Summary
A nephrectomy involves the surgical removal of kidneys, in part or whole. Kidneys are located behind the abdomen on each side. They play a crucial role in detoxifying the blood and eliminating the wastes generated in the body through urine. Nephrectomy is recommended in cases of cancer of the kidney and other conditions that severely affect kidney function. It is performed under general anaesthesia with the open or laparoscopic technique and may take one to three hours to complete.
- What is nephrectomy?
- Why is nephrectomy recommended?
- Who can and cannot get nephrectomy?
- What preparations are needed before nephrectomy?
- How is nephrectomy done?
- How to care for yourself after nephrectomy?
- What are the possible complications/risks of nephrectomy?
- When to follow up with your doctor after a nephrectomy?
What is nephrectomy?
Nephrectomy is a surgery in which a part of or whole of one or both kidneys is removed.
The kidneys are located on the flanks in the posterior part of the abdomen beneath the rib cage, shielded in part by the bottom two ribs and some muscles on the sides and back of the body. Each kidney is approximately four to five inches in length. The chief function of the kidneys is to remove waste products from the blood and generate urine for elimination outside the body.
Nephrectomy is generally done for renal (kidney) cancer, which most commonly affects one kidney (rarely, both kidneys) in people above the age of 60 years. This surgery is also done in case of kidney trauma or other health conditions that severely affect kidney function.
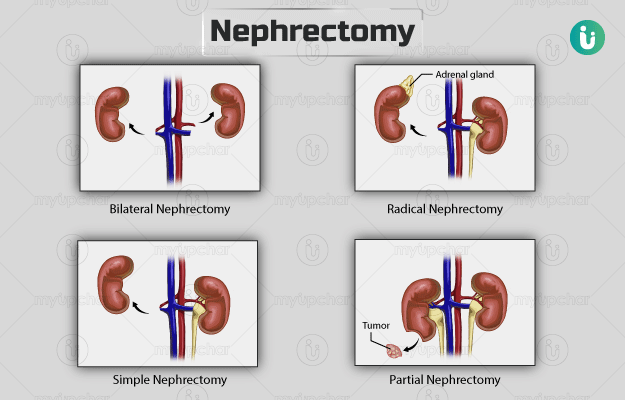
Based on the nature and spread of the condition, nephrectomy is of four types:
- Bilateral nephrectomy: Removal of both kidneys.
- Simple nephrectomy: Removal of one kidney.
- Radical nephrectomy: One kidney is removed along with the adrenal glands (a small gland located on top of each kidney, responsible for the production of vital hormones), lymph nodes, thin tube-like structure (the ureter, carries urine from the kidney to the bladder), and the layer of fat surrounding the kidney.
- Partial nephrectomy: The affected part of the kidney is removed, leaving the remaining healthy region intact to function as usual.
Nephrectomy can be performed in two ways:
- Open nephrectomy: The kidney is removed through a long cut to the abdomen.
- Laparoscopic (keyhole) nephrectomy: Three to four small incisions are made in the abdomen, and with the help of a laparoscope (a lighted, thin tube with a camera on its end) and surgical tools, the kidney is removed.
Why is nephrectomy recommended?
People with the following conditions can get nephrectomy:
- Kidney cancer and other cancers such as Wilm’s tumour
- Severe trauma to the kidney
- Non-cancerous conditions that affect kidney function. These can be due to:
- Symptomatic hydronephrosis (swelling of the kidneys due to retention of urine and failure to drain it to the bladders)
- Chronic infection
- Polycystic kidney disease (formation of fluid-filled sacs in the kidney that reduce their function)Kidney stones
- Hypertension
- Shrunken kidney
- For kidney transplant or in case of rejection of a kidney in a person who has had a kidney transplant
The signs and symptoms of kidney dysfunction or kidney cancer for which a nephrectomy may be advised are:
- Difficulty sleeping
- Lack of appetite
- Nausea and vomiting
- Muscle cramps
- Excessive urination or decreased urination
- Difficulty breathing
- Swelling in the ankles and feet
- Dry and Itchy skin
- Blood in urine
- Urine that appears foamy (excessive bubbles in the urine)
- Tiredness
- Pain in the kidneys
Who can and cannot get nephrectomy?
The conditions in which nephrectomy is contraindicated include:
- Coagulopathy (a bleeding disorder in which the blood is unable to form clots or coagulate)
- Severe impairment of lung and heart functions
- Sepsis (a life-threatening condition caused by infection)
The contraindications related to laparoscopic nephrectomy are:
- Incarcerated inguinal hernia (a condition in which a part of the intestine pushes out through a weak region of the abdomen and gets caught in the groin or scrotum).
