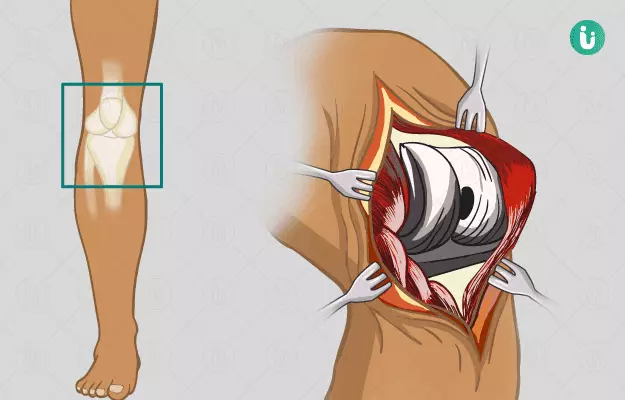
Knee replacement surgery is an operative procedure performed on people with severe knee damage that could not be treated with other treatment methods. For example, knee damage caused due to advanced knee arthritis. In advanced knee arthritis, wear and tear of the knee cartilage causes the surface of the knee to become pitted, uneven and eroded. This leads to instability, stiffness, and pain in knee and a change in the alignment of the body.
This surgery may also be advised to individuals who have a weakened knee joint due to an injury or other condition. The surgery can help them lead a more active life.
The knee has three compartments- inner (medial), outer (lateral) and kneecap. Depending on how much of the knee joint is being replaced, there are two types of knee replacement:
- Total knee arthroplasty (replacement) procedure: In this procedure, surgeons replace the damaged bone and cartilage from the knee joint with an artificial surface made from metal and plastic. All the three parts of the knee joint are replaced in this one.
- Partial knee arthroplasty: Only one part of the knee joint is replaced. This surgery is usually needed to replace the inner side of the knee joint.
Why is a knee replacement surgery done?
Your doctor may recommend a knee replacement surgery in the following cases:
- The severity of the pain from knee arthritis does not allow you to sleep well or perform your regular activities -
- You are unable to walk or care for yourself.
- You are unable to go out socially or work.
- You are feeling depressed due to lack of mobility and pain.
- Other treatments are not able to alleviate your knee pain.
Who can and cannot get the knee replacement surgery?
People with the following conditions can get the surgery:
- Arthritis: In this condition, the cartilage that forms the surface of the knee joint is worn out due to ageing or disease. So every time you move, your bones rub on each other, causing pain and further roughness of the joint surface.
- Injuries: These may be sports-related or due to trauma or accident.
- Osteonecrosis in the thigh bone: In this condition, the blood supply to the thigh bone is reduced, leading to bone death. This may cause the bone to break due to weight-bearing activities, resulting in a painful joint.
Knee replacement surgery may not be advisable in individuals with the following conditions:
What preparations are needed before the knee replacement surgery?
Before the surgery, your doctor will ask you to sign a consent form allowing them to perform the procedure. He/she will explain to you the procedure and resolve all your doubts and queries. You may have to fast for 8 hours before the surgery, usually postmidnight.
Your doctor will carry out a physical exam to ensure overall health. Along with this, you may need blood tests and diagnostic tests such as the following:
- Blood tests to check for anaemia and the proper functioning of the kidneys.
- Urine test to check for infections.
- An MRSA (methicillin-resistant Staphylococcus aureus bacteria) swab (cotton bud) test of the nasal, armpit and groin areas to check for bacteria resistant to certain medicines.
- An electrocardiogram (that records the electrical activity of the heart) to ensure your heart is healthy.
Your blood sugar levels (especially if you have diabetes) and blood pressure would also be monitored. You should also get a dental check-up to diminish the risk of acquiring an infection due to the bacteria getting into your blood from a dental infection.
Inform the doctor about any of the following:
- Allergy to any drugs, tape, latex, and anaesthetic medicines (medicines used to produce a temporary loss of sensation).
- All the medications you are currently taking, including prescription and non-prescription medicines and herbal supplements.
- If you are pregnant or suspect that you are pregnant.
- History of bleeding disorders or, if you are consuming any anticoagulants, (blood-thinning medicines), aspirin or any other medicines that affect the blood clotting process.
You may need to discontinue some of the above medicines before your surgery.
The orthopaedic surgeon will advise some exercises to strengthen your thigh muscles as your recovery will go faster if your muscles are strong. Along with this, you may need to see a physiotherapist or occupational therapist who will explain to you the exercises that need to be done after the surgery and any special equipment, such as cane, crutches, walker or wheelchair that may help you function well at home.
