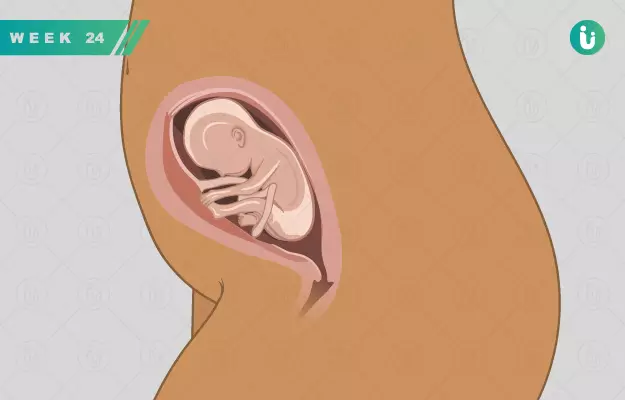
Welcome to the 24th week of pregnancy! If your baby’s kicking in the womb is old news by now, here’s something new to celebrate: your baby is now considered to be viable. This means that if for any reason you go into premature labour this week, your baby can survive given the right neonatal medical support.
To be sure, a premature baby can face a number of disadvantages. So an early delivery is not ideal. But still, this can be a source of relief, especially if your pregnancy has been fraught with complications.
This apart, you should continue with your regular pregnancy routine for prenatal care, which includes a good pregnancy diet, pregnancy exercises, pregnancy checkups, and ultrasounds as per your doctor’s recommendations.
If you’re doing all this, then there shouldn’t be much to worry about at this stage—you can sit back and relax this week. However, it’s important to discuss gestational hypertension and gestational diabetes with your doctor, and get tests done if you’re at risk or can see symptoms emerging. It’s equally important to keep an eye on your mental health, as depression during pregnancy can happen to anyone.
Communicating your feelings and experiences with your spouse, family and friends is therefore as important as keeping stress and anxiety at bay. Keep in touch with your doctor and don’t be afraid to ask questions about your health or that of your baby if you do have any concerns. Here’s everything you need to know about the 24th week of pregnancy, and what happens during it.