- Severe obesity
- Strong post-surgical adhesions (scar tissue developed in abdominal tissues and organs after a surgery)
- Large hiatal hernia (the stomach pushes up into the chest cavity through an opening in the diaphragm). Read more: Hernia types
What preparations are needed before nephrectomy?
You may expect the following things before the surgery:
- A general health evaluation will be performed to assess your fitness for the surgery.
- Inform your doctor of your medical history including any allergies (if you have any), and if you have had any surgeries earlier.
- Tell the doctor about all medications that you take, including prescribed or non-prescribed medicines or blood thinners (e.g., aspirin and warfarin) as they may need to be discontinued before surgery. Continue taking your regular medicines unless advised by the doctor.
- Stop smoking, as it can worsen some conditions and increases the risk of complications after surgery.
- Inform your doctor if you have any stents, implants, pacemaker, transplants, or other foreign bodies inserted in your body.
- Your blood pressure, height, weight, pulse, and lung function will be recorded and your doctor will ask you to get some blood and urine tests done.
- X-ray and electrocardiogram will also be done to assess your fitness for the surgery.
- In the weeks leading to your surgery, eat a balanced, healthy diet.
- Do adequate exercise, such as brisk walks for about 20 to 30 minutes each day. This prepares the cardiovascular system to cope better with any surgical challenges.
- Inform your doctor if you are suspecting a pregnancy.
- You can consume your meals normally on the day before your surgery. In order to give you nourishment and a better recovery, you may be given a high carbohydrate drink that must be consumed after meals.
- Do not eat or drink anything after midnight the night before the surgery. Food or liquids in the stomach can make its way up and can damage the lungs under the effect of anaesthesia.
- You need to take an enema on the evening before your surgery to clear your bowels before the procedure.
- You will be asked to sign a consent form for the surgery.
Consider the following things while going to the hospital on the day of the surgery:
-
All ongoing medication with the packaging should be carried to the hospital. Carry an extra set of clothing, nightwear, toiletries, and slippers with you to the hospital. Do not wear any jewellery, makeup, contact lenses, dentures, and other prostheses.
How is nephrectomy done?
Before the surgery:
You will be asked to change into a hospital gown and will be administered with a blood thinner injection to reduce blood clots during surgery and an antibiotic injection. You will also be provided with special leg stockings to reduce the chances of blood clots. An anaesthetist will discuss the anaesthesia and other pain management options with you. The procedure is generally carried out under general anaesthesia (the person is put to sleep).
Before the surgery, a tube will be introduced into your stomach through your nose (nasogastric tube) it is used for nutritional support and remove any excess fluids from stomach. An intravenous drip will be placed to give you fluids to prevent dehydration. A catheter will be inserted into your bladder to track the urine output. These tubes will be removed a few days after the surgery.
Broadly, nephrectomy can be performed using two surgical approaches:
Conventional open nephrectomy
The treatment of choice for kidney cancer that has not spread (localised) and for irreversible kidney damage is open nephrectomy.
Simple nephrectomy:
- You will be made to lie on your side bent at the waist on an angled table if the surgery is performed from the side to give better access to the kidney.
- A surgeon will cut your skin and muscle and, If required, remove some region of your ribs to access your kidney.
- He/she will then move aside the nearby organs.
- The surgeon will tie up and cut the blood vessels of your kidney and ureter and gently lift y the affected kidney out of your body.
- Finally, the surgeon will suture the lower layers of the incision. The upper layer may be either sutured or stapled.
Radical nephrectomy:
-
The procedure for radical nephrectomy is largely similar to the one described above. However, a larger incision will be made across the front of your abdomen that may extend to the base of your chest. Here, the kidney and neighbouring lymph nodes and adrenal glands are removed.
The procedure may take one to three hours to complete and may require a hospital stay of five to seven days.
Laparoscopic nephrectomy:
This procedure can be performed using a transperitoneal (from the front side of the abdomen) or retroperitoneal (from the backside of the abdomen) approach.
- In the transperitoneal method, the surgeon will make an incision on your abdomen and inflate your abdomen with carbon dioxide for better visibility of your organs. He/she will then make three to four more cuts in your abdomen, to insert instruments for the surgery,
- In the retroperitoneal method, the surgeon will make a small cut on your back, and push a small balloon in to create space. The balloon will be removed, and carbon dioxide will be introduced to fill the space. Thereafter, two or three small incisions will be made in your back for other instruments.
- Through the openings, the surgeon will insert a laparoscope, which is a thin tube with a light and camera on the end in your abdomen. The procedure is facilitated by pictures received from the camera that the surgeon can use to visualise the kidneys and surrounding tissues.