How is the knee replacement surgery done?
Just before the procedure, you may be administered a sedative to help you relax. You will meet the surgeon and anaesthetist to discuss any additional doubts about the procedure.
After that, you will be administered either general anaesthesia which will keep you unconscious during the surgery or epidural or spinal anaesthesia in which you will be conscious but will not feel anything below the waist. The anaesthesia may be administered in the operation theatre or while you wait to be transferred into the operation theatre.
During the surgery, a doctor will replace the worn-out part with a prosthesis, which is a made-to-measure part of plastic or metal. This may be either a partial or total knee replacement depending upon the extent of knee damage.
The total knee replacement surgery takes about 1 to 3 hours, and both sides of the knee are replaced. The procedure is as follows:
- The surgeon will make an incision (cut) on your affected knee to expose the knee joint.
- They will remove the damaged parts, and appropriately measure and shape the ends so that the prosthetic fits.
- This will be tried by fitting a dummy joint to check the working of the joint, and then the final prosthetic is attached.
- The end of the thigh bone will be replaced with a curved metal prosthetic, and a flat metal plate will replace the end of shin bone.
- A special bone “cement” can be used to fix these to the bone or they can be treated with a coating to encourage the bone to fuse with the replaced parts.
- To reduce the friction, the surgeon will place a plastic spacer between the pieces of metal to act as cartilage.
- If required, the back of the kneecap may also be replaced.
- Once the procedure is done, the doctor will seal the wound using staples or stitches, and a dressing is done.
- Only in rare cases, a splint (a rigid or flexible material to protect an injured part) may be placed, but generally, movement of the knee is encouraged as early as possible.
A partial knee replacement is generally performed in about a quarter of the people with osteoarthritis. The surgery can be performed by a minimally invasive or reduced invasive technique. This is a relatively simple surgery in which a smaller incision is required and less bone is removed. The recovery period and hospital stay are also shorter with a partial knee replacement. Knee movement after a partial knee replacement is more natural, and you can lead a more active lifestyle compared to that after a total knee replacement. A blood transfusion is rarely required with this surgery.
You may experience some difficulty in bending and kneeling after a knee replacement surgery.
Immediately after the surgery, you will be taken to the recovery room and your vital signs (breathing, blood pressure and pulse) will be monitored. If required, you may be given oxygen through a tube or a mask. You may also be given a blood transfusion if needed. After you are alert and your vital signs are stable, you will be taken to your room (in the hospital) where you will have to stay for a few days.
Your knee will be covered in a dressing to protect the wound. A tube will be attached at the site of surgery to drain the blood and prevent it from collecting in the wound. Until the wound is healed, the dressing will be routinely changed. You will also have to take pain medications regularly.
How to care for yourself after the knee replacement surgery?
During the recovery period, you will meet a physiotherapist to plan the appropriate exercise rehabilitation programme, which will begin in the hospital and continue after your discharge until you have regained muscle strength and a wide range of motion. You may be discharged to home or to a rehabilitation centre.
At home, you will need to maintain hygiene at the surgical site and follow the specific instructions for bathing as follows:
-
Having a bath: Wait for 24 hours before taking a shower. Keep these tips in mind before taking a bath:
- Take a shower instead of a bath as soaking the wound may cause the scar tissue to open up. Only take a bath if you can keep the wound dry.
- Do not use any soap, body lotion, talcum powder or any bathing products on the wound as they can cause discomfort and increase the risk of infections.
- You can keep the dressing on if it is waterproof but may need to remove it if it is not. Ask the healthcare provider for the type of dressing you have on.
- If you splash some water on the wound, do not panic.
- Do not rub on the wound as it can delay healing and be painful.
- Pat the wound dry with a clean, dry towel after your bath or shower.
- Changing the dressing: The dressing can be left on for two days or as advised by the doctor unless there is oozing at the surgical site. Keep the dressing dry for two days. However, if the dressing gets wet due to any liquid, including blood, it needs to be changed. Before changing the dressing, keep the following tips in mind:
- Clean your hands properly with soap and water.
- Take the old dressing off without touching the used side.
- Avoid touching the wound with your fingers.
- Do not touch the clean side of the new dressing to prevent contamination
- Do not apply any antiseptic cream under the dressing
At the 2-week follow-up clinic visit, the stitches or staples on your wound will be removed. You should continue taking pain medication as advised by the doctor. Make sure that you take only those medicines advised by your doctor to prevent the risk of bleeding.
