Summary
Decompressive craniectomy is performed to relieve pressure on the brain resulting from a brain swelling that is caused by an injury or other conditions. The procedure involves the removal of a part of the skull to allow space for the swelling to grow upwards. You will remain asleep during the whole procedure. The part of the skull removed during the surgery will be replaced a few months after recovery. In some cases, a synthetic skull is placed instead of the original part of the skull. Your stay at the hospital depends on the extent of injury to the brain. This surgery is associated with a longer recovery period, which could be anywhere from a few months to years. You may also be required to undergo rehabilitation for complete recovery from the surgery.
- What is decompressive craniectomy?
- Why is decompressive craniectomy recommended?
- Who can and cannot get decompressive craniectomy?
- What preparations are needed before decompressive craniectomy?
- How is decompressive craniectomy done?
- How to care for yourself after decompressive craniectomy?
- What are the possible complications/risks of decompressive craniectomy?
- When to follow up with your doctorafter a decompressive craniectomy?
What is decompressive craniectomy?
Decompressive craniectomy is a surgery that involves the temporary removal of a part of the skull to relieve pressure on the brain.
Your brain is closely protected by your skull, such that there is very little space between the skull and the brain. However, a few conditions such as head injury can damage the blood vessels in the brain, resulting in leakage of blood and brain swelling.
In such cases, the tiny space between the skull and brain may not be enough to accommodate the swelling and leads to increased pressure inside the skull. If the swelling and the resultant pressure inside the skull are left uncontrolled, it could damage the cells in the brain and lead to coma, brain damage or death.
Craniectomy helps in relieving this pressure and reduces the possibility of resultant brain damage.
Why is decompressive craniectomy recommended?
Your doctor may recommend this surgery in case of any of the following conditions that could lead to increased pressure inside your skull:
- Subarachnoid haemorrhage (bleeding due to damage to any blood vessel present at the surface of the brain) Read more: Brain haemorrhage symptoms
- Severe head injury
- Brain infection
- Swelling from a brain tumour
- Stroke (death of brain cells due to decreased flow of blood to a part of the brain caused by blood clots or damage to blood vessels). This can lead to symptoms such as headaches, difficulty in speaking, seeing or understanding speech, sudden weakness, paralysis or numbness on one side of the body or the face
Increased pressure inside your skull could result in the following symptoms:
- Sudden, severe headache
- Confusion
- Vomiting or nausea
- Loss of consciousness
- Seizures
Who can and cannot get decompressive craniectomy?
Your doctor may not recommend this surgery if you:
- Are more than 65 years old
- Have a Glasgow Coma Scale score of 3, (this scale evaluates the severity of head injury after a trauma, and a score of 3 indicates a high mortality rate)
- Have irreversible systemic disease (an infection in the bloodstream that cannot be treated)
- Have suffered a trauma that will not allow you to survive for more than 24 hours
- Have intracranial hypertension (high blood pressure inside the skull for more than 12 hours despite treatment with medicines)
What preparations are needed before decompressive craniectomy?
Individuals who need decompressive craniectomy are usually in the hospital and being closely monitored. They might also be under sedation and needing ventilator support. Since this surgery is mostly performed as emergency surgery, preparing for it beforehand may not be possible. You should inform the doctor if you are taking any medicines or supplements or if you have any allergies. You will be given a consent form to sign to give permission for the surgery. If any other preparation is needed, the hospital staff will discuss with either you or your family member.
You can expect the following at the hospital before the surgery:
- The surgeon will ask you or your family member about your medical history and conduct a physical examination.
- You may not be allowed to eat/drink anything before the surgery.
- The medical staff will perform an imaging test, probably a computed tomography scan of your head. It is an imaging test that uses a computer and x-rays to create a detailed picture of the internal structures of your head.
How is decompressive craniectomy done?
You will be under general anaesthesia during the surgery, i.e., you will be unconscious throughout the procedure. A neurosurgeon will perform this surgery. The procedure usually involves the following steps:
- The hospital staff will take you to the operating room.
- An anesthesiologist will administer general anaesthesia through an intravenous (IV) line and closely monitor your vital signs throughout the surgery.
- You will also be given antibiotics through an IV line to prevent infection.
- A breathing tube will be put down your throat to control your breathing during the surgery.
- A healthcare practitioner will remove (shave) and clean your hair around the portion of the skull to be removed.
- The neurosurgeon will make a cut on the cleaned portion of your scalp and pull aside the skin and tissues.
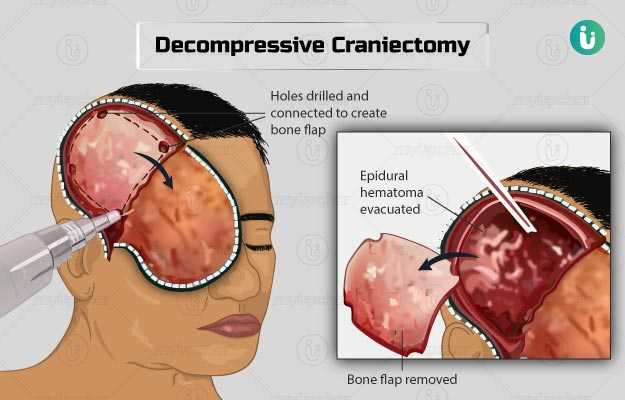
- He/she will then make holes in your skull using a special drill, and use a saw to connect the holes and to remove the desired part of the skull
- The bone will be stored in a freezer so that it could be replaced after the swelling in your brain subsides.