- Using the instruments, the surgeon will dissect your affected kidney from the surrounding tissues and blood vessels and place it in a small bag, which is removed by widening one of the incisions. Alternately, the surgeon will break down your affected kidney into pieces in the bag and then removed through one of the incisions.
- Finally, the surgeon will close the incisions with clips or absorbable stitches that disappear within two to three weeks. You may be given a local anaesthetic to relieve pain.
- The entire procedure takes one to three hours until complete. You will likely be discharged after three days.
After your surgery, you will be moved to the recovery room until the effect of anaesthesia wears off. Then, you will be shifted to the ward.
You will have:
- An oxygen mask that gives you oxygen for the initial one or two days.
- A drain at the wound site to drain fluids collected after the operation.
- A dressing placed on your sutured openings.
Your temperature, blood pressure, pulse, and oxygen levels will be frequently checked. You will wear the support stockings on your legs to prevent blood clots from forming. You may receive medications to avoid blood clots and for pain. You will be encouraged to mobilise as it reduces the formation of blood clot and chest infection. You should be able to have a light meal the day after surgery to initiate normal bowel movements that may be sluggish initially.
Discharge from hospital:
- You will be discharged only after you eat, drink, resume bowel movement, and walk independently.
- Pain medicines will be prescribed to you.
- You will be taught to administer blood clotting medications to yourself before discharge, which you may be asked to continue for about 28 days.
How to care for yourself after nephrectomy?
While at home, you would be asked to keep the following things in mind:
- Avoid strenuous exercises or heavy lifting for six weeks.
- You can bathe as normal as there is no dressing involved.
- Avoid driving for two to three weeks to reduce pressure to the surgical site.
- Be active to reduce blood clots in the legs. Slowly increase the exercise starting with short walks and mild exercise.
- Eat a healthy diet with many fluids, fresh vegetables and fruits to keep your bowels regular.
Work can be resumed after two to three weeks. You may be allowed to resume sexual activity three to four weeks after the surgery. It is normal to feel tired and emotional after the surgery for the first couple of weeks.
When to see the doctor?
You should visit a doctor immediately if you experience:
- Abdominal pain, vomiting, or nausea
- Cough, breathlessness, or signs of flu
- The surgical site does not show signs of improvement or develops redness, tenderness, fluid leak, and swelling
- Fever
- Chest pain
- Inflammation, redness, and pain in your calves
- Burning sensation while urinating
What are the possible complications/risks of nephrectomy?
The type of nephrectomy and the surgical procedure (open or laparoscopic) determine the risks or complications involved. The risks include:
- Injury to the surrounding organs, namely the liver, spleen, blood vessels, lungs, among others which require further surgery.
- Temporary reduction in lung function.
- Lowered kidney function (temporary), in case of partial nephrectomy.
- Anaesthesia-related concerns or cardiovascular problems (chest infection, clots in the lungs, heart attack, or stroke) requiring transfer to the intensive care unit.
- Lung cavity puncture or damage during surgery leading to a collapsed lung.
- Bleeding from the surgical site opening or within the abdomen.
- Wound infection.
- Nerve injury near the region of the surgery.
- Bowel movements may be affected in the first few weeks after the surgery.
- In partial nephrectomy, if the tumour is extensive, the entire kidney will need to be removed. In such cases, there may be a risk of urine leakage into the abdomen.
- Formation of blood clots in the legs (deep vein thrombosis).
- In laparoscopic nephrectomy, there will be abdominal bloating and shoulder tip pain and Injury to the bowel.
- In the case of keyhole surgery, hernia or infection at the site of the openings.
When to follow up with your doctor after a nephrectomy?
You will have a follow-up visit in one or two weeks after the surgery. The doctor will remove stitches if needed, assess the surgical site and advise you on resuming your normal activities.
Disclaimer: The above information is provided purely from an educational point of view and is in no way a substitute for medical advice by a qualified doctor.
Surgery Cost In Your City
References
- Harvard Health Publishing. Harvard Medical School [internet]: Harvard University; Nephrectomy
- NHS Scotland [Internet]. National Health Service. UK; Nephrectomy: a guide for patients and family
- University Hospital Birmingham [Internet]. NHS Foundation Trust. National Health Service. UK; Open and laparoscopic nephrectomy
- Royal Berkshire Hospital [internet]: NHS Foundation Trust. National Health Service. U.K.; Nephrectomy (kidney removal): information and advice for patients on the enhanced recovery programme
- American Kidney Fund [Internet]. Maryland. US; Symptoms of kidney disease
- National Kidney Foundation [Internet]. New York (NY). US; 10 Signs You May Have Kidney Disease
- National Institute For Health and Care Excellence [Internet]. London. UK; Laparoscopic nephrectomy (including nephroureterectomy)