Summary
Bariatric surgery is a weight loss surgery in which certain changes are made in the digestive system (either stomach or intestines) to either reduce your total calorie intake or the absorption of nutrients in your gut. This surgery can be performed in different ways such as a laparoscopic adjustable gastric band, gastric sleeve, gastric bypass, and biliopancreatic diversion/duodenal switch. Before the surgery, physical examination and tests are performed to check your health. You may need to fast for a few hours before the surgery. During the surgery, general anaesthesia is given. After the surgery, care must be taken to keep the wounds clean and dry. You will lose weight up to 2 to 3 years after the surgery.
- What is bariatric surgery?
- Why is bariatric surgery recommended?
- Who can and cannot get bariatric surgery?
- What preparations are needed before bariatric surgery?
- How is bariatric surgery done?
- How to care for yourself after bariatric surgery?
- What are the possible complications/risks of bariatric surgery?
- When to follow up with your doctor after a bariatric surgery?
What is bariatric surgery?
Bariatric surgery is also called metabolic surgery or weight loss surgery. In this surgery, doctors modify your digestive system which either makes you eat less or reduces the absorption of food in your body. These modifications include:
- Reducing the size of the stomach: To make you eat less, doctors may reduce the size of your stomach. This restricts the amount of food your stomach can hold, making you feel full sooner and, in turn, reducing your calorie intake per meal.
- Modifying your intestine: Certain changes in the intestine such as creating a bypass prevents the absorption of nutrients and calories from food.
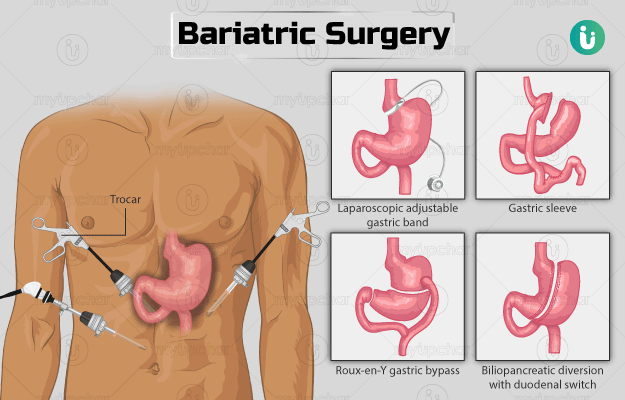
Depending on the procedure, the following types of bariatric surgery can be done:
- Laparoscopic adjustable gastric band (LAGB): In this surgery, a band is placed around the stomach. The band constricts the stomach area, making you feel full early.
- Gastric sleeve: In this surgery, some part of the stomach is removed so it can take in less food than normal.
- Gastric bypass/Roux-en-Y gastric bypass: In this surgery, a small pouch is made from the upper part of the stomach, which is then attached to the small intestine. This will prevent the absorption of calories from food and also make you feel full sooner.
- Biliopancreatic diversion with duodenal switch (BPD/DS): In this surgery, a small portion of the stomach is removed (vertically) to create a tubular stomach pouch. Then, a huge part of the small intestine is bypassed so that the food goes directly into the end part of the small intestine.
Your doctor will decide which surgery is suitable for your weight loss. It is important to note that bariatric surgery is not a substitute for a healthy lifestyle.
If you are tired of dieting and exercising and are not able to lose weight, then use myUpchar Ayurveda Medarodh Fat Burner Capsule, it has no side effects, order it today and avail the benefits.
Why is bariatric surgery recommended?
Your doctor may suggest bariatric surgery to you if you have severe obesity or the following health conditions related to obesity:
- Type 2 diabetes
- High blood pressure
- High cholesterol
- Gastroesophageal reflux disease (GERD)
- Asthma
- Sleep apnoea
Here is a breakdown of some specific types of bariatric surgery that are recommended in certain conditions
Gastric bypass surgery is recommended in individuals with the following conditions:
- Diabetes
- High BMI
- Severe reflux disease
Gastric sleeve surgery is recommended in individuals:
- Who have had multiple abdominal surgeries
- Who weigh more than 200 kg
- Who are on multiple medications for mental disorder
Who can and cannot get bariatric surgery?
Anyone with a Body mass index (BMI) above 30 and associated conditions including uncontrolled diabetes, high cholesterol, high blood pressure, sleep apnoea, fatty liver disease may be asked to undergo this surgery. A person with extreme obesity - a BMI of 40 or higher - may also be advised to get a bariatric surgery.