You do not need to follow any dietary restrictions unless specifically advised by the doctor. Start driving when the doctor permits you to do so. The restriction may also apply to other activities such as sitting, kneeling, and going up and down the stairs.
You can make the following changes to your home to help speed up your recovery:
- Attach handrails in the bathroom, shower and all staircases
- Raise the height of the toilet seat
- Use a chair while showering
- Sit on a stable chair with arm support that has a firm back and seat cushion, that allows the knees to be positioned at a level that is lower than the hips
- Use a shower hose and a shower sponge with a long handle
- Use a reaching stick to grab things
- Use firm pillows to raise the level of hips above the knees when sitting
- Remove loose objects, like carpets and electrical cords that may cause you to fall
The benefits of a knee replacement surgery are as follows:
- Knee replacement surgery can relieve persistent knee pain
- Most people do not need any help in walking once they recover
- Most artificial knee joints last for 10 to 15 years, and some may last up to 20 years before they need to be replaced.
When to see the doctor
Inform your doctor if you experience any of the following:
What are the possible complications/risks of knee replacement surgery?
The presence of complications decreases the outcome of the surgery and the satisfaction of the person undergoing the replacement. It is reported that about 20% of the people who undergo a knee replacement surgery are not satisfied with the results. The possible complications include:
- Peroneal nerve palsy (paralysis of the peroneal nerve - a nerve in the lower leg)
- Patellar clunk syndrome (nodule formation near the knee cap causing catching or popping when the knee is extended)
- Loosening of the prosthetic parts
- Stiffness of the knee
- Infection of the joint replacement, needing further surgery
- Unexpected bleeding into the knee joint
- Bone fracture around the replaced knee
- Blood clots in the deep veins of the leg
- Pulmonary embolism (artery in the lungs gets blocked by blood clots)
- Nerve and other tissue (like arteries and ligaments) damage during surgery
- Pain in the knee
- Dislocation of the knee
Follow-up with your doctor after knee replacement surgery
Your doctor may give you a follow-up appointment at 2-week after the surgery when the stitches or staples on your wound will be removed.
The next appointment would be at about 6 to 12 weeks after the surgery to check your progress. An x-ray of the knee may be performed at the follow-up appointment.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Surgery Cost In Your City
Doctors for Knee Replacement Surgery

Dr. Vatsal Khetan
Orthopedics
9 Years of Experience

Dr. Prince Uchadiya
Orthopedics
7 Years of Experience

Dr. Manoj Kumar S
Orthopedics
8 Years of Experience
Dr. Ankur Saurav
Orthopedics
20 Years of Experience
References
- MedlinePlus Medical Encyclopedia [Internet]. US National Library of Medicine. Bethesda. Maryland. USA; Knee Replacement
- Hospital for Special Surgery [internet]. New York. US; Knee Replacement
- American Academy of Orthopaedic Surgeons [Internet]. Illinois. US; Treatment of osteoarthritis of the knee: evidence-based guideline 2nd edition
- Mihalko WM. Campbell's Operative Orthopaedics. 13th ed. Philadelphia: Elsevier; 2017. Chapter 7, Arthroplasty of the knee.
- Feng JE, Novikov D, Anoushiravani AA, Schwarzkopf R. Total knee arthroplasty: improving outcomes with a multidisciplinary approach. J Multidiscip Healthc. 2018 Jan 25;11:63-73. PMID: 29416347.
- National Health Service [internet]. UK; Knee replacement
- Cedars Sinai [Internet]: Cedars Sinai Medical Center. Los Angeles. US; Knee Replacement Surgery
- Versus arthritis [Internet]. Chesterfield. UK; Knee replacement surgery
- Johns Hopkins Medicine [Internet]. The Johns Hopkins University, The Johns Hopkins Hospital, and Johns Hopkins Health System. US; Arthroplasty
- Sankar B, et al. The role of MRSA screening in joint-replacement surgery. Int Orthop. 2005 Jun;29(3):160-163. PMID: 15864590.
- Oxford University Hospitals [internet]: NHS Foundation Trust. National Health Service. U.K.; Caring for surgical wounds at home
- Patient education: Bone and joint center [Internet]. University of Washington Medical Center. US; After Total Knee replacement: caring for your knee at home.
- Varacallo M, Luo TD, Johanson NA. Total Knee Arthroplasty (TKA) Techniques. [Updated 2020 Feb 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan
- Smith LK, et al. Empirical support for radiographic review: a follow-up study of total hip arthroplasty. Hip Int 2013;23(01):80–86.