What is Abdominal ultrasound?
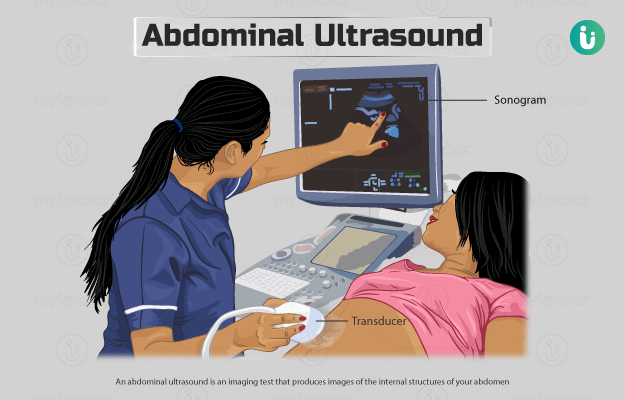
An abdominal ultrasound is an imaging test that produces images of the internal structures of your abdomen including appendix, liver, gall bladder, intestine, pancreas, spleen, urinary bladder and kidney. This test is used to diagnose health conditions in any of these organs.
Ultrasound, also known as sonography, is a non-invasive method that does not use ionizing radiation as in an x-ray or computed tomography (CT) scan. Instead, it uses high-frequency sound waves to create images of the examined area. These sound waves are passed into the examined area with the help of a gel and a small probe called a transducer. These sound waves hit your body tissues and bounce back to the probe. The probe then passes on the information to an attached computer that produces black and white images of the organs.