Summary
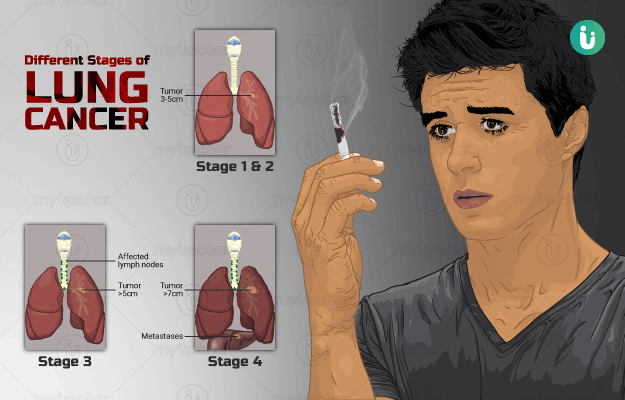
According to the World Health Organization, cancer ranks second on the list of diseases that are leading causes of death worldwide. Out of these, around 70% of people who die from cancer belong to the low-income and middle-income countries. Lung cancer is among the most prevalent types of cancers. High pollution levels, radiation, cigarette smoking and exposure to certain harmful chemicals like asbestos are the common causes and risk factors of developing a lung cancer. Lung cancers are generally classified into three types: small cell, non-small cell and lung carcinoid tumour. Non-small cell lung cancer is the most widespread among the other types of lung cancer. Doctors perform a chest X-ray, CT scan or a PET-CT scan, bronchoscopy, order blood tests and use a spirometer to diagnose lung cancer. Treatment of lung cancer depends upon the type and extent of growth of cancer. The outcome of lung cancer treatment is better if the symptoms presented are due to primary tumours rather than cancerous tumours. The best way to prevent lung cancers is to quit smoking.

 Doctors for Lung Cancer
Doctors for Lung Cancer  OTC Medicines for Lung Cancer
OTC Medicines for Lung Cancer
 Lung Cancer articles
Lung Cancer articles News for Lung Cancer
News for Lung Cancer
 Homeopathic Treatment of Lung Cancer
Homeopathic Treatment of Lung Cancer





































 Editorial Team
Editorial Team

 Dr. Ashu Abhishek
Dr. Ashu Abhishek