Summary
Endometrial ablation is a procedure that is done for the treatment of heavy periods. In this procedure, the surgeon removes the endometrium or the inner lining of the uterus using extremely cold temperature (cryoablation), electric current (electrocautery), or heated fluid (hydrothermal). The procedure does not need any cuts or incisions, instead, a hysteroscope or other instruments are inserted in through the vagina.
You will have to undergo a biopsy prior to the procedure. Also, fasting for at least eight hours is also necessary. On the day of the procedure, your doctor will suggest you to take sanitary napkins to the hospital as you will be bleeding for a while afterwards.
Women who undergo this procedure may not be able to get pregnant afterwards.
Initially, after the surgery, your periods will still be heavy. However, the flow will gradually reduce over the months. You must refrain from heavy lifting, strenuous activities, and sexual intercourse for a few weeks after this procedure. to allow proper healing of the operated area.
- What is endometrial ablation?
- Why is endometrial ablation recommended?
- Who can and cannot get endometrial ablation?
- What preparations are needed before endometrial ablation?
- How is endometrial ablation done?
- How to care for yourself after endometrial ablation?
- What are the possible complications/risks of endometrial ablation?
- When to follow up with your doctor after endometrial ablation?
What is endometrial ablation?
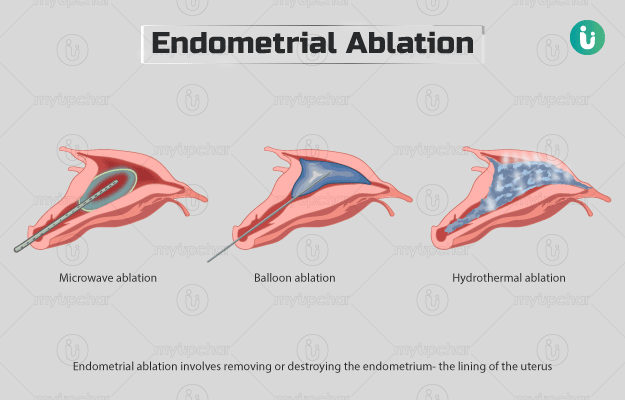
Endometrial ablation involves removing or destroying the endometrium- the lining of the uterus (womb) to treat menorrhagia (abnormally heavy and/or prolonged periods). The procedure is only performed in women who do not wish to become pregnant because endometrial ablation can prevent the attachment of eggs to the lining of the uterus, thus not allowing a pregnancy.
Doctors initially prescribe medications such as hormonal pills or non-hormonal medicines (e.g., mefenamic acid) and uterine hormonal devices to treat this condition. However, if these treatments do not work, he/she may suggest endometrial ablation. After this procedure, your periods may either reduce or stop; thus, reducing the unpleasant symptoms. Endometrial ablation does not involve any incision over the uterus instead, he/she will insert probes or instruments through your vagina.
Why is endometrial ablation recommended?
This procedure is recommended for the management of menorrhagia. The following are the signs of menorrhagia:
- Heavy bleeding even through your clothes or bed sheet
- Need to use several types of sanitary products (pads and tampons) together
- Passage of large blood clots
- Need to change your sanitary napkin every two hours
Some conditions that can cause menorrhagia are:
- Hormonal problems
- Endometriosis (endometrial tissue is present outside the womb)
- Fibroids (non-cancerous growth inside or around the uterus)
- Uterine cancer
- Polycystic ovary syndrome (a common condition that causes irregular periods)
- Polyps (non-cancerous growth inside the uterus lining)
Who can and cannot get endometrial ablation?
Endometrial ablation is performed under the following conditions:
- If the woman has intrauterine devices in place
- Abnormal shape or structure of the uterus
- If the woman is planning to become pregnant in the future
- Previous surgeries for fibroids
- Recent pregnancy
- Pelvic inflammatory disease
- Weak muscles of the uterine wall
- Vertical or classic cut for cesarean section
- Cervical infection or vaginal infection
- Cancer of the endometrium, uterus, or cervix (the opening of the uterus)
What preparations are needed before endometrial ablation?
Before undergoing this procedure, you will need the following preparations:
- You will be asked to undergo a few diagnostic tests, including biopsy of the endometrium. This will help the doctor to determine if you have polyps or cancer in the endometrial tissue.
- Notify your healthcare provider if you are diabetic or have kidney disease or heart disease.
- Ensure to report your doctor if you are or can be pregnant.
- Share a list of all the medicines that you take, including non-prescribed medicines, herbs, vitamins, and supplements.
- Your doctor may prescribe you certain hormones to block the formation of oestrogen (female sex hormone) to help thin the lining of your uterus so that the procedure is more effective. These should be started one to three months prior to the procedure.
- You will need to consume medicines that open your cervix eight to 12 hours before the procedure.
- Discontinue blood-thinning medications (ibuprofen, aspirin, clopidogrel, etc.) for at least two weeks before the procedure.
- Smoking cessation before and after the operation will help reduce your chances of postoperative complications.
- Inform your surgeon if you are allergic to any medicines or things used during surgery, for example, latex, anaesthesia, or surgical tape.
- You will be asked to fast for at least eight hours before this procedure.
- Carry sanitary napkins to the hospital for use after the procedure.
- Arrange for someone to drive you home after the procedure.
- You will be asked to sign an approval or consent form if you agree to the procedure.
How is endometrial ablation done?
After your admission to the hospital, the medical staff will provide you with a hospital gown. They will place an intravenous catheter (tube) in your arm or hand to administer medications.
- You will be asked to sit on the operating table with your legs placed in stirrups (an apparatus that holds the legs in the desired position).
- General anaesthesia will be administered to keep you relaxed and pain-free.
