Summary
A heart transplant is a surgical method to replace a failing heart with a new donor heart. A transplant surgery is the last option when all other treatment methods have failed. Some conditions in which you are considered ineligible for a transplant surgery include age over 65 years, other major health problems such as a disease of the lungs, kidneys, or any other organ, and smoking or drug abuse.
Click on the link given here, to know in detail about the treatment of heart disease.
To check for your eligibility for the procedure, the doctor will ask you to undergo multiple tests. Once the transplant team reviews your reports, you will be on the waiting list. As soon as a donor’s heart is obtained, your doctor will notify you. Your transplant surgery will mostly be conducted on the same day. After the surgery, you will be in the hospital for about one to two weeks. You will be on multiple medicines, some of which you will need to take for life. After a transplant, you need to be careful to not get any infection as your immunity will be low.
Contact your doctor if you observe any symptoms such as bleeding at the incision site or fever.
(Read More - Enlarged Heart Treatment)
- What is heart transplant surgery?
- Why is heart transplant surgery recommended?
- Who can and cannot get heart transplant surgery?
- What preparations are needed before heart transplant surgery?
- How is heart transplant surgery done?
- How to care for yourself after heart transplant surgery?
- What are the possible complications/risks of heart transplant surgery?
- When to follow up with your doctor after heart transplant surgery?
What is heart transplant surgery?
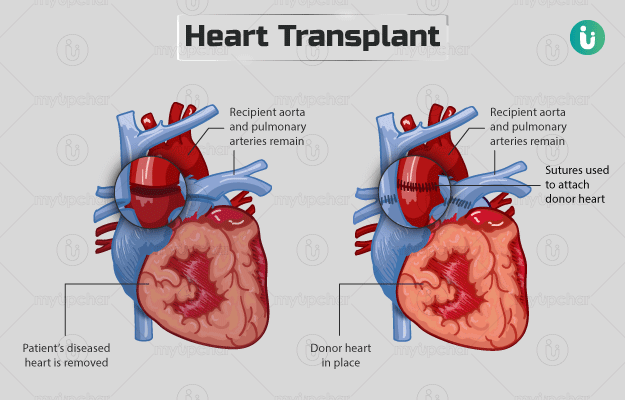
A heart transplant is a surgical technique in which a diseased and failing heart is replaced with a healthy heart from a donor. This surgery is the last option when all other treatments, such as surgeries or medicines, have been unsuccessful.
Heart failure is a medical condition in which the heart cannot effectively pump blood. As all organs in the body require blood to function, when the heart is unable to pump blood adequately, it disrupts the functioning of the other organs. Heart failure may either affect one side of the heart or the entire heart.
(Read More - Angina Treatment)
Why is heart transplant surgery recommended?
A doctor will recommend a heart transplant if you have end-stage heart failure. End-stage heart failure means your heart’s inability to pump blood is severe, and no other treatments are working.
Symptoms of heart failure include:
- Breathing trouble even when resting
- Sudden weight gain
- Chest pain
- Abnormal urination
- Irregular heartbeat
- Bloating
- Swelling in the legs, ankles, feet or abdomen
- Increased heart rate
- Confusion
- Fatigue
- Loss of appetite
- Trouble in performing daily activities
- Feeling out of breath
- Change in sleeping pattern
(Read More - Congenital Heart Disease)
Who can and cannot get heart transplant surgery?
You may be unable to get the transplant surgery if you:
- Have HIV
- Are malnourished
- Had cancer less than two years ago
- Have dementia or have had a severe stroke
- Are older than 65 years
- Have an active infection such as hepatitis
- Have liver, nerves, kidneys, or lungs condition
- Have insulin-dependent diabetes
- Have any disease affecting the blood vessels of your legs and neck
- Have no support from your family and do not follow your treatment
- Smoke, use drugs or abuse alcohol, all of which may affect the new heart
- Have pulmonary hypertension
- Cannot be relied upon to take your medicines or cannot visit the hospital frequently for follow-up visits
(Read More - Congestive Heart Failure)
What preparations are needed before heart transplant surgery?
The following preparations will need to be done before a heart transplant surgery:
-
A transplant team will review your evaluation before the surgery. This evaluation includes:
- Physical check-up.
- Blood tests: The tests help to find a suitable donor, which lowers the risk of organ rejection.
- Diagnostic tests: These check for your overall health and include tests like an ultrasound, CT scan, X-ray, pulmonary function tests (to check how your lungs work), and a dental exam. Women would additionally need a mammogram, Pap smear, and a gynaecology evaluation.
- Psychological evaluation: Some psychological issues associated with a transplant that need to be evaluated are financial problems, stress, and support from friends and family.
- You may require additional vaccines to decrease the risk of infections after transplant surgery.
- Let your doctor know about all your medications and your complete medical and surgical history.
- Once all the tests are done, and you meet the criteria, you will be put on the waiting list. You may have to wait for a few days to more than one year for a donor heart to be available.
- As soon as you are informed that a heart is available for transplant, discontinue eating and drinking anything. You should go to the hospital immediately as the operation needs to be conducted within four hours of recovering the donor heart.
- You need to sign a consent form before the surgery.
(Read More - Endocarditis treatment)
How is heart transplant surgery done?
After you arrive at the hospital, you will be asked to wear a hospital gown. The surgery includes the following steps:
- The doctor will administer general anaesthesia (a sleep-inducing medicine) and shave your chest if necessary.
- Your chest will be cleaned with an antiseptic solution.
- The surgeon will make a vertical incision from the end of your neck to just above your belly button.
