The cases of COVID-19 have increased tremendously since it was first found in Wuhan, China late last year. As it is a new disease, doctors have been trying to understand the SARS-CoV-2 virus and find out a cure for those infected by it.
Doctors have seen that people with pre-existing medical conditions like High blood pressure (Hypertension), Diabetes, Heart disease, Chronic Kidney disease, Lung Disease and Cancer are at a high risk of developing severe symptoms of COVID-19 infections. These patients are the ones who develop complications in the later stages of their infection.
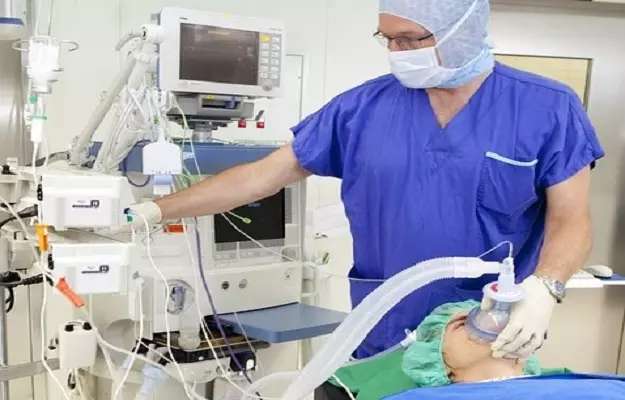
The most common complication seen in these patients is related to the respiratory system which includes extreme difficulty in breathing, viral pneumonia and pulmonary embolism. Apart from the respiratory complications, various other complications were seen in critically ill patients of COVID-19 infection.
Here in this article, we will tell you about the various complications that are seen in patients with COVID-19 infection.
- Cardiac injury
- Coagulopathy
- Septic shock
- Encephalopathy
- Liver injury
- Immune Thrombocytopenic Purpura
- Deep vein thrombosis
- Rhabdomyolysis
Cardiac injury
People with a pre-existing heart conditions are already said to be at risk of developing severe symptoms of the COVID-19 infection. However, doctors have also seen that in heart patients, the respiratory infections due to COVID-19 increase the workload of the heart which was already working overtime. This means that the heart is not getting the extra oxygen it requires.
Earlier it was concluded that the Middle East respiratory syndrome (MERS) can cause acute myocarditis and heart failure. Similarly, myocardial damage (damage to the muscle of the heart) was also seen in COVID-19 patients. According to a Chinese study, 5 out of the first 41 COVID-19 infected patients had suspected myocardial injuries. After testing, the levels of cardiac troponin I was found increased in their blood, which is otherwise only seen after any cardiac injury.
Coagulopathy
Coagulopathy is a condition where blood loses its ability to clot. Critically ill patients with COVID-19 infection have been reported to develop coagulopathy later in the hospital stay. Coagulopathy was also reported in patients with sepsis.
In a Chinese study by Tang et al, it was concluded that 71% of the non-survivors from COVID-19 infection met the ISTH (International Society of Thrombosis and Haemostasis) criteria which measures the internal bleeding. It was noticed that these patients had elevated D-dimer levels at admission. Increased D-dimer levels indicate an increased risk in abnormal blood clotting which can be seen during acute pulmonary embolism. Increased D-dimer levels were seen to be associated with high mortality, cytokine storm and organ failure.
The most common pattern of coagulopathy observed in patients hospitalised with COVID-19 is characterized by elevations in fibrinogen and D-dimer levels.
Septic shock
An article, published in the journal Lancet on 11 March 2020, was based on a small study from China. The study stated that half the patients who had the worst outcomes from the COVID-19 infection were those who had developed sepsis. The doctors confirmed that sepsis was one of the common complications that were seen in critical patients of COVID-19.
Sepsis is a life-threatening reaction of the body towards the infection that tries to invade different organs. A patient with sepsis would present with fever, weakness, a rapid heart rate, a rapid breathing rate, and an increase in the number of white blood cells. Sepsis damages various internal organs such as the kidneys, heart and lungs, and causes them to fail. When the blood pressure goes too low due to the sepsis, that condition is known as septic shock.
Another study published on 20 March 2020 concluded that patients who were critically ill and those who had died had severe infections such as viral pneumonia, Acute respiratory distress syndrome (ARDS), sepsis and septic shock.
Encephalopathy
Neurological complications in COVID-19 infected patients have not been widely reported. Encephalopathy is a rare complication of a viral disease and has just been reported in a handful of people infected with the COVID-19 infection. Encephalopathy is the disease of the brain that alters brain function or structure.