There are no absolute contraindications (when a procedure is completely inadvisable) for bariatric surgery, but the relative contraindications (when having the procedure may not be advisable) include:
- Drug or alcohol dependency
- Heart failure
- Unstable coronary artery disease
- End-stage lung disease
- Portal hypertension (increased blood pressure in the vein carrying blood from digestive organs to the liver)
- Impaired intellectual capacity
- Ongoing cancer treatment
What preparations are needed before bariatric surgery?
Before a bariatric surgery surgery, your surgeon will ask you to get various tests such as:
- A complete physical examination
- Blood tests and other tests, like an ultrasound of the gallbladder, to ensure you are in good health for the surgery
- Chest X-ray to check the health of your lungs
- An imaging study of the stomach or upper endoscopy
- Electrocardiogram (ECG) to check heart rate
The surgeon may ask you to see other healthcare providers to:
- Get nutritional counselling
- Check if you are emotionally ready for this surgery
- Check if you have problems like diabetes, high blood pressure, and heart or lung problems and to ensure that they are well controlled
You should inform your doctor if you:
- Are taking any medicines like non-prescription or prescribed medicines, herbs, vitamins, and other supplements
- Had any illness like fever or infection recently
- Have a history of bleeding disorders
- Are or could be pregnant
- Use any machine for sleep apnoea or other breathing disorders
- Are taking blood-thinning medicines like aspirin, ibuprofen, vitamin E or warfarin
- Are allergic or sensitive to any medicines, latex, anaesthetic medicine, or tape
Your healthcare practitioner may ask you to do the following things before the surgery:
- Quit smoking because smoking increases the risk of problems and slows down recovery Read more: Effects of smoking on body
- Get counselling to discuss unorganised eating habits and emotional health
- Lose weight by following a special diet
- Read material about the surgery that includes the procedure, expected results and complications
On the day of the surgery:
- Fasting for 6 hours before the surgery is needed
- Take all the medicines given by your healthcare provider with a little amount of water
Also, after the surgery, you will need someone to drive you home.
How is bariatric surgery done?
The procedure for each bariatric surgery is different. All the surgeries can be done laparoscopically as follows:
- Your healthcare practitioner will first give you general anaesthesia so that you feel sleepy and have no pain.
- The surgeon will then make one to five small cuts in your abdomen.
- Through these cuts, a tiny camera called a laparoscope and small instruments required to operate will be placed inside your belly.
Laparoscopic adjustable gastric band
The duration of LAGB is 30 to 60 minutes. After the laparoscope and instruments are placed in your stomach, the following procedure will be followed:
- The surgeon will place a band around the upper area of your stomach to separate it from the lower bottom area.
- This forms a small upper pouch with a narrow opening that enters into a larger bottom area of stomach.
- This surgery does not need stapling or cuts inside the abdomen. A small access port that is connected to the band will be placed below your skin to allow the surgeon to adjust the gastric band if it moves later. The port can be used to introduce saline into the band to increase or decrease the constriction of stomach.
Whenever you eat after the surgery, the small pouch will fill up first, and you will get a feeling of fullness with just a small quantity of food. Later, the food will slowly empty into the main part of your stomach.
You can go home on the same day after the surgery.
Gastric bypass surgery
The duration of this surgery is 2 to 4 hours. For a gastric bypass surgery, the following steps will be taken after the laparoscope and instruments are placed inside your stomach:
- Your surgeon will use a laparoscopic staple to make a small pouch from the upper part of your stomach.
- In the second step, they will connect a small portion of the jejunum (middle part of the small intestine) to the pouch made from the upper part of the stomach through a small hole.
- The incision will be closed with sutures.
When you eat after the surgery, the food will first enter the pouch and then will go into the jejunum (small intestine) through the opening between these organs. This will cause less absorption of calories while also making you eat less.
Gastric bypass surgery can be also be done as an open surgery where one large surgical cut is made in the belly).
Post-surgery care: After gastric bypass surgery, you may be asked to stay in the hospital for 1 to 4 days. In the hospital, the following things can be expected:
- On the same day of the surgery, your doctor will ask you to sit on the bedside and walk a little.
- A catheter will be inserted through your nose into your stomach to remove fluid from the intestine (which may be present due to the surgery). It may be kept in for 1 to 2 days.
- A catheter may also be inserted in your bladder to drain urine.
- You will not be able to eat anything for the first 3 days after surgery. After that, you can slowly start with liquids and then soft or pureed foods.
- You will be asked to wear special stockings on your legs to prevent blood clotting.
