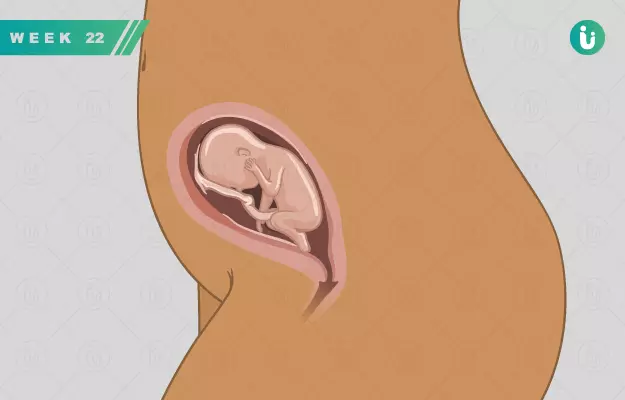
Welcome to the 22nd week of pregnancy! This is one of those weeks when you can just spend time getting to know your growing baby bump better by cooing, singing and talking to it. Your baby’s movements in the womb are now becoming more pronounced, so obviously you’ll also enjoy the interactions these simple activities will provide.
You won’t be up for another foetal ultrasound until the third trimester starts. If your pregnancy symptoms are manageable and no complications show up, then you won’t need to visit a doctor this week for a pregnancy check-up either. This is the perfect opportunity to rest up, take things slow and plan ahead for the rest of your pregnancy, while maintaining your pregnancy diet and exercise routine for pregnancy.
As your baby bump keeps growing, you might feel a little more unbalanced and observe more stretch marks appearing on your skin. Many women also experience varicose veins during pregnancy, which show up on the legs, vaginal area and buttocks. While Braxton Hicks contractions usually show up in the third trimester, some women can also experience them in the second trimester.
These contractions are nothing to worry about, but you should still keep your doctor in the loop about them and go in for a check-up if they intensify. While there’s no need to unnecessarily worry about your health or that of your baby this week, you should keep an eye out for any signs of complications, especially infections. Here’s everything you need to know about the 22nd week of pregnancy.