One of the cases was that of a 74-year-old man who had a history of atrial fibrillation, cardiac stroke, Parkinson’s disease, chronic obstructive pulmonary disease (COPD) and recent cellulitis. After being admitted to the hospital once due to fever and cough, he was sent home with a prescription of oral antibiotics. But his symptoms worsened and he presented with an altered mental status and severe headache. On testing his nasopharyngeal swab, the doctors found him to be COVID-19 positive. On getting his head CT scan, the doctors found that the person had encephalopathy. Due to his severely critical condition, the man was admitted to the ICU.
Another case was of a female airline worker who presented with a 3-day history of cough, fever, and altered mental status. On testing her nasopharyngeal swab specimen, she was found COVID-19 positive and on taking her head CT the doctors found that the woman had areas of a brain haemorrhage. The doctors diagnosed her for acute hemorrhagic necrotizing encephalopathy, which is a deadly brain condition where the brain tissue starts decomposing on its own.
Liver injury
Liver injury has been seen in a few patients of COVID-19, however, the cause of the infection has not been clear so far. Some doctors believe that liver impairment could be due to drug hepatotoxicity (injury to the liver due to exposure to drugs).
Some doctors believe that immune-mediated inflammation, such as cytokine storm (storm of inflammatory cells in the body) and pneumonia-associated hypoxia (lack of oxygen in the body due to pneumonia), might also contribute to liver injury and sometimes can be a reason for liver failure in patients with COVID-19 who are critically ill.
Immune Thrombocytopenic Purpura
A case published in the New England Journal of Medicine stated that a woman with hypertension and hypothyroidism, who was confirmed with COVID-19 infection, started presenting with a nasal bleed and dark purple-bluish spots (purpuric spots) in the lower extremities on the fourth day of treatment. On testing her blood, it was found that her platelet count was extremely low. The doctors concluded that the woman was suffering from immune thrombocytopenic purpura.
Immune Thrombocytopenic Purpura is a bleeding disorder where the blood doesn't clot due to a low number of platelets or thrombocytes. Platelets are formed in the bone marrow of the body. They stop the bleeding by making clots over small cuts or breaks that happen on the blood vessel walls.
Deep vein thrombosis
Deep vein thrombosis (DVT) is a serious condition where a blood clot gets lodged in a vein inside the body. These clots are usually seen in the thigh or lower leg, but they can also develop in other areas of your body.
Severely ill patients of COVID-19 infection need intensive care such as ventilators and are needed to be admitted in the Intensive Care Units (ICU). Prolonged mechanical ventilation, the insertion of central venous catheters, the inability of the patients to move and the presence of other comorbidities including obesity can lead to the occurrence of a deep venous thrombosis (DVT) in patients of COVID-19 infection admitted at ICU. The incidence of DVT during ICU stay has been reported in many critically ill patients of COVID-19 infection.
Rhabdomyolysis
Rhabdomyolysis is a life-threatening medical condition involving the rapid destruction of damaged or injured skeletal muscles of the body. A few cases of rhabdomyolysis have been reported in the patients of COVID-19 infection in Wuhan, China. Several hypotheses have been given to explain the reason behind the occurrence of this condition in COVID-19 patients:
- Some scientists believe that rhabdomyolysis is initiated due to the virus that enters the body.
- Some believe that as the virus enters the body, our immune system gets activated resulting in a cytokine storm (storm of inflammatory cells in the body) which damages muscle tissues.
- Some scientists believe that the circulating viral toxins in the body may have directly destroyed the muscle cell membranes.
It does not present immediately, but if caught in early stages, rhabdomyolysis can be treated and prevented easily.
Medicines / Products that contain Complications of severe COVID-19 infection
- Proctosedyl BD Cream - ₹118
- Anovate Ointment - ₹117
- Covifor Injection - ₹3780
- Fabiflu 400 Tablet - ₹856
- Fabiflu 200 Mg Tablet - ₹1292
- Fabiflu (Favipiravir) 200 Mg Tablet - ₹1292
- Fabiflu (Favipiravir) 400 Mg Tablet - ₹1224
- Pilo GO Cream - ₹75
- Anovate Cream - ₹111
- Remdesivir Injection - ₹10500
- Molusafe Capsule - ₹457
- Movfor 200 Mg Capsule - ₹2490
- Molflu 200 Mg Capsule - ₹1400
- Molulife 200 Capsule - ₹1399
- Cipmolnu 200 Mg Capsule - ₹2000
- Molxvir 200 Mg Capsule - ₹1520
- Alzumab Injection - ₹8229
- Immunocin Alpha Plus 1.6mg Injection - ₹5998
- Imualfa 1.6mg Injection 1ml - ₹2628
- Molnutor 200 Mg Capsule - ₹2000