Summary
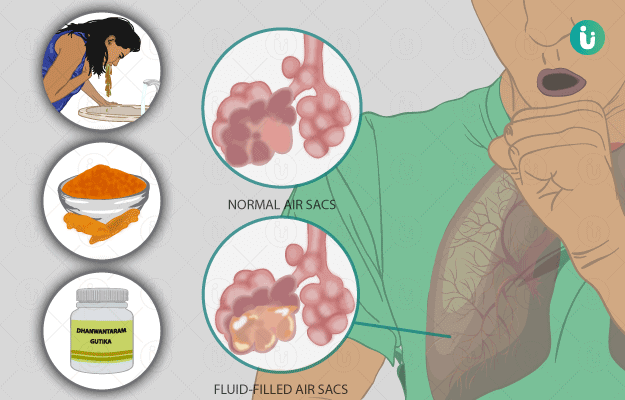
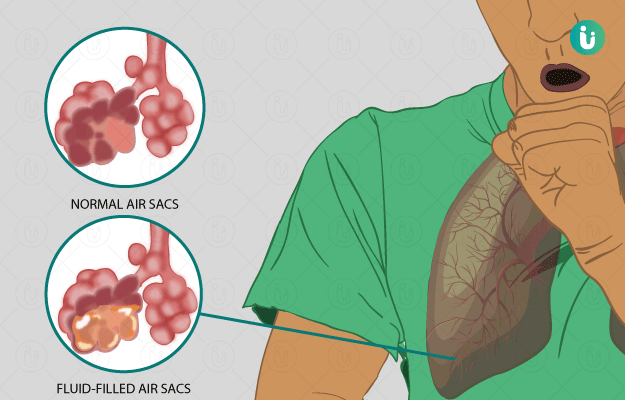
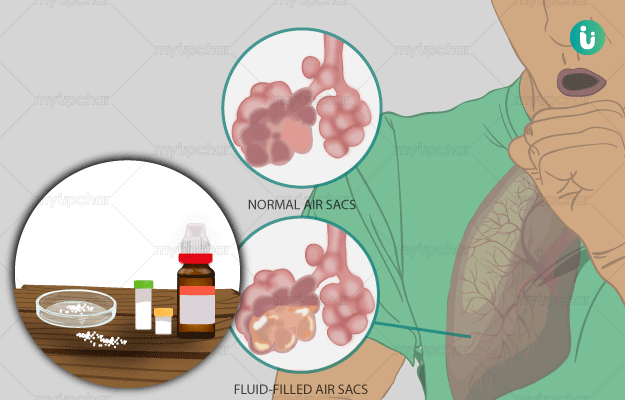
Phlegm is a thick, slimy, fluid produced by the cells of the linings of the lungs and upper airways. It is produced in the body as one of the defence mechanisms and is medically termed as mucus. But, when a person is healthy, the mucus is thin in consistency; hence, it is unnoticeable. During certain illnesses, mucus thickens to trap dust particles and infectious agents such as bacteria. Phlegm may have an unusual odour and colour to it in the case of an underlying disease and needs to be investigated. It might be produced in excess in illnesses such as common cold, upper respiratory tract infection, chronic obstructive pulmonary (lung) disease (COPD), allergy, asthma, pneumonia, and lung cancer. Diagnosis of abnormal phlegm is usually done by taking a chest X-ray or CT scan, microscopic and culture examination of the phlegm along with some blood tests to confirm the same. Treatment protocols depend upon the underlying cause and vary from person to person. Prevention of phlegm is not possible as it is a naturally produced fluid in the respiratory tract.

 Doctors for Phlegm
Doctors for Phlegm  OTC Medicines for Phlegm
OTC Medicines for Phlegm
 Lab tests for Phlegm
Lab tests for Phlegm Phlegm articles
Phlegm articles
 Ayurvedic Treatment of Phlegm
Ayurvedic Treatment of Phlegm
 Home Remedies for Phlegm
Home Remedies for Phlegm
 Homeopathic Treatment of Phlegm
Homeopathic Treatment of Phlegm




































 Editorial Team
Editorial Team
 Dr. Rachita Narsaria
Dr. Rachita Narsaria

 Dr. Laxmidutta Shukla
Dr. Laxmidutta Shukla