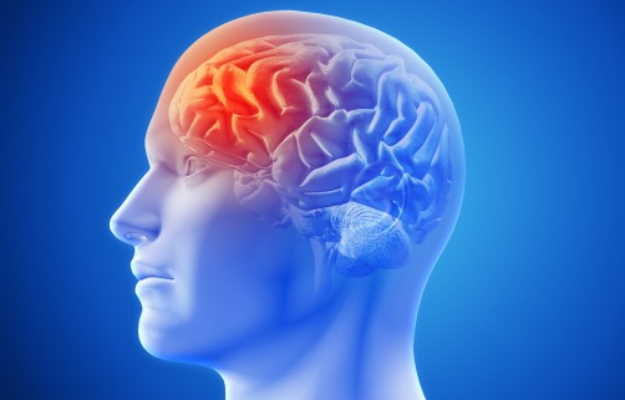
An epidural hematoma is defined as a collection of blood in the space between the dura (protective lining that covers the brain) and the skull bone. Sometimes, this may occur in the spinal column as well. This is defined as a collection of blood in the extradural space and can be referred to as an extradural hemorrhage. Extradural means that it is outside the dura.
In the spinal column of our body, the epidural space is defined as a space that is between the vertebral column (backbone) and the dura mater which is the protective lining covering the brain. If the epidural hematoma occurs in the spinal column it is termed as a spinal extradural hematoma.
Inside our head, the epidural space is a potential space. It is between the skull bone and the dura mater. It is a known fact that the dura mater is very tightly bound to the inside of our skull. An extradural hematoma that occurs in this potential space is termed as an intracranial extradural hematoma.
Some doctors refer to an epidural hematoma as an extradural or epidural hemorrhage as it means that there is bleeding that has occurred. A subdural hematoma is a condition in which there is accumulation of blood in the subdural space.
(Read more: Brain Hemorrhage)

 Doctors for Epidural Hematoma
Doctors for Epidural Hematoma  Surgery for Epidural Hematoma
Surgery for Epidural Hematoma