- Your doctor will give you medicines like pain relievers through an intravenous (IV) line or by placing a catheter into your vein.
You will be allowed to go home when:
- You do not need pain killers
- You can move around without much pain
- You can eat food without vomiting
Gastric sleeve surgery
This surgery takes 60 to 90 minutes. After the laparoscope and instruments are placed in your stomach, the following steps will be taken:
- Using a laparoscopic stapler, the surgeon will divide your stomach to form a narrow vertical sleeve or a banana-shaped stomach.
- The rest of the stomach will be removed by cutting it.
- After this, the tools and laparoscope will be removed from your body, and cuts will be closed with stitches.
The new, smaller-sized stomach will limit the quantity of food you eat, thus making you fuller soon.
You can go home within 2 days after the surgery.
Biliopancreatic diversion with duodenal switch
The BPD/DS surgery is performed in the following manner:
- The surgeon will form a smaller, tube-like pouch by cutting a part of the stomach (vertically) using a laparoscopic stapler.
- The upper portion of the small intestine (the duodenum) will be divided and connected to the bottom portion of the small intestine (duodenal switch).
- The bypassed small intestine carries the bile and pancreatic enzymes that are needed for the digestion of fats and proteins. This portion is reconnected to the last part of the small intestine (biliopancreatic diversion).
- The surgeon will remove the tools and close the cuts with stitches or surgical glue.
This surgery can also be performed as open abdominal surgery.
After the procedure, when you eat, the food goes only through the new pouch and is emptied in the end part of the small intestine. Thus, less food is digested, and fewer nutrients and calories are absorbed.
You will be shifted to the hospital room after the surgery. The healthcare provider will ask you to get out of the bed and walk a little. During the hospital stay, you will be on a liquid diet.
How to care for yourself after bariatric surgery?
You may be asked to keep the following things in mind after the surgery:
Wound care:
- Keep the wounds dry and clean.
- Staples or sutures will be removed after 7 to 10 days of the surgery. Change the bandage (dressings) each day. If it becomes dirty or wet, change it frequently.
- You may have bruising around the wound. It will go away on its own.
- Avoid wearing tight clothes until your wound is healed.
- Avoid taking a shower until your next follow-up appointment unless advised otherwise by the doctor.
- If you are allowed to shower, avoid scrubbing, and let the water run on your cuts.
- Avoid soaking in a hot tub, bathtub or swimming pool unless allowed by your doctor.
- Press a pillow over the cuts when you need to sneeze or cough.
Diet care:
Your healthcare provider will explain your diet to you and ask you to avoid certain foods after the surgery.
- Eat only pureed or liquid food for the first 2 to 3 weeks.
- Slowly add soft food and then regular food to your diet.
- Avoid eating and drinking together. Keep a gap of 30 minutes between eating and drinking fluids.
- Avoid gulping; take small sips while drinking.
Activity:
Physical activity will help you to recover faster.
- If you have pain in your belly, try to get up and move around.
- Stop doing an activity if it starts aching.
- Avoid lifting anything heavier than 5 to 7 kg.
- Take short walks and go up and downstairs.
- Avoid activities that involve pushing or pulling.
Medicines:
Your healthcare practitioner will give you a few supplements to take daily. These include:
- Iron supplement
- Vitamins A, D, and K
- Calcium supplement
- Multivitamin
- Vitamin B12 supplement
After the surgery, you will start to lose weight rapidly in the first 3 to 6 months. You may experience:
These symptoms will go away when the body gets used to weight loss and till your weight stabilises. You will lose weight for up to 2 to 3 years. It can also improve your medical conditions.
When to see the doctor?
Call your healthcare practitioner if you have the following symptoms after the surgery:
What are the possible complications/risks of bariatric surgery?
Risks of anaesthesia and surgery include:
- Breathing problems
- Bleeding or blood clot formation
- Allergic reaction to medicines
- Heart problems
The common risks of bariatric surgery include:
- Stomach ulcers, heartburn
- Gastritis (inflamed stomach lining)
- Infection in the port used for gastric banding
- Poor nutrition
- Injury to organs (stomach, intestines, or others) during surgery
- Hernia (bulging of the tissue) at the incision site
- Kidney failure
- Acid reflux (digestive disease, stomach acid irritates the lining of the food pipe)
- Diarrhoea and cramping
- Vomiting from eating more than your stomach pouch can hold
- Scarring inside your belly that causes blockage in your bowel
You may need LAGB re-surgery if:
- The stomach slips up through the band
- The band erodes through the stomach
- The surgeon is unable to tighten or loosen the band
- Access port has flipped upside down
- Puncture in the tubing near the access port
Gastric bypass surgery has a risk of leakage from the line where parts of the stomach are stapled together.
