Summary
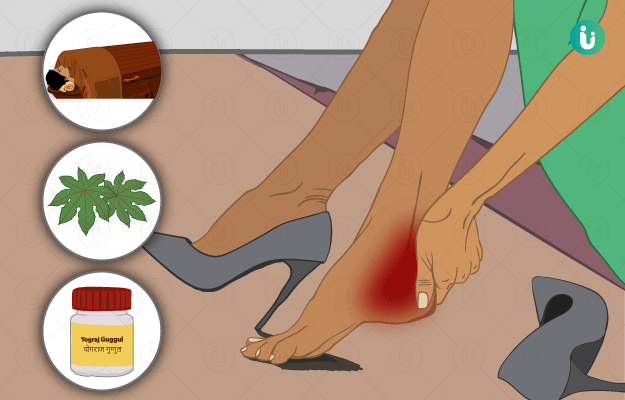
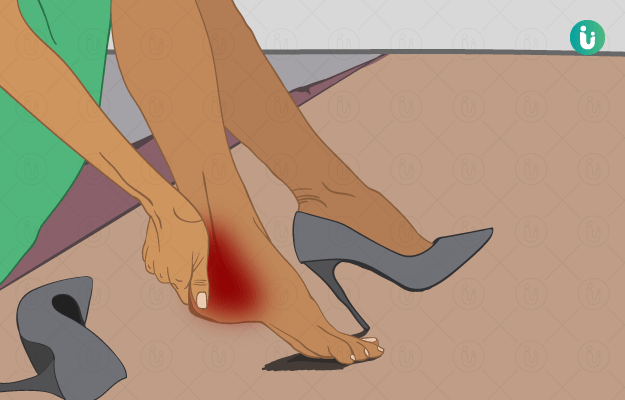
The foot and ankle are made up of 26 bones, forming 33 joints and are attached to each other with over 100 tendons. The heel or the calcaneum is the largest bone of the foot. Overuse or injury of the heel can lead to pain, which can significantly reduce movement, ranging from mild restriction to complete disability. Sometimes heel pain can be treated with self-care measures, whereas others require surgical management.

 Doctors for Heel Pain
Doctors for Heel Pain  OTC Medicines for Heel Pain
OTC Medicines for Heel Pain
 Heel Pain articles
Heel Pain articles
 Ayurvedic Treatment of Heel Pain
Ayurvedic Treatment of Heel Pain
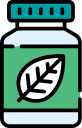
 Home Remedies for Heel Pain
Home Remedies for Heel Pain
 Homeopathic Treatment of Heel Pain
Homeopathic Treatment of Heel Pain



































 Dr. Laxmidutta Shukla
Dr. Laxmidutta Shukla
 Dr. Rachita Narsaria
Dr. Rachita Narsaria