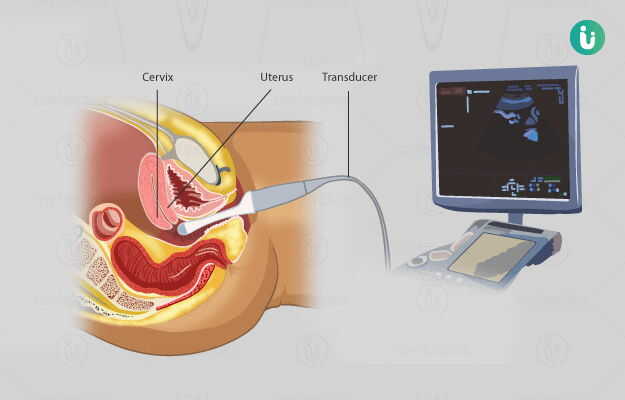
Hysteroscopy is a minimally-invasive surgical procedure used to internally visualise the cervix and the uterus (womb).
The procedure is done using a hysteroscope, which is inserted through the vagina and progressed up to the uterus. The procedure is used to assess and sometimes treat cervix and/or uterus related symptoms.
Prior investigations include blood tests and radiological tests. The procedure is often a daycare admission (the person is admitted in the morning and discharged by the evening).
Post-procedure, the aftercare is uneventful and the person can resume normal activities by end of the day.
- What is hysteroscopy?
- Indications for hysteroscopy
- Contraindications for hysteroscopy
- Preparations before the procedure
- What happens during the procedure
- Risks and outcomes of the surgery
- Aftercare, discharge and follow up
- Takeaway
What is hysteroscopy?
The cervix and uterus are part of the internal genitalia of the female reproductive system. The cervix is the lower part of the uterus and serves as the entrance into the uterus. The uterus or womb is a hollow organ that is made of three layers: outer, middle (myometrium) and inner (endometrium). Abnormalities can be present or can occur in these structures.
Hysteroscopy is a procedure that is employed to visualise the internal structure of the cervix and uterus so that such abnormalities can be detected.
It is done using a thin, flexible, telescope-like tube with a light and a camera attached to it which is inserted via the vagina. Hence, no cuts are made on the body during the insertion of the hysteroscope. The images collected from the camera are transmitted to a monitor and are then analysed by the doctor. The procedure uses a special gas or fluid to dilate the uterus for better visualisation.
Hysteroscopy is of two types based on the requirement. They are:
- Investigative and/or Diagnostic hysteroscopy: it is used to help investigate and diagnose uterine abnormalities based on the symptoms of the patient
- Interventional / Operative hysteroscopy: it is considered a step further in treating the cause of the symptoms of the patients.
Indications for hysteroscopy
Indications for hysteroscopy include abnormal symptoms of the patient, interventional reasons or abnormal results of pathological tests. They can be categorised as:
- Investigative indications:
- Heavy bleeding during periods (menorrhagia)
- Unusual vaginal bleeding
- Abnormal pap smear test results
- Bleeding after menopause
- Pelvic pain
- Inability to conceive or repeated miscarriages
- Diagnostic indications:
- Interventional indications:
- Removing fibroid or polyps
- Remove displaced Intra-Uterine Contraceptive Devices (IUCDs)
- Place small birth control devices into the fallopian tubes
- Remove excess endometrial tissue
- Remove adhesions (scar tissue) that can contribute to issues in menstruation, conceiving or maintaining pregnancy
Contraindications for hysteroscopy
The absolute contraindication for hysteroscopy is pregnancy, hence, it is to be ruled out beforehand. Relative contraindications can involve:
- Any pre-existing conditions, which can increase risks associated with anaesthesia
- Infections of the cervix or uterus
- Cancer of the cervix or cancer of the uterus
Preparations before the procedure
The procedure is done by a gynaecologist (OBG surgeon). The doctor explains the procedure to the patient along with the outcome and associated risks. A detailed history of the patient is taken which includes the symptoms of the patient, history of any pre-existing conditions (comorbidities), menstrual history (which may also include a history of pregnancy and miscarriage, if any), family history, medication history. A local physical examination is done which may include taking a Pap Smear (collecting secretions from the cervix).
Investigations to be done before the procedure include:
- Routine blood tests
- Routine urine investigations
- Urine pregnancy test (UPT): since pregnancy is a contraindication for the procedure
- Ultrasound of the abdomen and ultrasound of the pelvis: to rule out ectopic pregnancy (site of pregnancy is other than the uterus)
- Certain blood tests can be done to help narrow down the cause of infertility
- In some cases, CT or MRI of the pelvis may be required
Medications for any pre-existing conditions taken by the patient may be stopped or altered as per the doctor’s orders.
The patient may be advised to arrange a ride back home beforehand because of the after-effects of anaesthesia. The procedure is usually a daycare admission. The patient is told to fast overnight before the procedure.
On the day of the procedure, the patient arrives at the hospital with all the relevant documents and reports and gets admitted. The patient changes into the hospital attire. Pubic hair, if present, is shaved off. The doctor explains the procedure again with the associated risks and written consent is taken from the patient. A final review of the patient is done by the doctor and nurses before the patient is shifted to the operation theatre (OT).
What happens during the procedure