Biliopancreatic diversion with duodenal switch causes difficulty in absorbing vitamins and minerals. It may cause:
- Protein malnutrition
- Calcium deficiency and iron deficiency
- Vitamin A, D, E, and K deficiency
- Thiamine deficiency
- Kidney stone
- Thinning bones
- Anaemia
When to follow up with your doctor after a bariatric surgery?
You will be asked to follow-up within a few weeks after the surgery. You will also need to consult your dietician and mental health provider who will help you to eat appropriately for the smaller size of your stomach and help you to deal with the concerns after the surgery, respectively. You may be asked to get some blood tests done to check the levels of vitamins and minerals in your body.
If you have had LAGB, you may need a follow-up to tighten or loosen the band if you are:
- Unable to lose weight
- Vomit after eating
- Have problems eating
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Find Gastroenterologist in cities
- Gastroenterologist in Gurgaon
- Gastroenterologist in Bangalore
- Gastroenterologist in Chennai
- Gastroenterologist in Jaipur
- Gastroenterologist in Ahmedabad
- Gastroenterologist in Noida
- Gastroenterologist in Mysore
- Gastroenterologist in Visakhapatnam
- Gastroenterologist in Hyderabad
- Gastroenterologist in Pune
Surgery Cost In Your City
Doctors for Bariatric surgery

Dr. Rishabh Gupta
Gastroenterology
6 Years of Experience

Dr. Paramjeet Singh.
Gastroenterology
10 Years of Experience

Dr. Nikhil Bhangale
Gastroenterology
10 Years of Experience

Dr Jagdish Singh
Gastroenterology
12 Years of Experience
References
- National Health Service [internet]. UK; Weight loss surgery
- National Institute of Diabetes and Digestive and Kidney Diseases [internet]: US Department of Health and Human Services; Bariatric surgery
- American Society for Metabolic and Bariatric Surgery [Internet]. Florida. UK; Bariatric Surgery Procedures
- Health direct [internet]: Department of Health: Australian government; Obesity symptoms
- Jensen MD, Ryan DH, Apovian CM, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. J Am Coll Cardiol. 2014;63(25 Pt B):2985-3023. PMID: 24222017.
- Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 20th ed. Philadelphia, PA: Elsevier Saunders; 2017
- Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 10th ed. Philadelphia, PA: Elsevier Saunders; 2016
- Stahl JM, Malhotra S. Obesity Surgery Indications And Contraindications. [Updated 2019 Feb 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan
- Stahl JM, Malhotra S. Obesity Surgery Indications And Contraindications. [Updated 2019 Feb 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan
- Mingrone G, Panunzi S, De Gaetano A, et al. Bariatric-metabolic surgery versus conventional medical treatment in obese patients with type 2 diabetes: 5 year follow-up of an open-label, single-centre, randomised controlled trial. Lancet. 2015;386(9997):964‐973. PMID: 26369473.
- Halperin F, Ding SA, Simonson DC, et al. Roux-en-Y gastric bypass surgery or lifestyle with intensive medical management in patients with type 2 diabetes: feasibility and 1-year results of a randomized clinical trial. JAMA Surg. 2014;149(7):716-726. PMID: 24899464
- Buchwald H, ed. Buchwald's Atlas of Metabolic & Bariatric Surgical Techniques and Procedures. Philadelphia, PA: Elsevier Saunders; 2012
- Johns Hopkins Medicine [Internet]. The Johns Hopkins University, The Johns Hopkins Hospital, and Johns Hopkins Health System; Roux-en-Y Gastric Bypass Weight-Loss Surgery
- University of Rochester Medical Center [Internet]. Rochester (NY): University of Rochester Medical Center; Biliopancreatic diversion with duodenal switch (BPD-DS) weight-loss surgery
- Mechanick JI, Youdim A, Jones DB, et al. Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient--2013 update: cosponsored by American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic & Bariatric Surgery. EndocrPract. 2013;19(2):337-372. PMID: 23529351
- Gloy VL, Briel M, Bhatt DL, et al. Bariatric surgery versus non-surgical treatment for obesity: a systematic review and meta-analysis of randomised controlled trials. BMJ. 2013;347:f5934. PMID: 24149519