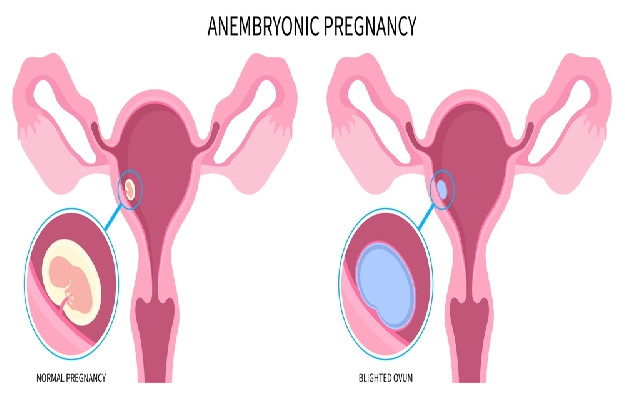
Getting a positive pregnancy test result brings tremendous joy to couples who are trying for a baby. However, losing the pregnancy in the first 20 weeks - known as a miscarriage - can be equally hard on couples. Up to 15% of pregnancies end in a miscarriage and eight out of 10 miscarriages occur in the first trimester of pregnancy, from weeks zero to 13.
Distressing as a miscarriage can be, one to two out of 100 women also run the risk of having recurrent miscarriages. Having two or more consecutive miscarriages prior to 20 weeks of pregnancy is known as recurrent pregnancy loss or miscarriage. Also known as repeated spontaneous abortion or habitual abortion, this type of miscarriage can be a cause of concern and distress for women who are trying to have a baby.
According to a study published in the Journal of Obstetrics and Gynecology of India in 2015, Indian women are more likely to suffer recurrent spontaneous miscarriage (RSM) than Westerners. According to the study, "age, (blood) clotting disorders, immunological factors, infections, and genetic disorders were the significant risk factors associated with RSM". Further, the study authors added, the chances of subsequent miscarriage go up by 24.97% after the first miscarriage, 34.04% after the second miscarriage and 21.88% after the third miscarriage.
Usually, a woman who has had recurrent miscarriages is advised to undergo a number of tests to figure out the underlying issue that is causing the miscarriages. These tests include a pelvic exam and blood tests to identify any uterine, genetic or immunological anomalies behind the recurrent miscarriages.
If and when the underlying causes of the recurrent miscarriage is identified, it can be treated accordingly. Since this type of repeated loss of pregnancy is rare, identification of the causes and treatments can vary from person to person.