The patient is made to lie in the lithotomy position (position where the patient is lying on their back and the legs of the patient are spread wide when giving birth). A monitor is attached to keep track of the vitals (heart rate, blood pressure and oxygen saturation) of the patient. An IV cannula is inserted through which medications for the procedure are administered. A urinary catheter is inserted to prevent contamination of the procedure. The genital area is cleaned and covered with sterile drapes. The procedure can be done under general or regional anaesthesia (the lower half of the body is made numb).
The surgeon then opens the vagina using an instrument called the speculum and then, the hysteroscope (a thin, flexible tube with a light and camera) is inserted. A gas (carbon dioxide) or fluid is inserted from the hysteroscope to dilate the uterus to help in easier visualisation of the internal anatomy. The amount of gas or fluid inserted is carefully monitored. The fluid/gas is chemically inert and usually does not cause any irritation.
The doctor then visualises the uterus using the camera of the hysteroscope and takes pictures of the uterus. Based on the indication of the procedure, additional interventions can be done such as:
- Sample of the endometrium may be taken (endometrial biopsy)
- The excess endometrial lining may be scraped off
- Misplaced IUCDs can be retrieved
- New contraceptive devices can be inserted into the fallopian tubes
- Any adhesions (scar tissue) can be removed
- Polyps or fibroids can be excised using special instruments
After the procedure is done, the doctor withdraws the hysteroscope and the urinary catheter is removed. The vaginal opening is packed with gauze to stop any bleeding associated with the procedure. The entire procedure is usually completed within 30 minutes. However, the duration may extend if any additional interventions are performed.
Risks and outcomes of the surgery
The risks associated with the procedure are minimal. However, some complications may arise, such as:
- Excessive bleeding
- Localised infection
- Damage to the uterus or cervix, such as perforation
- Damage to the surrounding structures such as intestine, bladder, ovaries
- Pelvic inflammatory disease (diffused inflammation of the genital tract due to infection)
- Complications related to anaesthesia
- Complications related to the gas or fluid injected
- Formation of adhesions or scarring of the endometrium
Aftercare, discharge and follow up
After the procedure, the patient is shifted from the OT to an observation room for a few hours. In some cases, the patient may be kept in the hospital for overnight monitoring. Normal passing of urine indicates the wearing-off of anaesthesia. The patient may feel cramping pain (similar to the pain during periods) which is managed by analgesics.
A discharge summary is prepared by the doctor which contains relevant medications and advice on wound care. These typically include:
- Continuation of medication for pre-existing conditions, if any
- Antibiotics to prevent infection
- Oral medication to minimise bleeding may be prescribed (Tranexamic Acid tablets)
- The patient may feel abdominal discomfort (bloating) due to the gas/fluid injected during the procedure. However, this subsides within 24 hours.
- Wear sanitary pads for a few days since minimal bleeding or spotting may be present
- Pain similar to cramps during menstruation may persist for a few days which are managed by analgesics
- Proper hygiene is to be maintained around the area to prevent infection
- Abstain from strenuous and sexual activities for one to two weeks after bleeding has subsided
The recovery period is usually uneventful. The patient may be able to resume normal activities and return to work within 24 hours. The patient should notify the doctor if any of the following symptoms arise:
- Excessive bleeding
- Excessive discharge from the vagina, which may be foul-smelling or is purulent (has pus), indicating infection
- Excessive prolonged pain not relieved by analgesics
- Fever
The follow-up of the patient is as per the outcome of the procedure and doctor’s orders.
Takeaway
Hysteroscopy is a modern, minimally-invasive surgical procedure used to visualise the internal structures of the cervix and uterus. It is used for investigative and diagnostic purposes. In addition, it can be coupled with additional interventional procedures to treat numerous pathologies and abnormalities of the uterus and cervix. Pregnancy is an absolute contraindication of the procedure. The procedure itself is of short duration and has minimal risk. Recovery post-procedure is fast and the patient can resume normal activities within 24 hours.
Find Obstetrician and Gynaecologist in cities
- Obstetrician and Gynaecologist in Bangalore
- Obstetrician and Gynaecologist in Mumbai
- Obstetrician and Gynaecologist in Ghaziabad
- Obstetrician and Gynaecologist in Chennai
- Obstetrician and Gynaecologist in Pune
- Obstetrician and Gynaecologist in Delhi
- Obstetrician and Gynaecologist in Hyderabad
- Obstetrician and Gynaecologist in New Delhi
- Obstetrician and Gynaecologist in Gwalior
- Obstetrician and Gynaecologist in Gurgaon
Surgery Cost In Your City
Doctors for Hysteroscopy

Dr. Shravani A
Obstetrics & Gynaecology
3 Years of Experience

Dr Minoo Singh
Obstetrics & Gynaecology
44 Years of Experience

Dr. Godi Anuradha
Obstetrics & Gynaecology
31 Years of Experience