- A catheter will be inserted inside your bladder to allow the drainage of urine.
- The healthcare provider will then use a tool (speculum) to open up your vagina and reach your cervix.
- He/she will use forceps to hold your cervix firmly in place and use rods of various sizes to gradually dilate it enough for inserting a hysteroscope (a thin rod-like instrument with a camera at the end). The hysteroscope will be connected to a screen, through which the surgeon will be able to see the inside of your uterus and perform the procedure with precision.
- Next, based on the tool, the surgeon will use one of the following methods for ablation:
- Microwave ablation: The surgeon will use a thin probe to send microwave energy and destroy your endometrium.
- Electrical ablation: The surgeon will send in a rollerball or wire loop through the hysteroscope into your uterus. Electric current will be through this tool and the tool will be moved across the lining of the uterus to destroy it.
- Hydrothermal ablation: The surgeon will pump in heated fluid through the catheter to destroy your endometrial lining. Once this procedure is done, he/she will pump out the fluid.
- Once the procedure is done, the surgeon will carefully remove the tool used for ablation.
The ablation procedure can also be conducted without a hysteroscope. It is performed under the effect of local anaesthesia and includes the following steps:
- The surgeon will use a uterine sound, which is a thin rod-like instrument, through your cervix to gauge the length of your uterus and cervical canal.
- Once that is done, he/she will remove the rod and use one of the following methods to destroy your uterine lining:
- Balloon ablation: The surgeon will place in a small thermal balloon inside your uterus and fill the balloon with hot liquid to destroy your uterine lining. The temperature, pressure and time of treatment will be controlled by a computer.
- Cryoablation: The surgeon will insert a cryoablation probe inside your uterus. He/she will use ultrasonography to guide the probe to the areas that will require freezing. The extreme cold temperature from the probe will help destroy the lining of the uterus.
- Radiofrequency ablation: The surgeon will place a special mesh in your uterus which will then be expanded to occupy the uterus. Then the surgeon will pass radio wave energy into the mesh, which will destroy your uterine lining.
- Finally, the surgeon will use suction to remove the contents of your uterine lining as needed. After completing the procedure, he/she will remove the tools through your vagina.
This is a quick procedure that takes only 15 to 45 minutes. If general anaesthesia were used during the procedure, the medical team will move you to the recovery room to monitor your vital functions. Usually, the patient is sent home on the same day.
How to care for yourself after endometrial ablation?
Once you are home, you should take care of yourself in the following manner:
- Medications: Your doctor may prescribe painkillers to reduce cramps or soreness after the procedure. Take them as directed.
- Bathing:
- You may be allowed to take a shower. However, the surgeon may suggest you to avoid soaking in a bathtub for a few days after the procedure.
- Bleeding:
- It is normal to bleed for six to eight weeks after endometrial ablation. You may also observe watery discharge for a few weeks.
- Initially, you will experience heavy periods that will gradually reduce over the months.
- Diet: Take a balanced diet and keep yourself hydrated. Tell the doctor if the painkillers cause poor appetite.
- Activities:
- You may be able to perform your everyday activities two days after the procedure.
- Avoid driving until you are on painkillers.
- Avoid using tampons or douches (prepackaged mixes of water and vinegar, iodine, or baking soda) for at least one to two weeks after endometrial ablation.
- Restrict your sexual activities for a week. Continue using contraceptives to prevent pregnancy even after this procedure.
- Do not perform strenuous activities or lift heavy objects until your doctor allows you to.
When to see the doctor?
Contact or visit your healthcare provider immediately if you experience the following symptoms:
- Fever
- Problem in urinating
- Chills
- Nausea or vomiting
- Chest pain
- Cough
- Heavy bleeding for more than two days
- Foul-smelling discharge from the vagina
- Severe abdominal pain
- Difficulty breathing
- Lower back pain
- Severe pain during sex
- Abdominal cramps
- Tenderness or pain in the leg or calf
What are the possible complications/risks of endometrial ablation?
The endometrial ablation procedure is known to carry the following risks:
See Similar Category Medicines Here
When to follow up with your doctor after endometrial ablation?
You may have to visit your doctor after four weeks of the procedure. Your doctor will check the success of the procedure with you and discuss any treatment plan for the future.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Surgery Cost In Your City
References
- Johns Hopkins Medicine [Internet]. The Johns Hopkins University, The Johns Hopkins Hospital, and Johns Hopkins Health System; Endometrial Ablation
- South Tees Hospitals [Internet]. National Health Service. NHS Foundation Trust. UK; Endometrial Ablation
- National Health Service [Internet]. UK; Heavy periods
- Minalt N, Canela CD, Marino S. Endometrial Ablation. [Updated 2020 Nov 3]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan
- Carlson SM, Goldberg J, Lentz GM. Endoscopy, hysteroscopy and laparoscopy: indications, contraindications, and complications. In: Lobo RA, Gershenson DM, Lentz GM, Valea FA, eds. Comprehensive Gynecology. 7th ed. Philadelphia, PA: Elsevier; 2017:chap 10
- Baggish MS. Minimally invasive nonhysteroscopic endometrial ablation. In: Baggish MS, Karram MM, eds. Atlas of pelvic anatomy and gynecologic surgery. 4th ed. Philadelphia, PA: Elsevier; 2016:chap 110
- Springfield Hospital [Internet]. Chelmsford. UK; Microwave Endometrial Ablation
- Beth Israel Lahey Health: Winchester Hospital [Internet]. Winchester. Maryland. US; Endometrial Ablation
- UW Medicine [Internet]. University of Washington Medical Center. Washington DC. US; After Your Endometrial Ablation