- He/she will cut your breastbone and open it apart to get access to your heart.
- Next, the surgeon will stop your heart for the surgery. To keep up circulation in your body during the procedure, the surgeon will join the tubes attached to the bypass machine into your chest. The machine will pump blood through your body like your heart.
- Once the machine takes over the pumping role, the surgeon will replace your diseased heart with a healthy heart.
- He/she will then reconnect all the blood vessels to the new heart and give it a slight electric shock to start functioning. The ventilator tubes will be removed before this.
- The surgeon may attach wires in your heart which will be connected to a pacemaker outside the body to help in adjusting the pace of the heart until the time of recovery.
- He/she will reattach your breastbone with wires, and stitch up your skin using sutures or staples.
- A health care practitioner will place a drain in your chest to drain any accumulated blood or fluid around the heart and will apply a dressing on the incision.
The heart transplant surgery takes about four hours.
After the operation, you will be under observation in the intensive care unit for some days. A nurse may administer medicine for pain.
You will undergo some blood tests to determine if the new heart and other organs are functioning properly. You may also need some medication to regulate your blood pressure and to control any bleeding problems. The doctor will remove the wires attached to the pacemaker and monitor your dose of immunosuppressants (anti-rejection medication).
You will start with drinking liquids and slowly progress to solid foods. Once your vitals are stable enough, the medical staff will shift you from the intensive care unit to a private room for further recovery. Your doctor will suggest you to walk around and take a healthy diet.
You will be given discharge after seven to 14 days.
(Read More - Rheumatic Heart Disease)
How to care for yourself after heart transplant surgery?
Once you go home after the transplant surgery, keep these pointers in mind:
- You will need to take immunosuppressant medication for your entire life as prescribed by the doctor.
- You will need to keep a daily record of the following which the doctor will check in every follow-up appointment:
- Heart rate
- Weight
- Temperature
- Blood pressure
- Blood glucose
- Keep the wound dry and clean.
- Avoid crowded places and anyone with an infection in the initial few months of recovery to lower your chances of infections.
- Avoid driving for about six weeks after the surgery.
- You can resume work in about two to three months after the transplant surgery.
- You should not lift, push, or pull any heavy weights for six weeks after the surgery.
- Avoid using hot tubs, swimming pools, or bathtubs until your incision is completely healed.
- You can perform activities like brisk walking, stationary bike riding, or dancing five times a week for about half an hour.
- Avoid travelling for long distances for the first three months to prevent any infections.
- You will likely be allowed to travel domestically after three months, but you will have to wait for six months to travel internationally.
- Avoid any gardening activity for six months.
- Wear a mask while gardening after six months and when you walk past any construction site.
- You may attend support meetings if you wish to meet people who have undergone a transplant to discuss your concerns and share advice.
The heart transplant will increase the life span of people who would have died without the transplant.
When to see the doctor?
Contact the doctor if you experience the following symptoms:
- Excessive pain at the surgery site
- Low blood pressure
- Fever, chills, or both
- Excessive fatigue
- Breathing problem
- Redness, swelling, drainage, or bleeding from the wound
(Read More - Cardiomyopathy treatment)
What are the possible complications/risks of heart transplant surgery?
The following are some possible risks and complications of a heart transplant surgery:
- Reaction to the anaesthetic
- Heart attack
- Bleeding
- Infection
- Blood clots
- Breathing problems
- Heart rhythm problems
- Anti-rejection medicines causing cancer or damage to the liver, kidney, or other organs
- Kidney or lung failure
- Increased risk of infections due to the rejection medicines
- High cholesterol, bone thinning, or diabetes due to anti-rejection medicines
- Rejection of the new heart
- The new heart may not function at all
- Severe coronary artery disease
(Read More - Valvular Heart Disease treatment)
When to follow up with your doctor after heart transplant surgery?
For the first two months after discharge, you will have a weekly visit to the clinic.
Even in the initial few months, you will have frequent follow-ups in the initial few months after the transplant surgery, at which the doctor will perform certain tests to check if your body is accepting the new heart. These tests include electrocardiograms and heart biopsies (a thin needle is used to remove the heart tissue for examining it under a microscope).
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
(Read More - Hypertrophic cardiomyopathy treatment)
Surgery Cost In Your City
References
- Chiu P, Robbins RC, Ha R. Heart transplantation. In: Sellke FW, del Nido PJ, Swanson SJ, eds. Sabiston and Spencer Surgery of the Chest. 9th ed. Philadelphia, PA: Elsevier; 2016:chap 98.
- University of Rochester Medical Center [Internet]. Rochester (NY): University of Rochester Medical Center; Heart Transplantation Procedure
- Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM. Pediatric heart and heart-lung transplantation. In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 470.
- Yancy CW, Jessup M, Bozkurt B, et al. 2017 ACC/AHA/HFSA Focused Update of the 2013 ACCF/AHA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of Amer. J Card Fail. 2017;23(8):628-651. PMID: 28461259.
- Jessup M, Atluri P, Acker MA. Surgical management of heart failure. In: Zipes DP, Libby P, Bonow RO, Mann, DL, Tomaselli GF, Braunwald E, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 11th ed. Philadelphia, PA: Elsevier; 2019:chap 28.
- Mancini D, Naka Y. Cardiac transplantation. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 25th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 82.
- UK Healthcare [Internet]. University of Kentucky. US; Pre-Heart Transplantation Guide
- UCSF health: University of California [internet]. US; Heart Transplant Recovery
- Cedars Sinai [Internet]: Cedars Sinai Medical Center. Los Angeles. US; Adult heart transplant