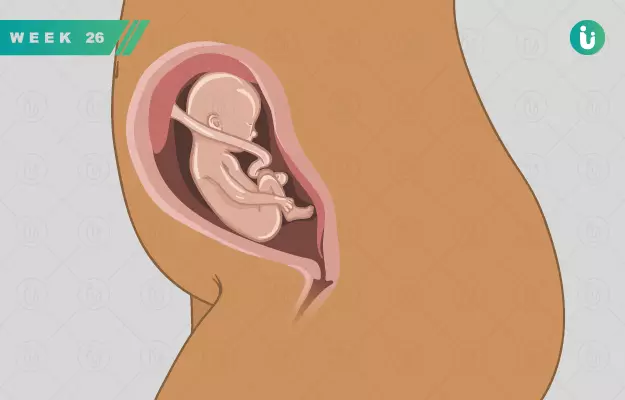
Welcome to the second-last week of your second trimester! By now, you must be quite adept at handling your pregnancy diet, pregnancy exercise routine, pregnancy check-ups, ultrasound, etc. You're probably very good at knowing your baby’s movements and response times, too, at this point.
However, as the third trimester approaches, you’re also likely to feel more tired, slow and uncoordinated—and that’s because your baby bump is still growing as your baby keeps growing. This is the reason why most pregnant women naturally slow down a little in the tailend of the second trimester, and continue to experience this in the third trimester as well. This is absolutely normal, and you should not worry about feeling more lethargic or becoming slower as long as you’re healthy and so is your baby in the womb.
Your baby is probably quite active at this juncture, but if you observe any slowing down in his or her movements, you should call your doctor immediately. There are a number of symptoms of pregnancy that will show up around this week, like fatigue, sleep issues, indigestion and dizziness. This is another reason why you should take things a little slow.
This apart, you should look out for infections and other complications this week. Gestational diabetes and hypertension could show up, which is why you should check your sugar and salt consumption even more than before. Make sure you also monitor your mental health and engage with other mothers-to-be, relatives, friends and your partner to keep depression during pregnancy at bay. Here’s everything you need to know about the 26th week of pregnancy.