- The surgeon will make a cut in the tissue covering your brain and will make necessary repairs to reduce the swelling.
- After the swelling subsides, the neurosurgeon will place a mesh piece over it.
- Finally, he/she will close up your skin with sutures.
You will be moved to the intensive care unit after the surgery where you will be closely monitored. The outcome of this surgery may not be visible immediately after the surgery as the brain takes some time to recover from injury and swelling. Your stay in the hospital after the surgery will depend on the extent of injury to the brain. In some conditions, you may need to be hospitalised for at least two months until you have recovered enough to resume your normal activities.
How to care for yourself after decompressive craniectomy?
Depending on the severity of the injury, you may require a few months to years to completely recover.
Once you are discharged from the hospital, you can expect the following after a decompressive craniectomy:
- You may have symptoms, such as muscle weakness, after the surgery. These symptoms usually depend on the nature of the injury.
- The cut in your scalp may cause some pain. You may be prescribed medicines to reduce the pain.
- You will have to use a special helmet to protect your brain from injury after the surgery, at least until the bone is replaced.
- You may have to go through rehabilitation to recover from symptoms after the surgery. The surgeon may recommend occupational and physical therapy to help you recover from the weakness after the surgery.
- You may also be asked not to do the following for a few days after the surgery:
- Having a shower
- Exercising or performing similar physical activities
- Drinking alcohol
- Smoking
- Driving a vehicle
- Lifting objects that weigh over 2kg
This life-saving surgery helps to reduce swelling in the brain and limits the damage to the brain.
When to see the doctor?
You should contact the surgeon immediately if you have any of the following symptoms after the surgery:
- Fever
- Seizures
- Shortness of breath
- Vomiting
- Drainage from the wound
- Redness or hotness in the scalp around the wound
What are the possible complications/risks of decompressive craniectomy?
The following risks are associated with this surgery:
- Infection in the brain or spine
- Further brain damage
- Bleeding around the membranes of the brain (meninges)
- Seizures
- Heart attack
- Blood clot formation
- Abnormal accumulation of cerebrospinal fluid
- Partial or complete paralysis
- Inability to speak
- Vegetative state, a condition wherein you will lack awareness even while being awake
These complications may even lead to coma or death.
When to follow up with your doctorafter a decompressive craniectomy?
The neurosurgeon will ask you to visit the hospital a few months after the surgery to replace the bone that was removed. The bone is checked for growth of bacteria, and in the absence of any bacterial growth, so it can be placed back in the skull at its original location. However, if the bone shows the presence of bacterial growth, a synthetic skull replacement is used.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Surgery Cost In Your City
References
- Schirmer CM, Ackil AA Jr, Malek AM. Decompressive craniectomy. Neurocrit Care. 2008;8(3):456‐470. PMID: 18392785.
- Saint Luke's Health System [Internet]. Kansas city. US; What is craniectomy?
- UR Medicine: Highland Hospital [Internet]. University of Rochester Medical Center. New York. US; Craniectomy
- Harvard Health Publishing. Harvard Medical School [internet]: Harvard University; Subarachnoid Hemorrhage
- National Cancer Institute [Internet]. Bethesda (MD): U.S. Department of Health and Human Services; NCI Dictionary of Cancer Terms
- National Heart, Lung, and Blood Institute [Internet]. Bethesda (MD): U.S. Department of Health and Human Services; Stroke
- Alvis-Miranda H, Castellar-Leones SM, Moscote-Salazar LR. Decompressive craniectomy and traumatic brain injury: a review. Bull Emerg Trauma. 2013;1(2):60‐68. PMID: 27162826.
- Demetriades D, Kuncir E, Velmahos GC, Rhee P, Alo K, Chan LS. Outcome and prognostic factors in head injuries with an admission Glasgow Coma Scale Score of 3. Arch Surg. 2004;139(10):1066-1068. PMID: 15492144.
- Grindlinger GA, Skavdahl DH, Ecker RD, Sanborn MR. Decompressive craniectomy for severe traumatic brain injury: clinical study, literature review and meta-analysis. Springerplus. 2016;5(1):1605. Published 2016 Sep 20. PMID: 27652178.
- Howard JL, Cipolle MD, Anderson M, et al. Outcome after decompressive craniectomy for the treatment of severe traumatic brain injury. J Trauma. 2008;65(2):380‐386. PMID: 18695475.
- Livesay S, Moser H. Evidence-based nursing review of craniectomy care. Stroke. 2014;45(11):e217‐e219. PMID: 25316281.
- Ding Jun, Guo Yan, Tian Hengli. The influence of decompressive craniectomy on the development of hydrocephalus: a review. Arq. Neuro-Psiquiatr. 2014; 72(9).
- Gouello G, Hamel O, Asehnoune K, Bord E, Robert R, Buffenoir K. Study of the long-term results of decompressive craniectomy after severe traumatic brain injury based on a series of 60 consecutive cases. ScientificWorldJournal. 2014;2014:207585. Published 2014 Feb 24. PMID: 24719566.
- Hutchinson PJ, Kolias AG, Timofeev IS, et al. Trial of Decompressive Craniectomy for Traumatic Intracranial Hypertension. N Engl J Med. 2016;375(12):1119‐1130. PMID: 27602507.
- Santana-Cabrera L, et al. Complications of post–injury decompressive craniectomy. Int J Crit Illn Inj Sci. 2012 Sep-Dec; 2(3): 186–188. PMID: 23181215.